3-D mammograms are popular, but are they better than 2-D?
Gold standard trials comparing breast cancer screening methods are just getting under way
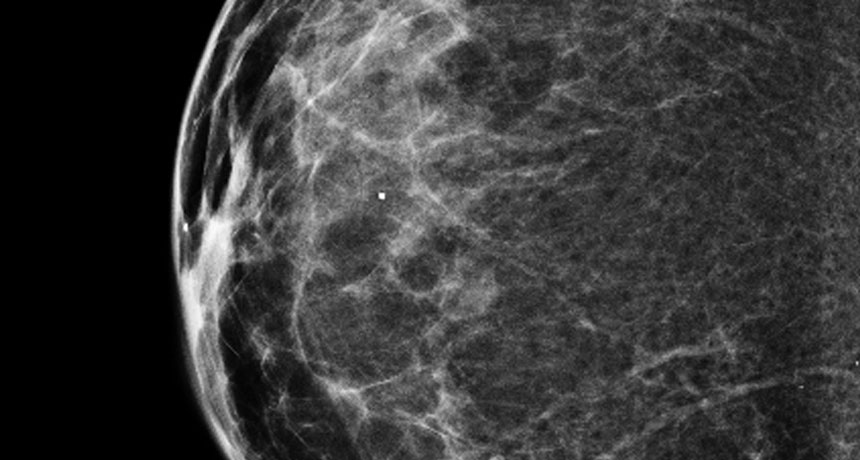
ALL CLEAR This 3-D mammogram shows a normal breast. Initial studies suggest that the technology is more sensitive than traditional 2-D imaging, but it’s unclear if that helps reduce the number of deaths from breast cancer.
National Cancer Institute, National Institutes of Health/Flickr (CC BY-NC 2.0)
In recent years, women getting a mammogram have had a new decision to make: 2-D or 3-D?
Some breast-care centers have touted the newer 3-D mammography technology as more accurate. But while initial research suggests that it may be a more sensitive diagnostic test, evidence that the technology actually reduces the number of deaths from breast cancer better than 2-D imaging is lacking.
Even so, use of this technology has skyrocketed in recent years, according to a new analysis of private insurance data. Also known as digital breast tomosynthesis, three-dimensional mammography was the primary screening method in 43.2 percent, or 763,982 out of close to 1.8 million exams in a private insurance database in the second half of 2017, researchers report online June 24 in JAMA Internal Medicine. That’s up from only 12.9 percent, or 187,885 out of about 1.5 million, in the first half of 2015.
Both 3-D and 2-D imaging methods rely on X-ray technology. And a woman undergoing either method experiences breast-squeezing discomfort. But three-dimensional mammography takes images from many different angles around the breast, which a computer then combines to make a 3-D image. The standard 2-D mammography, which usually takes images from two angles, offers a flat image of the breast. When 3-D screening is used, the radiologist gets both a 3-D and a 2-D image.
The U.S. Food and Drug Administration, which approves medical devices, gave 3-D mammography the green light in 2011. But the American Cancer Society and U.S. Preventive Services Task Force don’t yet recommend the new technology for routine screening, citing lack of evidence.
Initial research suggests that three-dimensional imaging reduces the mammogram recall rate — how often a radiologist identifies a suspicious result that needs follow-up imaging. Higher recall rates are associated with increased false-positives, when a radiologist thinks a woman may have cancer but further screening shows she doesn’t (SN: 6/28/14, p. 22). Some liken a 3-D screening to having the follow-up test during the initial mammogram, says Ilana Richman, a general internist at Yale School of Medicine. The idea is that the 3-D images provide the radiologist with more information, making it easier to distinguish normal from abnormal areas. This saves women the time, cost and stress of another screening, says Richman, a coauthor on the JAMA insurance analysis paper.
A 2014 JAMA study that looked at more than 450,000 mammograms and compared those taken with 2-D versus 3-D imaging found a statistically significant reduction in the rate of screening recalls. There were 107 recalls per 1,000 screenings after 2-D imaging versus 91 per 1,000 for 3-D imaging, the researchers report.
The newer technology may also be more sensitive, research suggests, which means that 3-D imaging may catch more cancers. In the 2014 JAMA study, the cancer detection rate improved from 4.2 cancers per 1,000 cases for 2-D imaging to 5.4 cancers per 1,000 cases with 3-D imaging, also statistically significant.
But if the diagnosed cancer didn’t need to be found, because it would never have caused health problems, it can lead to unnecessary and potentially harmful treatments. “Finding more cancer sounds good,” Richman says. “But we know from a long history of screening in breast cancer and other cancer types that not every cancer is one that we need to worry about.”
Early findings in favor of 3-D mammography have come from observational studies or after-the-fact analysis. Now, several randomized controlled trials in which women are randomly assigned a screening method, allowing researchers to make a direct comparison, are under way. These trials “should provide more clarity about the benefits and harms of digital breast tomosynthesis over the next few years,” says Joy Melnikow, who heads the Center for Healthcare Policy and Research at the University of California, Davis in Sacramento, and wrote an accompanying editorial in the same JAMA Internal Medicine issue.
One, called the Tomosynthesis Mammographic Imaging Screening Trial, or TMIST, has begun enrolling, with a goal of 165,000 women in total. It will assess whether the 3-D technology reduces the number of women diagnosed with advanced breast cancers, those most likely to spread to other parts of the body and cause death. The trial measure is a proxy for improvements in breast cancer mortality rates.
If it turns out that 3-D mammography isn’t more beneficial, the fact that it’s already gained such popularity means that “it will likely take some years for its use to decline,” Melnikow says. That could mean unnecessary diagnoses and treatments.
And if evidence does support the use of the new technology, the way that the technique has spread could be a problem. Richman and her colleagues found that 3-D imaging was primarily employed in higher income areas that have a larger percentage of white residents, which largely held true when the researchers looked at Medicare insurance data, too. This pattern of use could widen existing racial disparities in breast cancer mortality, Melnikow says.