Wireless patches can comfortably monitor sick babies’ health
New skin sensors are less invasive and don’t harm an infant’s fragile skin
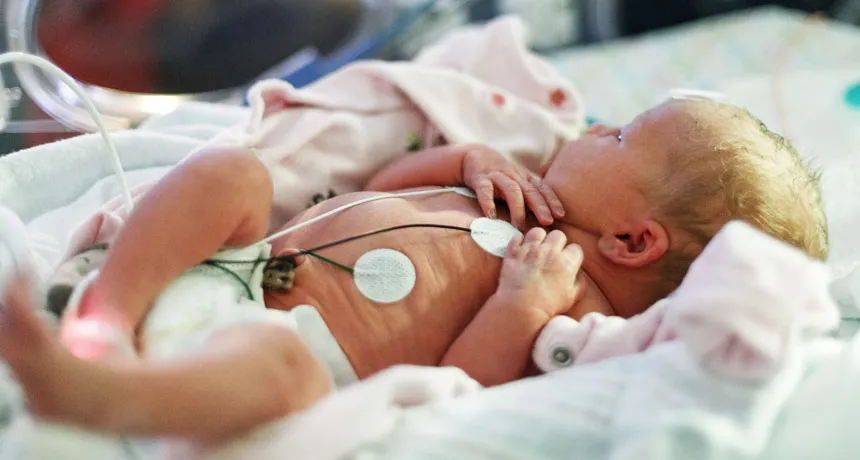
UNPLUGGED Ultrathin skin sensors that wirelessly stream vital-sign data to external devices could offer a less cumbersome way to monitor hospitalized infants than traditional, wire-tethered sensors (shown).
Susan Schmitz/Shutterstock
Wireless skin patches that measure a baby’s vital signs could offer a safer, more comfortable way of monitoring premature and sick infants in the hospital.
Each year, about 300,000 newborns are admitted to U.S. neonatal intensive care units, or NICUs, including preemies that are vulnerable to heart problems, breathing trouble and other medical complications (SN Online: 2/16/11). Doctors need to keep constant tabs on these tiny patients’ vital signs, and that typically involves outfitting a newborn with rigid sensors that are wired into machines around the baby’s cradle.
But adhesives on these sensors can harm an infant’s fragile skin, and they make it difficult for caregivers to hold the child, providing crucial skin-to-skin contact (SN Online: 3/22/17). The new wireless sensors, described in the March 1 Science, are designed to avoid those problems.
Each patch comprises an ultrathin layer of electronics sandwiched between sheets of flexible silicone. One patch, placed on an infant’s chest or back, uses electrodes to monitor the electrical activity of the baby’s heart (SN Online: 1/4/16). A second patch, worn on the hand or foot, shines LEDs on the baby’s appendage and measures how much illumination the tissue absorbs to measure the amount of oxygen in the blood. Both sensors monitor the baby’s temperature.

The supersoft silicone patches, which don’t need to be coated with adhesive to stick to skin, are easier on infants’ skin than traditional equipment, says study coauthor Steve Xu, a physician-engineer at Northwestern University Feinberg School of Medicine in Chicago.
Two soft, flexible surfaces, like the sensor patch and a baby’s skin, have a natural propensity to stick and stay together. “It’s like putting two pieces of American cheese together,” Xu explains. Without adhesives, these new sensors are much easier to peel off — which is especially important for preemies, who “are basically born as if they’re a giant wound, because their skin’s not developed enough,” he says.
This wireless setup could also make it easier for doctors and nurses to properly position children for medical examinations and procedures, and for parents to hold their kids, says Ruth Guinsburg, a neonatologist at the Federal University of São Paulo in Brazil whose commentary on the study appears in the same issue of Science. Besides facilitating parent-child bonding, skin-to-skin contact has been shown to reduce an infant’s risk of infection and help alleviate pain, she says.
Babies that are sick or born prematurely may not be the only patients to benefit from this technology, says study coauthor Amy Paller, a pediatric dermatology researcher also at Northwestern Feinberg School of Medicine. The skin patches could also provide a gentler means of monitoring patients with exceedingly fragile skin, such as burn victims or people with genetic skin disorders like epidermolysis bullosa (SN: 12/9/17, p. 6).