COVID-19 precautions may be reducing cases of flu and other respiratory infections
Once restrictions are lifted, there could be a deadly rebound in respiratory infections
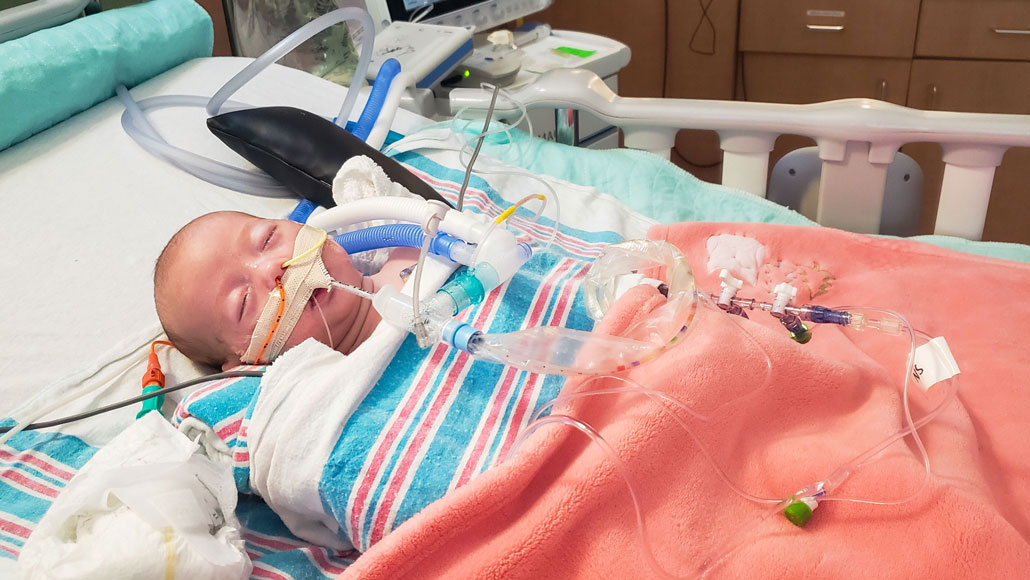
Mackenzie Burroughs caught respiratory syncytial virus (RSV) in December of 2019 and ended up in the hospital for more than a month. COVID-19 precautions are decreasing the incidence of these deadly respiratory infections this season.
Carla Burroughs
Heading into the dead of winter, doctors and scientists have noticed something odd: Missing cases of non-COVID-19 respiratory illnesses, specifically flu and respiratory syncytial virus, or RSV.
“We’re seeing very low numbers of both of these infections, even now, while we’re in the peak season,” says Rachel Baker, an epidemiologist at Princeton University. “We really should be seeing cases go up.”
Instead, positive flu tests reported in December are a little less than one one-hundredth of all of those tallied in December 2019, according to data from the U.S. Centers for Disease Control and Prevention. RSV’s drop in reported cases — to one two-hundredth of those a year earlier — is even bigger.
This dramatic dip is probably due to COVID-19 precautions. The same handwashing and social distancing that can prevent the spread of SARS-CoV-2, the virus that causes COVID-19, can prevent the spread of other viruses and pathogens. But that could mean trouble ahead. A lack of cases ironically leads to a growing population susceptible to infection, so future outbreaks could be larger and more unpredictable.
In a typical year in the United States, RSV hospitalizes an estimated 58,000 children under age 5 and more than 177,000 older adults. “Most people recover in a week or two,” says Benjamin Silk, an epidemiologist at the CDC. “But RSV infections can be serious, especially for infants, older adults and people with certain chronic medical conditions.” Worldwide, 3.4 million children under 5 years old are hospitalized with RSV each year, accounting for about 5 percent of deaths in this age group.
Highly contagious, RSV is transmitted through respiratory droplets, which can remain infectious for more than six hours on hard surfaces. Prevention is rooted in strict hand hygiene — using hand sanitizer or washing with soap and water.
In the United States, RSV season usually starts in the fall, peaking between December and mid-February. This year, there essentially is no peak. In December 2020, the CDC’s National Respiratory and Enteric Virus Surveillance System — which collects voluntarily reported data —reported just 120 RSV cases, compared with 24,280 in December 2019.
“RSV, in particular, is so stable — it does the same thing year after year,” Baker says. “I don’t think there’s much else that could explain [the drop] apart from the COVID-19 phenomena as a whole, particularly the control measures.”
Influenza infections are also down drastically. Flu regularly infects between 3 percent and 11 percent of the U.S. population and is especially deadly for older or immunocompromised people. The CDC estimates that in an average year, flu kills around 36,000 people and hospitalizes almost half a million.
According to the CDC’s lead flu tracker Lynnette Brammer, the adoption of COVID-19 prevention measures in the spring of 2020 coincided with a drop in the percent of positive flu tests from more than 20 percent to less than 1 percent — and that number has stayed low through the fall and now into winter (SN: 9/18/20). In December 2019, the CDC’s clinical lab FluVue reported 50,526 positive flu tests. In December 2020, that number was just 454. Preliminary data suggest this trend is continuing into January, when flu season typically peaks.
Brammer says the numbers of flu tests are steady, so it’s not that people aren’t going to get tested. They just aren’t spreading it around as much.
Dropping diseases
Positive tests for influenza and RSV have dropped drastically since COVID-19 prevention measures were put into place in March 2020.
Positive U.S. flu and RSV tests, October 2019–January 2021
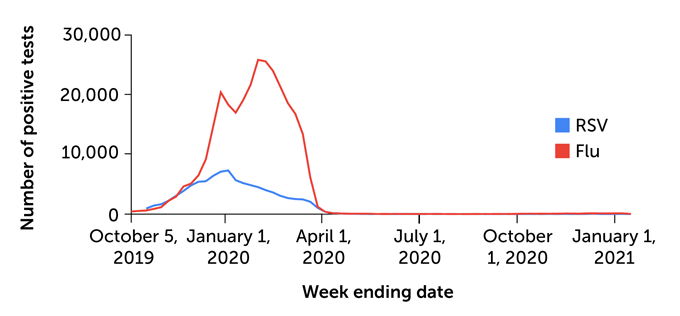
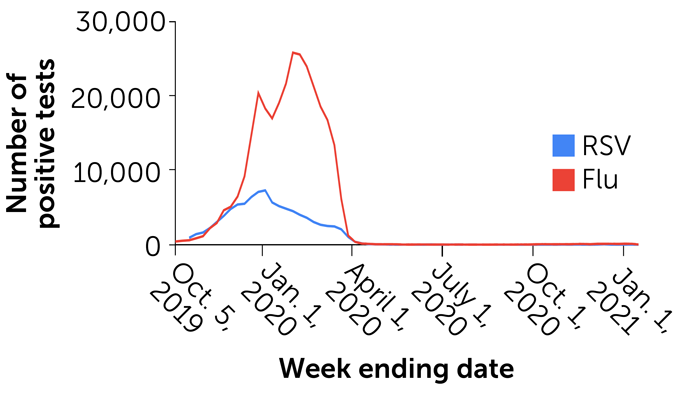
Some other infections, like parainfluenza, also seem to have declined with COVID-19 prevention measures, but viruses like rhinoviruses continue near their normal season levels. It could be because these viruses, unlike flu and RSV, aren’t as thoroughly destroyed by handwashing and using sanitizers.
This great news comes with a warning, though. Fewer infections means fewer people being exposed and gaining immunity to these viruses, building up a population susceptible to these infections later. That could fuel a deadly rebound in infections post COVID-19, Baker, the Princeton epidemiologist, and her colleagues reported December 1 in Proceedings of the National Academy of Sciences. In the analysis, the team assumed COVID-19 precautions would reduce RSV and influenza infections by 20 percent, but the decrease is proving to be much larger.
“We need to be prepared for offseason outbreaks and potentially large outbreaks,” Baker says.
That’s what’s happening right now in Australia’s New South Wales. Clinical nurse Gemma Saravanos and her colleagues observed a more than 85 percent reduction of positive RSV tests during the peak of their season, between April and June, the team reported in the Lancet in September. But now, after beating back COVID-19 and lifting stringent protective measures, they have a record-breaking offseason RSV outbreak on their hands. In the last two weeks of December 2020, NSW reported more than 6,000 positive RSV tests — during a time they typically have a few hundred. In 2019, the RSV season peaked at around 4,695 detections in May.
“It’s really extraordinarily unusual,” says Saravanos, who works at the University of Sydney. “It’s never been seen before.”
A rebound outbreak might hit the United States, too, Baker says. Australia “could be an interesting foreshadowing of what is to come in the Northern Hemisphere.”
That worries Carla Burroughs, a mother of four and former medic in Mobile, Ala., who has experienced RSV first hand. “The first time I heard of RSV, I was working on an ambulance, and I [transported] a child who passed away [from it],” she says. Then in December 2019, Burroughs’ 3-year-old daughter, Kaylee, caught RSV and was hospitalized for three days. “The second the doctor told us RSV with Kaylee, it just brought flashbacks. It just sent me into such a panic mode; I immediately knew this is going to be bad.”
It did get bad. A week later, Burroughs’ infant twins caught RSV. One, Mackenzie, was intubated for two weeks and stayed in the hospital for over a month. Seeing her daughter struggling to breathe, Boroughs says, “just changed everything. It took more of a toll on me than I expected.”
Burroughs’ children recovered, and she says now the new data show just how important basic hygiene behaviors are to helping prevent the spread of these viruses, saving thousands of lives every RSV and flu season — even without a pandemic. “It’s sad that [the pandemic] is what it came down to,” Burroughs says. “We should have already been doing all these things.”
Sign up for our newsletter
We summarize the week's scientific breakthroughs every Thursday.







