Cancer killers send signal of success
Nanoparticles deliver drug, then give real-time feedback when tumor cells die
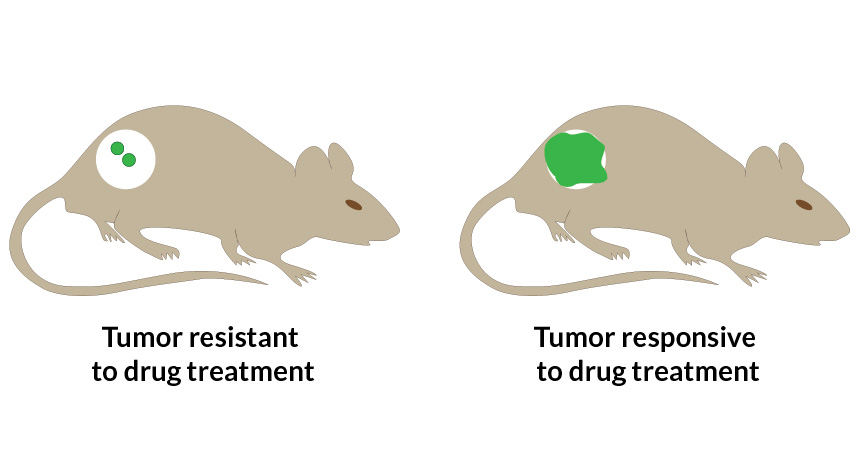
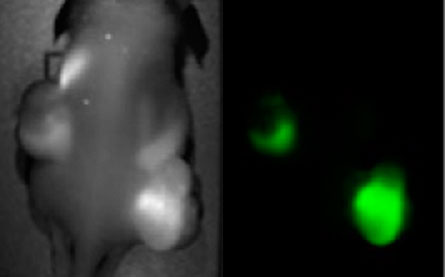
LIVE REPORT New lab-made nanoparticles deliver cancer drugs into tumors, then report their effects in real time by lighting up in response to proteins produced by dying cells. More light (right, green) indicates a tumor is responding to chemotherapy.
A. Kulkarni et al/PNAS 2016