Spin City
Fiber technique fuels materials research
In 1934, Anton Formhals patented a spinning technology that produced synthetic fibers with the aid of an electric field. Introduced shortly before the advent of nylon, Formhals’ electrospinning technique never caught on. The method’s output couldn’t compete against the large-scale fiber-spinning methods that later made nylon and polyester into industrial commodities.


The basic premise behind commercial fiber manufacturing has remained largely the same for decades. Most methods force molten or chemically treated polymers through showerhead-resembling devices called spinnerets, following the same strategy as a child’s Play-Doh pasta maker. Advances in such extrusion technologies have shrunk the diameter of fibers in all manner of fabrics to micrometer and sub-micrometer ranges.
Although the fiber diameters have shrunk, the equipment hasn’t. Industrial fiber-spinning machinery resembles a “big block of iron the size of a dining room table,” says polymer scientist Darrell Reneker of the University of Akron in Ohio.
Among researchers who want to study fiber technology on their laboratory benches, there’s been a revival in interest in Formhals’ technique. The method requires no specialized equipment. “You can have an experiment going in an hour with a few simple components,” says materials scientist Gary Wnek of Case Western Reserve University in Cleveland.
The room-temperature spinning process works because the polymer chains get knotted up during spinning. That tangling holds together a fiber that then is laid down as a mat.
In the new work, scientists often add extra molecules into their polymer mix. “You can put any kind of small molecule in there and spin it at the same time as the fiber,” says polymer scientist John F. Rabolt of the University of Delaware in Newark. The additions can include proteins or drugs that wouldn’t survive the high-heat processing and might not withstand the chemicals used in conventional fiber-extruding methods.
The flexibility of the technique points to a wide range of applications for the resulting fibrous mats, “primarily in the area of biomedical technology,” says chemist Timothy E. Long of Virginia Polytechnic Institute and State University in Blacksburg.
Researchers are already electrospinning potential innovations in drug delivery, wound dressing, and tissue engineering.
Spin specs
Electrospinning starts with a syringe filled with a polymer solution. The terminals of a voltage generator are attached to the syringe’s metal needle and to a metal plate, which sits about 20 centimeters below the tip of the syringe’s needle. The generator creates a voltage difference between the needle and the plate.
Although the syringe has a plunger, electrospinning isn’t an extrusion method. The plunger forces out just enough polymer to create a drop at the needle tip. Surface tension initially holds together the drop, explains Reneker, but the electric forces have the opposite effect. “We can make the electric forces win,” he says.
In most setups, the voltage generator creates positive ions in the polymer solution, explains Wnek. As the ions start to repel each other, the repulsive force pulls the drop into a cone shape. At some critical voltage, this force becomes greater than the surface tension, and a thin jet from the cone heads toward the negatively charged plate. The critical voltage—in the range of thousands to tens of thousands volts—depends on factors such as the concentration of the polymer solution and the polymer’s molecular weight.
Once launched, the fluid jet takes a circuitous route to the metal plate. Because of jostling among ions in the material, as the jet elongates, it begins to coil into a spiral, says Reneker. As the segments of the spiral itself continue to elongate, the jet becomes unstable and generates smaller coils: spirals within spirals. While the jet elongates, the solvent evaporates. “What you collect are those now-solid polymer coils coming down in a seemingly disorganized way,” says Reneker.
As the fiber lands on the plate, it forms a mat that “looks like tissue paper,” Rabolt says. “You can generally peel it off,” he adds.
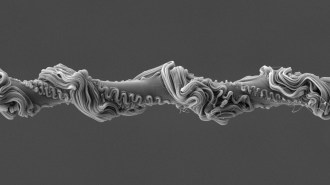
Under an electron microscope, the mat “looks like Pick-Up Sticks,” Rabolt says. A fiber’s diameter can range from about 100 nanometers to several micrometers.
Although setting up an electrospinning experiment is a breeze, researchers are just beginning to understand the complicated combination of physics, fluid mechanics, and polymer science that produces these micro- and nanoscale fibers. Figuring out the parameters that will produce a fiber for a given polymer-and-solvent system has been a trial-and-error process, says Wnek, because every recipe had its own set of instructions.
In the April 25, 2005 Polymer, Wnek and his team reported a series of calculations to determine the appropriate polymer concentration. “We want to have some predictive value,” he says.
Fiber fillers
Electrospinning’s amenability to additions is providing researchers new ways to consider delivering drugs and other compounds to cells and tissues. In the July 2005 Biomacromolecules, Rabolt, Kristi L. Kiick, and their colleagues reported making biocompatible polymer fibers that contain heparin, which has a structure similar to heparan sulfate, found in the body’s scaffolding for cells. In the body, heparan sulfate binds growth factors until the cells are ready to use them, says Kiick.
The researchers’ recipe included poly(lactide-co-glycolide) and an additional polymer, called poly(ethylene glycol), that was attached to heparin. Mats of the new fibers slowly released their heparin payload for about 2 weeks. The system is intended to replicate the body’s measured delivery of growth factors by heparan sulfate reservoirs, Rabolt says.
Rabolt and Kiick have now begun studying how cells respond to the mats, which the researchers say could eventually be used as patches that help the body repair skin or damaged internal organs.
Using a similar approach, Long and his colleagues have made fibers containing antibiotics. The team starts with a polymer, derived from lactic acid molecules, that is both biocompatible and biodegradable.
Electrospinning such molecules into nanoscale fibers “buys you surface area,” says Long, so that antibiotics can diffuse readily. There’s more surface area in a given volume of small fibers than in the same volume of larger fibers. A small electrospun patch can deliver a sizable antibiotic dose, says Long. His group is currently working on an electrospun-polymer patch that can be implanted in horses’ infected ankles, where it will release an antibiotic and then degrade.
In another application, Reneker and his University of Akron colleague Daniel J. Smith have patented an electrospun wound dressing. The bandage contains three layers of polymers that were spun separately. Each polymer binds one ingredient required for a reaction that produces the chemical nitric oxide, which helps wounds heal. The reagents react when water is applied to the bandage, and they don’t leave the bandage, which releases only the nitric oxide to the wound.
Spun supports
Electrospinning could have its biggest impact producing scaffolding for the emerging field of tissue engineering. The natural fibrous proteins, such as collagen, that make up the body’s scaffolding have diameters in the range of hundreds of nanometers to a few micrometers. Electrospun polymers offer materials that are “beginning to approach the scale that the cells would see in the natural extracellular matrix,” says William R. Wagner of the University of Pittsburgh.
Wagner, his University of Pittsburgh colleague Michael S. Sacks, and their respective research teams are designing biodegradable-fiber scaffolds for cardiac tissue. The scaffolds, seeded with cells and then implanted in the body, are being developed to provide support for heart cells until they produce their natural matrices.
Wagner’s team has worked out a method to align the fiber during spinning to create a network that has a more regular structure than the typical crisscrossed mat does. Instead of a metal plate, the researchers use a cylindrical target called a mandrel to make electrospun fibers arrange themselves into tubular mats. In this electrospinning setup, the researchers rotate the mandrel on its axis and move it back and forth under the syringe. When the mandrel’s back-and-forth motion reaches 2 meters per second, the fiber lines up along the length of the cylinder. The resulting mat is stiffer along its length than across its diameter.
Having control over the direction of stiffness is desirable for tissue engineering, says Wagner, because “you want to train the cells for the job they will have to do.” If a scaffold can behave as an artery does, the cells growing on it should produce a better replacement tissue than those on a static scaffold would, he says.
Sacks’ group has applied various stress tests to the scaffolds, loading and stretching them to study their mechanical behavior. Sacks and Wagner demonstrate in an upcoming Biomaterials that the resulting scaffold’s mechanical properties resemble those of heart-valve tissues, which vary widely in their elasticity in different directions.
In another innovation, Wagner’s team has devised a way to seed spun mats with cells. The researchers combine electrospinning with a technique called electrospraying, which uses a smaller voltage difference between the syringe’s needle and the plate. The drops containing cells fall to the plate intact instead of elongating into a fiber.
While one polymer-filled syringe propels a fiber to the target, a second syringe sprays vascular smooth muscle cells there. The researchers report in the February Biomaterials that the technique uniformly infused the mat with viable cells. The team is just beginning to test such a mat for tissue growth in rats.
Engineering vascular tissue is “a long-term research goal,” says Sacks, but he’s optimistic that electrospinning can move the technology along. “There’s really nothing else I know of that will match this approach.”
Spinning’s spread
While new uses abound, electrospinning isn’t likely to challenge current manufacturing methods for fabrics. “It’s hard to make a lot of stuff quickly,” says Wnek. “That’s been a criticism of electrospinning for a long time.”
But he doesn’t consider speed and volume critical issues in biomedical applications of the technique. “If you are thinking about coverings for wounds or a scaffold to grow a little piece of tissue, you don’t need much stuff,” Wnek says.
Electrospinning is changing the definition of what is spinnable, though. For example, Wnek and his colleagues have created fibers from natural polymers, such as collagen and fibrinogen, a protein that contributes to blood clot formation.
And in the Jan. 20 Science, Long’s group describes fibers made of a material that isn’t a polymer. The team used phospholipids that are components of cellular membranes (SN: 1/28/06, p. 61: Available to subscribers at Engineering membranes from cellular parts).
Phospholipids behave differently than polymers do. Because they contain a hydrophilic head attached to a hydrophobic tail, they organize into spheres when they’re in solution. In water, the hydrophilic heads face out, protecting the hydrophobic tails inside. In oily solvents, the heads stay in and the tails face out. Long’s group reasoned that if phospholipid molecules can self-organize in such a way, “then they should also form a fiber,” says Long, “and indeed, they did.”
Long’s team is now experimenting with ways to make electrospun phospholipids more durable. The electrostatic interactions that hold together the fiber break down in water. Mats made from such fibers might be fine for applications in which biodegradability is desirable, says Long. But for other uses, such as a blood filter made of natural materials, an insoluble mat would be necessary.
“Tunable durability,” Long says. “That’s the next step.”