Skeletal Discovery: Bone cells affect metabolism
If your blood glucose is out of whack, the problem may be in your bones. New research in mice shows that bone cells exert a surprising influence on how the body regulates sugar, energy, and fat.
The discovery could lead to new ways to treat type 2 diabetes, a disease involving poor regulation of blood glucose. It also means that skeletons act as endocrine organs, which affect other body tissues by releasing hormones into the bloodstream.
“I’m already changing my teaching slides” about the functions of bones, comments Jennifer Westendorf, an associate professor of orthopedic surgery at the Mayo Clinic in Rochester, Minn. “Now we can add that [the skeleton] affects energy metabolism as well,” she says. “It’s certainly an exciting breakthrough.”
The team announcing the finding, led by Gerard Karsenty of Columbia University, had previously found that fat cells secrete a hormone that influences bone-forming cells called osteoblasts. Because hormone regulation between two cell types is often reciprocal, Karsenty and his team reasoned that osteoblasts might also be emitting hormones that control fat tissue. Osteoblasts make bone throughout a healthy person’s lifetime, while cells called osteoclasts tear down bone—processes that constantly remodel the skeleton.
Osteocalcin, a somewhat enigmatic protein produced only by osteoblasts, seemed like a good hormone candidate, Karsenty says. “[It] has been the flagship molecule of the [bone-research] field for 30 years, but nobody knew what it was doing.”
Karsenty’s team fed a normal diet to mice engineered to lack the gene for osteocalcin. The mice became obese and had low blood concentrations of insulin, a key hormone for controlling blood glucose. The animals also had poor sensitivity to insulin, a hallmark of people with diabetes.
Another group of mice, which had been engineered to have extra osteocalcin, stayed thin despite being fed a high-calorie diet. These animals also maintained higher insulin concentrations and better sensitivity to insulin than the mice lacking osteocalcin did, the team reports in the Aug. 10 Cell.
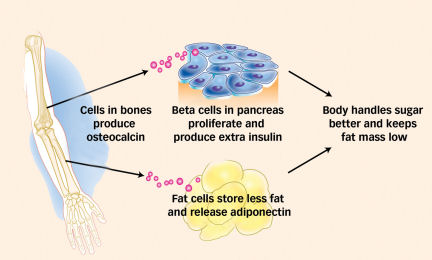
Further tests on mice showed that osteocalcin causes the insulin-making cells in the pancreas to proliferate and ramp up insulin production. The bone protein also causes fat cells to store less fat and to secrete a hormone called adiponectin. In people as well as in mice, this substance improves cells’ sensitivity to insulin.
Previous research has shown that many people with type 2 diabetes have low blood concentrations of osteocalcin.
“Osteocalcin, if everything goes well, could be a treatment for type 2 diabetes. That’s where the excitement is,” Karsenty says. Columbia University holds a patent on the idea, and Karsenty says that he’s helping form a company to commercialize the treatment.
“This could also have important ramifications for cardiovascular disease because of the effect on metabolic syndrome,” a condition related to diabetes, comments Dana T. Graves of Boston University. “The fact that bone cells regulate energy metabolism, and that they do it through osteocalcin, is a major finding,” he says.







