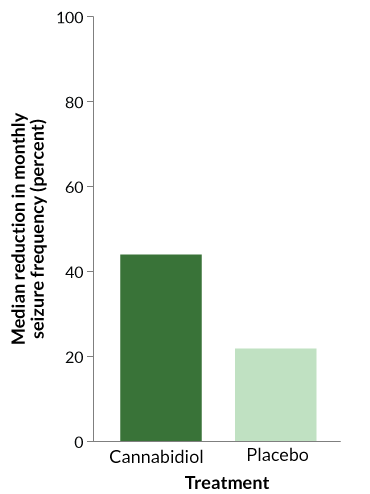The CBD boom is way ahead of the science
Strict regulations have stunted research on cannabidiol, but that hasn’t hampered product popularity

This shop in Fort Lauderdale, Fla., offers CBD-infused pizzas and smoothies, a growing trend as companies tout the oil’s ability to treat anxiety, depression, pain and more.
Jennifer Lett/Associated Press
A few months back, a new storefront appeared in my small Oregon town. Its shelves were packed with tinctures, jars of salve, coffee beans, bath bombs — even beard oil. This motley collection shared a single star ingredient: CBD.
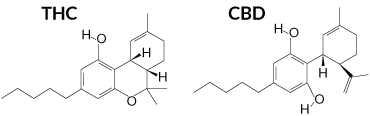
Produced by the cannabis plant, CBD is the straitlaced cousin of marijuana’s more famous component — the THC that delivers a mind-swirling high. CBD, or cannabidiol, has no such intoxicating effects on the mind. Yet the molecule has captured people’s attention in a profound way, sold as a remedy for pain, anxiety, insomnia and other ailments — all without the high.
That neighborhood shop, CBD Scientific, is far from alone in its efforts to sell people on the benefits of CBD, which is found in both marijuana and hemp, two versions of the Cannabis sativa plant. CBD is popping up in products in pet stores, coffee shops and the health and beauty sections of mainstream grocery stores. It’s even being brewed into beer. I left the shop with a $5 bottle of water infused with “5,000,000 nanograms” of CBD.
So far, messages of CBD’s purported health benefits come from people trying to sell CBD products — not from scientists, says Margaret Haney, a neurobiologist who directs the Marijuana Research Laboratory at Columbia University. A gaping chasm separates the surging CBD market and the scientific evidence backing it. While there are reasons to be excited about CBD, the science just isn’t there yet, Haney says.
Scientists still don’t know all of the targets CBD hits in the human body, nor what effects it may have, if any. With the exception of tests in people with rare forms of epilepsy, large studies that compare CBD with placebos in people are rare. Much of the existing research was done with cells in the lab or in lab animals, with results that don’t necessarily translate to people.
And there’s always the chance that for some people, CBD’s magic is made not by the compound itself but by a powerful placebo effect; people who expect good outcomes are more likely to see benefits.
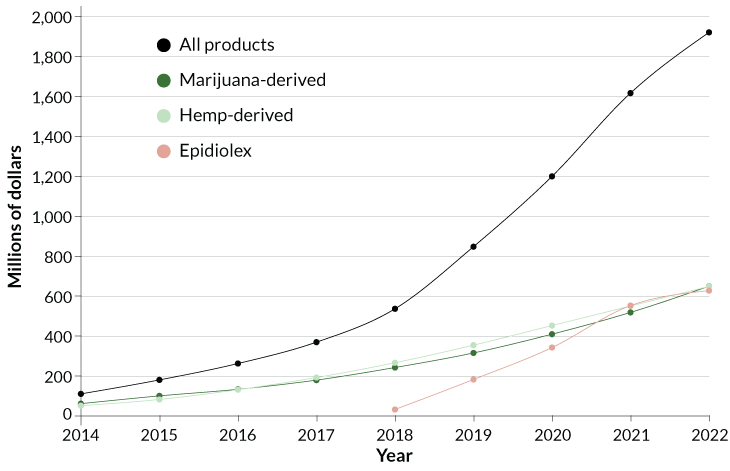
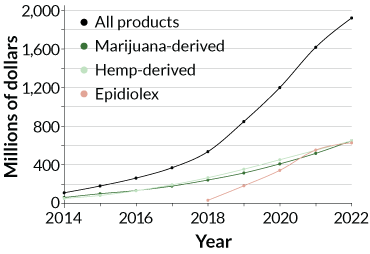
Researchers are stepping into the void, lured by promising early data. Small trials are under way looking at the effect of CBD on anxiety, pain, opioid addiction, depression and other health problems. National Institutes of Health funding for CBD studies went from zero in 2014 to an estimated $16 million in 2018.

“We’re very interested in CBD,” says Susan Weiss, director of the Division of Extramural Research at the National Institute on Drug Abuse in Bethesda, Md. Still, she urges caution to people eager to try CBD. Because of lax oversight, there’s no telling what’s inside many of those tinctures, oils, rubs and foods for sale online and in stores. “A lot of the products that people are taking may not be what they think,” she says.
Despite the risks and warnings, it seems safe to say that the collective fascination with CBD isn’t going to wear off anytime soon. “People think it’s great for everything,” says cognitive neuroscientist Kent Hutchison of the University of Colorado Boulder. That can’t possibly be true, he says. “But I do think it’s going to be great for some things. We just need to figure out what those things are.”
Mystery molecule
Each morning, Samantha Montanaro of Portland, Ore., drops a CBD tincture under her tongue. “I’m kind of testing out my own body with this,” she says. “I’m finding that it really helps with anxiety and stress.”
Montanaro isn’t alone; CBD testimonials are increasingly easy to find. In 2016, Montanaro, now 35, cofounded Tokeativity, a global cannabis community for women. Back then, “CBD wasn’t even a thing,” she says. But the first sparks of the CBD movement caught fire fast. “It’s been pretty crazy to watch how things have evolved,” she says. Some bullish analysts predict that the CBD market in the United States will balloon from hundreds of millions of dollars in 2018 to almost $20 billion by 2022.
Ziva Cooper directs UCLA’s Cannabis Research Initiative and fields a lot of questions about CBD. Her answers invariably disappoint. “When I tell [people] we don’t have very much evidence in people, they’re actually surprised,” she says. When it comes to CBD’s benefits, “there’s actually very little out there to hang our hats on.”
The one exception is for rare forms of childhood epilepsy. Neurologist Elizabeth Thiele of Massachusetts General Hospital in Boston had a young patient who was having over 100 seizures a day. After other treatments had failed, the boy’s parents began searching for a source of CBD oil, which they desperately wanted to try after learning about promising early results in animals. The family flew to England, so the boy could try the CBD formulation made by GW Pharmaceuticals. The child’s results, Thiele says, were remarkable. After a week of CBD, his daily seizures had fallen to single digits.

That result ultimately led to clinical trials, one of which included 171 people, mostly children, with Lennox-Gastaut syndrome, a rare and severe seizure disorder. In addition to their normal medication, half of the participants got doses of CBD that were rigorously tested and standardized by the drug’s maker. The other half received their regular treatment plus a placebo. After 14 weeks, the people taking CBD saw a median drop in monthly seizure frequency of about 44 percent; seizures in people who took the placebo dropped almost 22 percent. Thiele and her colleagues published those results in March 2018 in the Lancet.
Side effects were manageable, the researchers found. Diarrhea, sleepiness, poor appetite and vomiting were more likely to occur in the people who took CBD than in those who got the placebo. Along with results from several other trials, those data were strong enough to prompt the U.S. Food and Drug Administration to approve the CBD drug, called Epidiolex, last June.
Despite rigorous testing of Epidiolex, big gaps in knowledge on how the drug works in epilepsy remain. Researchers don’t know how CBD tames seizures. Because the molecule comes from cannabis, the early assumption was that CBD latches onto the same chemical receptors that THC connects to, one primarily in the brain and one mainly on immune cells. It turns out, however, that CBD doesn’t seem to hit either of those receptors.
Instead, studies in rats and mice point to two different targets. One, called TRPV1, is known to play a role in pain sensation and maybe epilepsy, too. The other, called GPR55, might change the activity level of nerve cells in the brain, a feat that may be behind CBD’s antiseizure power.
Scientists also don’t know whether CBD keeps working year after year. For some of Thiele’s patients, CBD seems to still be effective after five years of taking the drug, even allowing them to taper off some of their other medications, she says. But data from 92 other patients, presented in December at the American Epilepsy Society’s annual meeting, suggest that CBD’s benefits can start to fade after about seven months on the drug. About a third of the people in the study needed a dose increase after their CBD doses became less effective, researchers from Tel Aviv Sourasky Medical Center reported.
Research on CBD and other ailments lags way behind the epilepsy work. Early experiments, mostly on lab animals but some in small numbers of people, suggest that CBD might fight anxiety, ease schizophrenia symptoms and address pain.
One example: Healthy men who took CBD before a stressful public speaking task were calmer than those who took a placebo, researchers reported in October in the Brazilian Journal of Psychiatry. But only the 15 men who received doses of 300 milligrams were more relaxed. The 27 who took less or more CBD didn’t see benefits. Other types of studies with people, and studies of mice and rats, have turned up antianxiety effects, too. But most of these studies looked at single doses of CBD, not consistent use.
Early evidence of CBD’s promise against schizophrenia comes from a trial of 88 people with the disorder. After six weeks, people who had received a big daily dose of CBD (1,000 milligrams a day) in addition to their normal medication had more improvements in certain symptoms when compared with people who received a placebo. Those results hint that CBD might be a new type of drug for schizophrenia, researchers wrote in March 2018 in the American Journal of Psychiatry.
Studies in lab animals suggest that CBD may help relieve chronic pain. A study appearing in 2017 in Pain found that CBD could block osteoarthritis pain and nerve damage in rats. Hard data for humans are harder to find, but anecdotes abound. Pain clinician Kimberly Mauer of Oregon Health & Science University in Portland and colleagues at the OHSU Comprehensive Pain Center have seen an uptick in patients who say they’re taking CBD. Their experiences are mixed, she says: “About half the patients say they get some benefit, and about half say they didn’t notice anything.”
No easy access
To answer the many outstanding questions about CBD’s effects, scientists need access to the compound. But a complex web of U.S. regulations makes that difficult. CBD is subject to rules from both the FDA and the U.S. Drug Enforcement Administration. CBD produced by the marijuana plant remains on the DEA’s list of the most restrictive class of drugs, Schedule 1, alongside LSD, ecstasy and other drugs deemed to have no accepted medical use and high potential for abuse. Access restrictions on industrial hemp, and by extension, the CBD that comes from hemp, were eliminated in the 2018 Farm Bill, signed into law in December. However, regardless of its provenance, CBD is still subject to FDA regulations, as well as any regulations imposed by states.
“As easy as it’s gotten for the average person to go legally to buy recreational marijuana and consume it in many states, it’s gotten harder for scientists,” says Haney at Columbia. One of the few approved sources of CBD is a government-sanctioned cannabis facility at the University of Mississippi in Oxford. After she gets the CBD she needs for her studies, Haney is required to meticulously account for every milligram. “I have a gun safe in a locked room that I get into with my fingerprints to store both cannabidiol and marijuana.”
With those restrictions, many scientists just can’t do the studies they want, Hutchison says. “The whole thing is a little bit crazy. People can sell it everywhere, but it’s very difficult for scientists to study its effects in humans.”
Hutchison and colleagues have figured out a legal work-around that doesn’t require researchers to obtain supplies of CBD. The team is avoiding the government-grown cannabis, which can be quite different from the products in circulation, by testing the effects of the cannabis products that people are actually using. To do this, the researchers created a mobile pharmacology lab they call the CannaVan. The tricked-out Dodge contains equipment to study people after they’ve taken a product containing CBD (or THC) that they bought themselves. The researchers are currently collecting data on CBD’s effects on anxiety and pain.

Buyer beware
FDA rules say that CBD cannot be legally added to food and sold across state lines, sold as a dietary supplement or marketed with claims of treating diseases. But aside from sending some warning letters, the FDA has, so far, let the marketplace run uninhibited. (Some local health authorities, however, are beginning to flex their might, warning restaurants in New York City, for instance, to take CBD off the menu.)
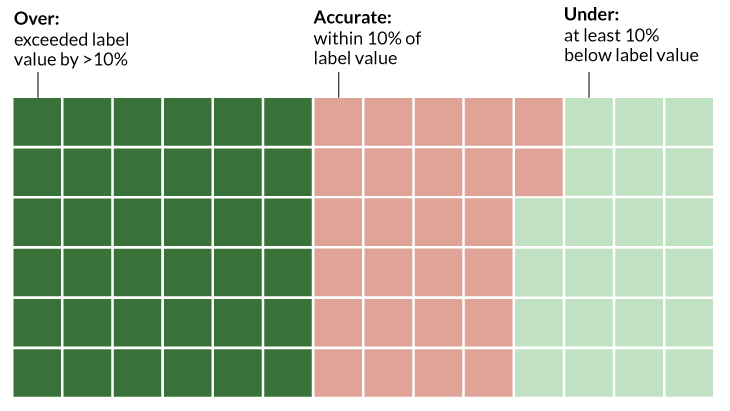
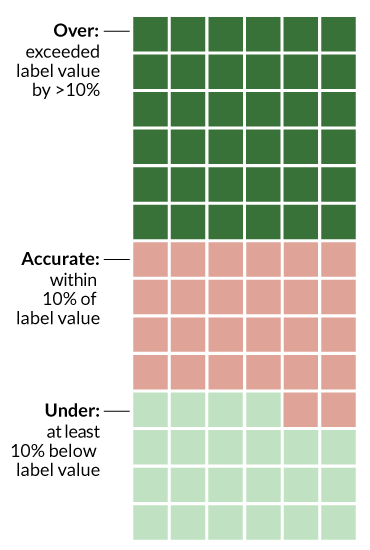
Overall, no one really knows what’s inside the bottles, rubs and coffees for sale. A study published in 2017 in JAMA gives a sense of the problem. Researchers ordered and tested 84 products sold online in 2016 as CBD-containing products. Of those, only 26 were labeled accurately (containing CBD within 10 percent of the claimed amount); 36 of the products had more CBD than their labels said; and 22 products had less. The researchers also found THC in 18 of the 84 samples.
Sophie Cloyd is a 30-year-old manager for the CBD company Ablis of Bend, Ore. She is also pregnant. I met her recently at a ski lodge, where she was offering beverage tastes and describing tinctures, oils and lotions. CBD, she says, has helped her manage this pregnancy, her second. She was prescribed the anti-nausea drug Zofran early in her pregnancy, but “the research on Zofran scared me more than the lack of research on CBD,” she says.
Ablis, which makes CBD-infused fizzy drinks and other products, currently gets purified CBD from Colorado, Cloyd says. When the CBD arrives, the company sends it to an independent lab to confirm that it has the right amount of CBD, no pesticides and no THC. But not all CBD sellers test their products.
An unexpected THC dose might not be enough to get a user high, but it could still be a problem, as news reports have begun to point out. To ease his pain from psoriatic arthritis, a school bus driver in Beaverton, Ore., had been taking a daily dose of CBD oil. In early 2018, he failed a periodic drug test with high THC levels, which caused him to lose his job, Portland news channel KATU reported. Even seemingly small amounts of THC can build up in the body with repeated use.
A product might contain even worse surprises. Between December 2017 and January 2018, for example, 52 people fell ill in Utah, with symptoms such as hallucinations, vomiting and seizures, after taking what they thought was CBD. It turned out that the products, many labeled “Yolo CBD oil,” contained a synthetic cannabinoid, and it had poisoned them.
Even if product labels were always accurate, people have no idea of the correct dose of CBD (assuming the right dose would be effective). “You see it marketed in doses like 10 milligrams,” Hutchison says. “Well, 10 milligrams probably does nothing.” For comparison, people who participated in one Epidiolex study took 20 milligrams per kilogram of body weight. To reach that daily dose, I’d need to chug 254 bottles of that 5 million nanogram CBD water I bought — at a cost of $1,270.
Haney makes the same point: “You’re not getting anything resembling an effective dose when you get CBD added to your coffee, or you buy a mint with a little bit of CBD in it,” she says.
There’s even less known about CBD products that you rub on your skin. Scientists don’t know that CBD in creams, oils and ointments actually makes it into the body. “I’m not convinced that anything you’re rubbing on your body with CBD is even getting through,” Haney says.

At its heart, the trouble is that most CBD use isn’t backed up by science, Haney says. “I am not against CBD,” she says. In fact, she is about to start a study looking at CBD to treat nerve pain due to chemotherapy in cancer patients. “But I don’t like marketers determining what it’s good for and what it’s not.”
Hype run amok isn’t anything new, says Mauer, the OHSU pain doctor. Consumers try lots of things before the science is definitive — keto diets, for instance, or vitamin D supplements (SN: 2/2/19, p. 16). And even if it turns out that the chemical doesn’t work, the placebo effect might be enough to help reduce symptoms.
So far, the science on CBD isn’t mature enough to weigh in, one way or another. But judging by the number of studies and clinical trials under way, this nascent research field is growing up fast, seeking to quickly fill the space between the science and what people want to know.
This research boom heartens Montanaro. Her message to the scientific community: “I would encourage curiosity,” she says. “I’m not a doctor, and I’m not a scientist, but I certainly know my own body,” and she says that CBD helps her. From her perspective, science has got some catching up to do.
This story appears in the March 30, 2019 issue of Science News with the headline, “The Allure of CBD: People seek health benefits despite lack of evidence.”