Solving mysteries of reproduction helped make parenthood possible for millions
A variety of assisted reproductive technologies have become almost routine

Nature pulls off a small miracle each month: Just one egg matures in an ovary and bursts forth to reach the fallopian tubes, ready to be fertilized. Assisted reproduction now makes maturation and fertilization work in the lab as well.
Nicolle Rager Fuller
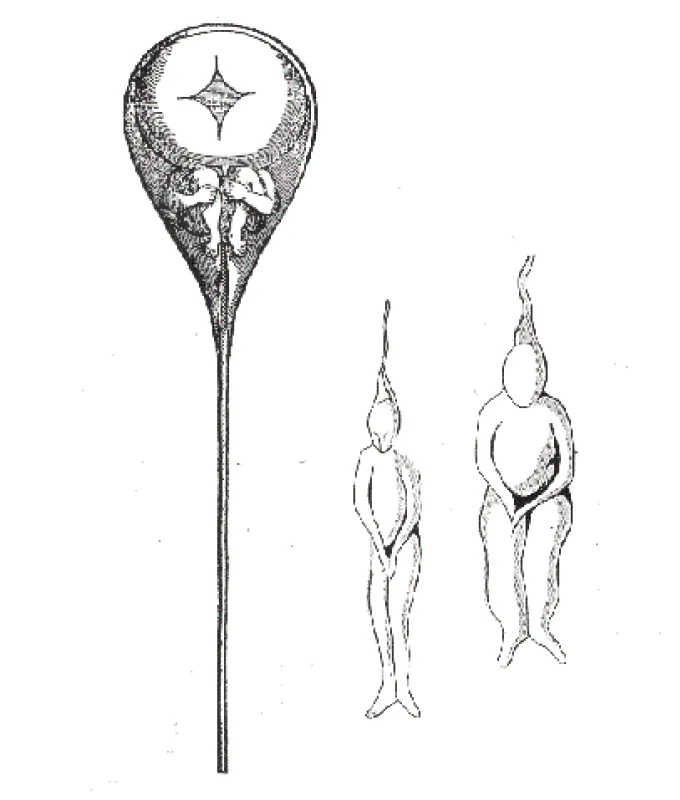
In the beginning, no one really understood how babies were made. Thinkers puzzled for millennia about how life arose from one generation to the next. But not until the 17th century did scientists start to seriously study the question. At that time, the theory of preformation held that minuscule humans already existed, fully formed, in either the mother’s menstrual blood or the father’s semen, depending on whether you were an “ovist” or a “spermist.”
Little changed until two late-19th century scientists, Oskar Hertwig from Germany and Hermann Fol from France, independently conducted experiments on sea urchins, proving conclusively that creating new offspring takes one egg and one sperm.
Despite the early confusion, the ancients were sure about one thing: Reproduction is far from a sure bet. Today, an estimated 15 percent of couples worldwide are unable to conceive a child naturally, leading to feelings of sorrow, loss and a profound sense of inadequacy for many. A century ago, science didn’t have much to offer these couples.
The only fertility intervention widely available in 1921 was artificial insemination by donor sperm, which was morally and legally fraught. In the first half of the 20th century, the practice was often considered a form of adultery; as recently as 1963, an Illinois court ruled that a baby conceived this way, even with the husband’s consent, was illegitimate.
In 1978, everything changed. The birth of Louise Brown, the world’s first “test tube baby,” proved that infertile couples had another option: in vitro fertilization. The technique involved removing a mature egg from the mother, mixing it in a lab dish with the father’s sperm, and letting the fertilized egg, called a zygote, grow for a couple of days. The zygote was then returned to the mother’s uterus, where it could implant and grow in an otherwise normal pregnancy.
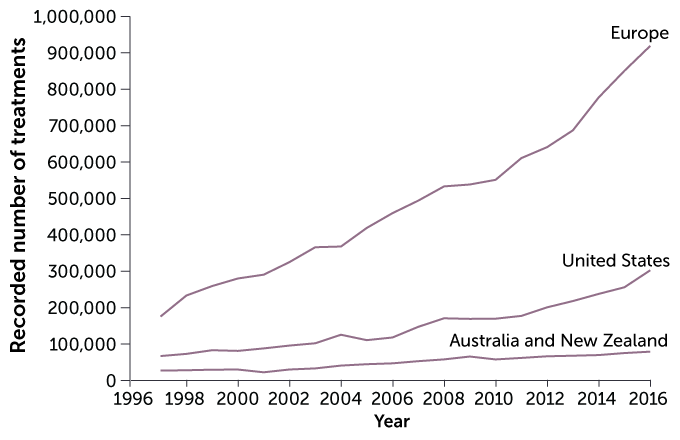
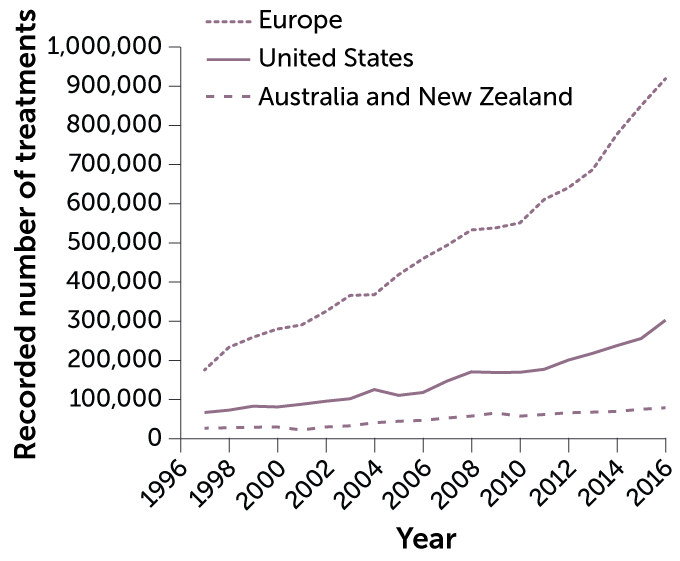
Since Brown’s historic birth, scientists have devised a range of ways to give Mother Nature a boost in baby-making. The various methods are known collectively as assisted reproductive technology, or ART. Some 9 million babies worldwide have been born using versions of ART.
The impact has been as profound sociologically as it has been medically. Now that ART has become almost routine, many of the early complaints about scientists playing God and manipulating life have faded away. Parenthood is now possible for people who never imagined it in their futures, including same-sex couples and single parents, thanks to such refinements as egg donors, surrogacy and the successful freezing of eggs, sperm and embryos. And all of it begins, as human life itself does, with the egg.
Good eggs
Even scientists can’t make babies without eggs. Normally, a woman produces only one mature egg every month, and the quality of her eggs tends to decline as she reaches her late 30s. So researchers’ ability to retrieve and prepare this scarce resource for fertilization, and if necessary preserve the eggs through freezing, have all been crucial in assisting reproduction.
Women have two ovaries, each one containing thousands of immature egg follicles. During the childbearing years, the ovaries usually release mature eggs in rotation: a single mature egg bursting from the right-hand ovary one menstrual cycle, from the left-hand ovary the next.
But women using ART often rely on injections of various fertility hormones to get the process going. These shots will enable sluggish ovaries to produce eggs that can be fertilized either through intercourse or in the lab via IVF. For IVF, the most robust-looking candidates are chosen to implant or to freeze for later use. This first step in ART, it turns out, is also one of the trickiest: choosing the right hormones to get the eggs you need.
Knowledge about hormones and how they affect ovulation dates back to 1923, when scientists Edgar Allen and Edward Doisy of Washington University School of Medicine in St. Louis first isolated estrogen in experimental mice and rats and found that it was produced in the ovaries. By the 1940s, scientists had elucidated the ebbs and flows of other hormones in lab animals and humans — follicle stimulating hormone, luteinizing hormone and human chorionic gonadotropin — over the course of a typical menstrual cycle.
ART usually begins with a woman giving herself daily injections containing a cocktail of these hormones, generally for 10 to 14 days. But for some women who want to have children but are dealing with a cancer diagnosis, hormone injections aren’t an option — and the clock is ticking. They need to start cancer treatments as soon as possible, but many of the treatments are likely to damage the reproductive system.
To preserve their fertility, these women might choose to freeze their eggs before cancer treatment. But they might not have 10 or so days to wait until the hormone injections provoke their ovaries to produce extra eggs — nor might they be able to take the drugs in the first place if they have a hormone-sensitive cancer, such as some breast cancers, that ovulation-stimulating drugs might make worse. So for these women, researchers had to find ways to bring a bunch of eggs to maturity all at once and outside the body — a technique known as in vitro maturation.
In vitro maturation was first used in 1934, when Harvard researchers Gregory Pincus and E.V. Enzmann used it in rabbits (SN: 3/10/34, p. 149). The two scientists cultured immature rabbit eggs for about a day, supplementing the nutrient broth either with extracts from cow pituitary glands or with an unspecified “maturity hormone.” Both supplements helped the immature eggs grow to maturity, at which point they were successfully fertilized.
In 1940, Pincus was asked by a New York Times reporter what the next big development might be in reproductive science. “There are no big steps, there are all little steps,” he said, declining to make any predictions. All he knew for sure, he said, was that the “big questions” of the day were: Why does an egg start to develop, and why does it continue to develop?

When reproductive endocrinologists retrieve eggs from their ART patients, after either stimulating the ovaries via hormone injections or maturing the eggs in the lab, they have two choices: fertilize the eggs and implant the embryo right away, or store them. For women who are not yet ready to have a baby, storing the eggs is the best option. This is done through freezing — which, in the early days of ART, was a tricky business indeed. Eggs have a high fluid content that leads them to form crystals when frozen; during thawing, those crystals can damage the egg, especially the delicate apparatus needed to cut the cell’s chromosome number in half. By dividing the chromosomes, one egg plus one sperm can fuse together without doubling the chromosome count.
In the 1980s, egg freezing worked occasionally; the first successful pregnancy using a woman’s own frozen eggs, leading to the birth of healthy twins, was reported in 1986 by Christopher Chen of Flinders University of South Australia in Adelaide. But egg freezing was still a long shot. Estimates were that no more than 1 or 2 percent of thawed eggs would result in a live birth.
Then, in 1999, reports appeared of a more reliable freezing method: vitrification, which freezes the egg so rapidly that no ice crystals can form. A research team based in Australia and Italy described animal experiments in which 1 in 4 vitrified cow eggs were fertilized and later grew, by around day 5, to the blastocyst stage. It was only about half the rate achieved for fresh cow eggs, but it was still several times better than the rate for slow-frozen eggs. When it came to clinical use, some researchers put the live birth rate of vitrified eggs at about 2 to 12 percent for women under age 38.
At first, vitrification was limited to people who froze their eggs for medical reasons such as cancer. But in 2013, egg cryopreservation became an option for anyone who wanted to delay childbearing for any reason, medical or not.
By 2020, estimates were that a growing subset of women who choose egg vitrification each year in the United States do so because they’re not ready to have children yet but hope to eventually — lifestyle-related reasons that have come to be known as “social freezing.”
While social freezing is often promoted as a way to delay childbearing almost indefinitely, it turns out that most women never return to the clinic to use their frozen eggs. At McGill University in Montreal, for instance, William Buckett and his colleagues found that over the course of 13 years, the school’s cancer fertility preservation program treated 353 women, of whom 9 percent died, 6 percent got pregnant spontaneously, and the majority were either still dealing with their cancer or had lost touch with the clinic for unknown reasons. Just 23 women, 6.5 percent of the group, came back to McGill to use their frozen eggs or embryos. That low return rate is also true for women who opt for social freezing.
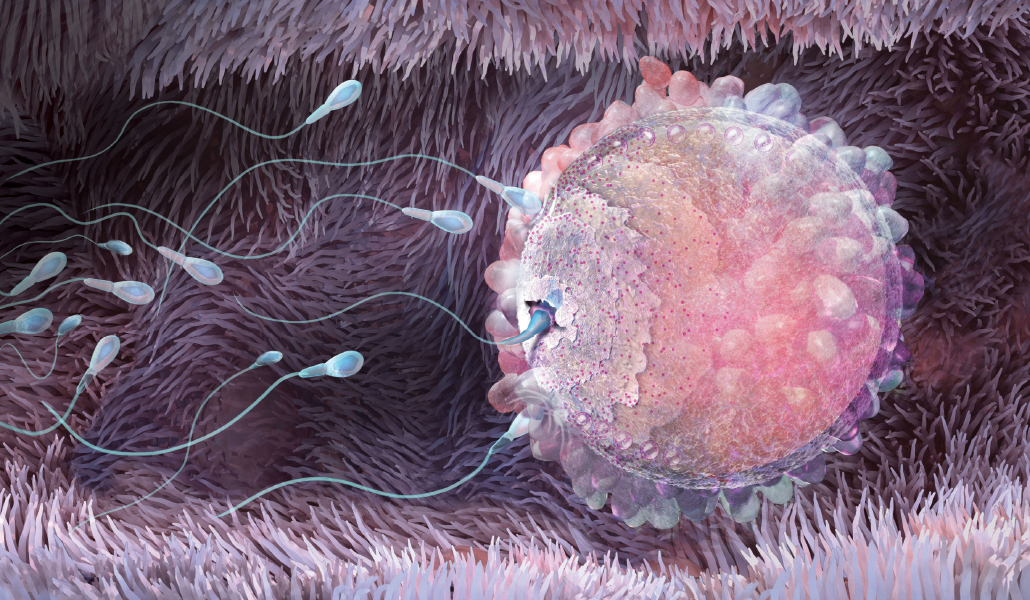
Sperm meets egg
Compared with the human egg, sperm are pretty simple. They were first observed in 1677 when Antonie van Leeuwenhoek, the Dutch inventor of one of the world’s first microscopes, took a look at his own ejaculate under magnification and noticed what he called “animalcules” swimming around in the sample. But their structure and function didn’t come into focus until 1876, when Hertwig watched a sperm fertilize the egg of a sea urchin.
Pincus and Enzmann, who were the first to bring mammalian eggs to maturity in the lab, used rabbit sperm to achieve the first laboratory fertilization in a mammal in 1934.
It took years of struggle to make the leap from rabbits to humans. In 1951, an oddity of sperm made it seem that Pincus and Enzmann had gotten lucky. Sperm cells, it appeared, needed to be primed in some way through a process called capacitation before they could pierce the egg.
Robert Edwards of Cambridge University, one of the world’s leading investigators in IVF through the 1960s and 1970s, thought capacitation would be “a terrible obstacle to IVF,” recalls Roger Gosden, an embryologist who worked in Edwards’ lab and authored Edwards’ biography, Let There Be Life. He remembers some frantic attempts to mimic sperm capacitation — such as when scientists created porous chambers, roughly the size of an implanted IUD, or intrauterine device, used for contraception. The researchers would fill a chamber with sperm and insert it into the uterus of a volunteer, hoping to expose the sperm to whatever unknown capacitating substance exists in nature. After waiting a bit, the scientists would pull on a string attached to the chamber to retrieve the now “primed” sperm to see if they had indeed become better able to fertilize eggs in the lab.
In the end, scientists found an easier way. “You just have to wash the sperm to get rid of some surface constituents,” Gosden says, and the sperm are ready to fertilize an egg in a lab dish. Other difficulties in clinical research proved more formidable, such as gauging the best timing of egg retrieval from women, and tweaking how many days post-fertilization were best to transfer the zygote to the uterus. Edwards and his collaborators, including gynecologist Patrick Steptoe, had more than 300 failed attempts at in vitro fertilization before their first success with Louise Brown in 1978 in England (SN: 7/25/18). Edwards went on to win the Nobel Prize in 2010 for his IVF discoveries.
Among the beneficiaries of Edwards’ pathbreaking work is Claudy, who was diagnosed with breast cancer at age 29, and who in a different century might never have been able to have a baby of her own. Claudy sought out Michaël Grynberg and his colleagues at the Antoine Béclère University Hospital fertility clinic, just outside Paris, to discuss ways to preserve her fertility. It was 2014, and egg freezing through vitrification was becoming more common. But bringing an immature egg to maturity in the lab was still relatively rare. From the time of the first baby born from fresh lab-matured eggs in 1991 to the time of Claudy’s arrival at Grynberg’s clinic, only about 5,000 such births had occurred.
But Grynberg had no choice. He had to retrieve immature eggs from Claudy, for the sake of both speed and to avoid aggravating her hormone-sensitive breast cancer with fertility drugs. In addition, he would have to do something unprecedented in the context of cancer: Freeze those lab-matured eggs for later use. No baby had ever been born from eggs taken from a cancer patient that were matured in the lab and then frozen. (There had been one baby born at McGill in 2009 from a woman who did not have cancer, whose eggs were matured in the lab and frozen, then thawed.)
Grynberg extracted seven immature eggs and was able to grow six of them to maturity over the next 48 hours. Those six went into the deep freeze, while Claudy had surgery and chemotherapy.
A few years later, Claudy’s oncologist told her it was safe to get pregnant, and she spent a year trying to conceive. But she didn’t. So in 2018, she returned to Grynberg’s clinic, where the doctors prepared to thaw her six frozen eggs.
To fertilize them, in Claudy’s case, required an additional bit of ART. Because her eggs had been frozen, her partner’s sperm would need help to fertilize her eggs. Vitrification causes changes in the egg’s outer membrane that makes the thawed egg particularly hard for sperm cells to penetrate. This membrane, called the zona pellucida, is a formidable barrier even in nature (SN: 1/3/09, p. 15). One of the first to describe it was Sardul Singh Guraya, a biologist at Punjab Agricultural University in India, who did his early work in field rats.
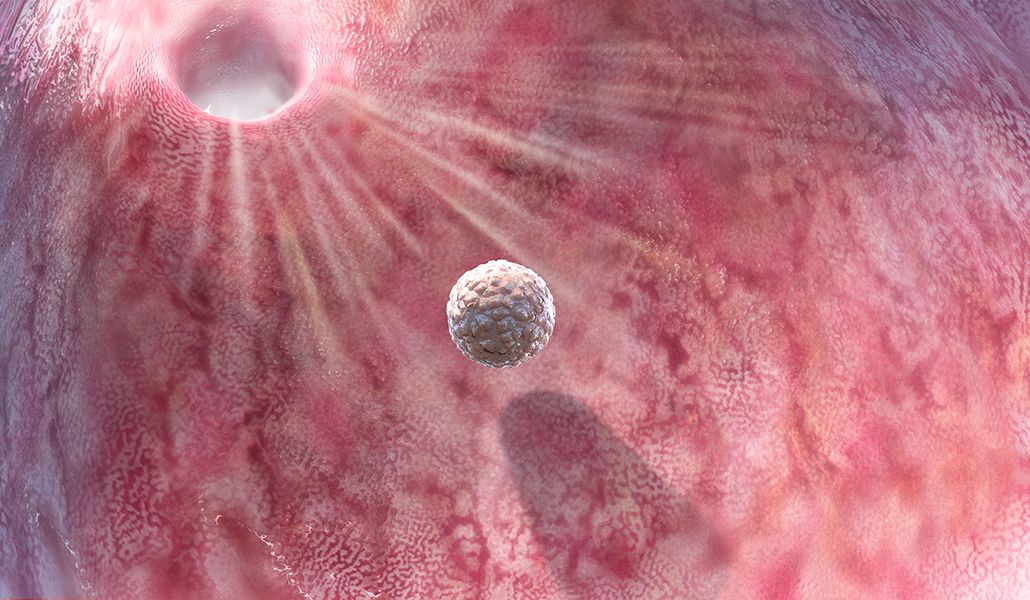
The zona pellucida, Guraya reported in 1978, is a barrier around the egg made of proteins and carbohydrates, and when one sperm breaches it, cortical granules rearrange themselves to shut out all other sperm. This ensures that the zygote will have a normal genetic complement of just two pairs of 23 chromosomes, one from the mother and one from the father, rather than a grossly inflated number that would result if multiple sperm fertilized the egg.
Scientists spent much of the next decade trying to get sperm into eggs that had been frozen using micro-manipulations described with such invasive terms as “zona drilling.” But the sperm still failed to reach the nucleus for fertilization.
Then in 1992, Gianpiero Palermo, an Italian scientist on sabbatical from the University of Bari, reported on an accidental discovery he made while working in a fertility lab at the Free University of Brussels. When he tried to gently inject sperm beneath the outer layer of the egg, careful not to pierce the jellylike center known as the cytoplasm, he noticed that an occasional “dimple” in the membrane would allow the sperm to penetrate directly into the center anyway. When that happened, the egg was almost always fertilized. So despite the general recommendation to avoid doing so, Palermo tried injecting the sperm, tail and all, directly into the cytoplasm.
Of the first 47 attempts Palermo and his colleagues in Brussels made with this approach, 38 eggs remained intact after the injection, 31 were fertilized and 15 grew to embryos that could be transferred to a uterus.
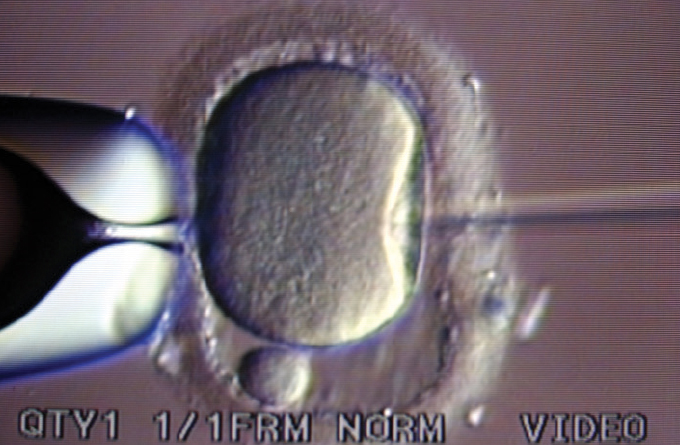
Ultimately, four babies were born: two healthy boys from two singleton pregnancies, and a healthy pair of boy-and-girl twins. The Belgian scientists called the procedure ICSI (pronounced ICK-see), shorthand for intracytoplasmic sperm injection.
Today, injecting a single sperm directly into an egg is even more common than the traditional form of IVF that adds sperm to an egg in a lab dish to let fertilization happen on its own. The injection method is used in about two-thirds of ART cycles around the world. And it is used in virtually all cycles that, like Claudy’s, start out with a hard-shelled frozen egg.
Growing a healthy baby
In 2018, Claudy returns to the fertility clinic at the Antoine Béclère University Hospital in suburban Paris. She is 34 years old and cancer-free. Because of the unusual nature of her case — her eggs were immature when they were retrieved and were brought to maturity in the laboratory — her doctors are not confident the eggs will survive the thawing and subsequent manipulations.
All six of Claudy’s eggs defrost with no apparent damage. The scientists perform ICSI on the eggs, using fresh sperm from Claudy’s partner. Five of the eggs fertilize.
These five zygotes go into an incubator so they can develop to a stage that is ready to implant. They undergo the early stages of cleavage, in which one cell becomes two, two become four, four become eight, and so on.
At many fertility clinics elsewhere in the world, doctors might interrupt things at this point to snip off a cell or two from the early embryo to see if things are progressing normally. It was revolutionary to discover that this could even be done — a feat first accomplished in 1968 by embryologist Richard Gardner. At the time, Gardner was a graduate student working in Edwards’ lab in Cambridge. His work showed for the first time that it was possible in rabbits to take cells from a blastocyst without causing harm (SN: 8/3/68, p. 119).
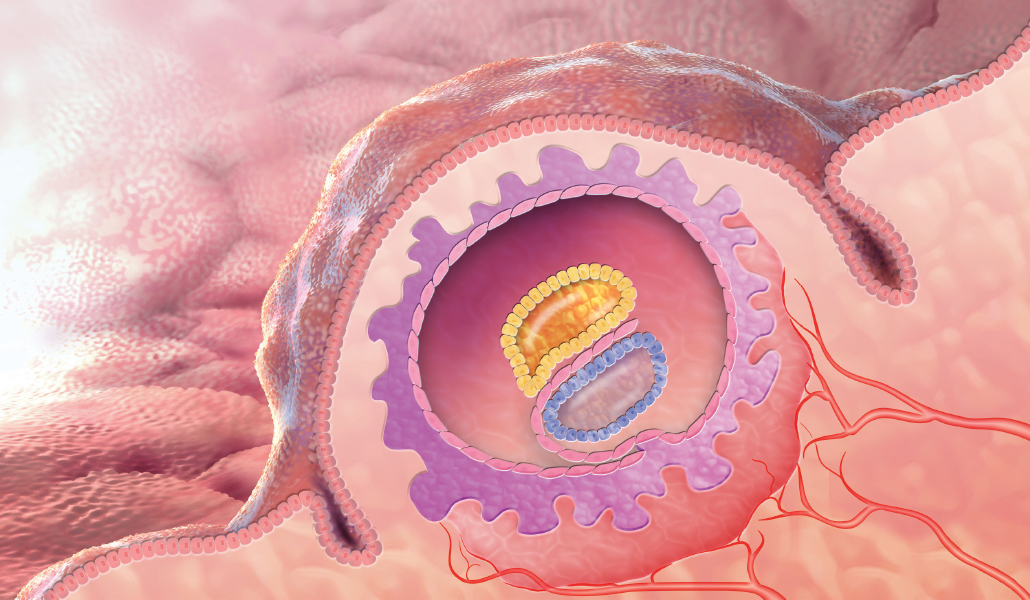
Scientists can examine the chromosomes of those cells removed from a human embryo, a process called preimplantation genetic diagnosis, or PGD. They might be looking for a particular disease-linked gene that runs in the family, to avoid implanting an affected embryo in the uterus. Or they might be checking that a developing embryo has the right number of chromosomes, and that the embryo has a good chance of implanting in the uterus and coming out a baby with 10 fingers, 10 toes and the chance of a healthy life.
In the future, they might also use PGD to see whether a desired gene tweak, introduced via a gene-editing technique like CRISPR, has actually taken hold. Without PGD, none of these approaches, from disease prevention to designer babies, could take place.
Two days after putting Claudy’s five embryos in the incubator, only one is still undergoing cleavage. That is the embryo the doctors transfer to Claudy’s uterus in the autumn of 2018.
The embryo implants, and continues to develop the way any embryo would, no matter what its origin story — a ball of a few hundred genetically identical embryonic cells that eventually differentiate into the 200 or so cell types that make up a human being. The mechanism by which this occurs was first laid out in 1924 by the German investigator Hans Spemann, who discovered the “organizer effect” that leads particular regions of the embryo to develop into particular cell types.
In 1965, Beatrice Mintz created mice that wore their bizarre genetic lineage on their unique, black-and-white striped coats. In her lab at the Institute for Cancer Research in Philadelphia, she created a mouse with four parents — two mothers and two fathers — to demonstrate which parent’s genetic contribution ended up in which region of the body (SN: 4/12/69, p. 361).

Mintz merged eight-celled embryos from two different mice, one pure black embryo and one pure white, by putting them into a lab dish, dissolving the protective layer around each embryo, and actually smooshing them together using a glass rod. The result was a mosaic mouse: Some of its cells contained genes that could be traced directly to the two white mouse parents, and some had genes from the two black mouse parents.
Other mysteries of how embryos develop were revealed by “knockout” technology, in which scientists disabled genes in a particular region of an embryo to see what those genes controlled. In 1995, developmental biologists William Shawlot and Richard Behringer of the University of Texas MD Anderson Cancer Center in Houston reported using this method in mouse embryos, confirming Spemann’s theory that a tiny region of the embryo touches off changes in neighboring cells to turn them into particular cell types (SN: 4/1/95, p. 197).
The embryo in Claudy’s uterus develops normally; everything about her pregnancy seems ordinary — except how miraculous it might feel to Claudy herself, who must have had some doubt, as a young breast cancer patient, about whether she’d ever have a baby of her own. In early July 2019, Claudy goes back to the Antoine Béclère University Hospital, this time to give birth. Her son is born on July 6; she and her partner name him Jules.
When Grynberg asks Claudy’s permission to write up her landmark case in the Annals of Oncology, she is overwhelmed. “I thought about everything I had gone through,” she told a reporter for the British newspaper the Telegraph as she posed for a photo with baby Jules. “And I cried as I realized how lucky I was.”