Lowering blood pressure may help the brain
In preliminary SPRINT results, fewer people aiming for 120 developed early memory loss
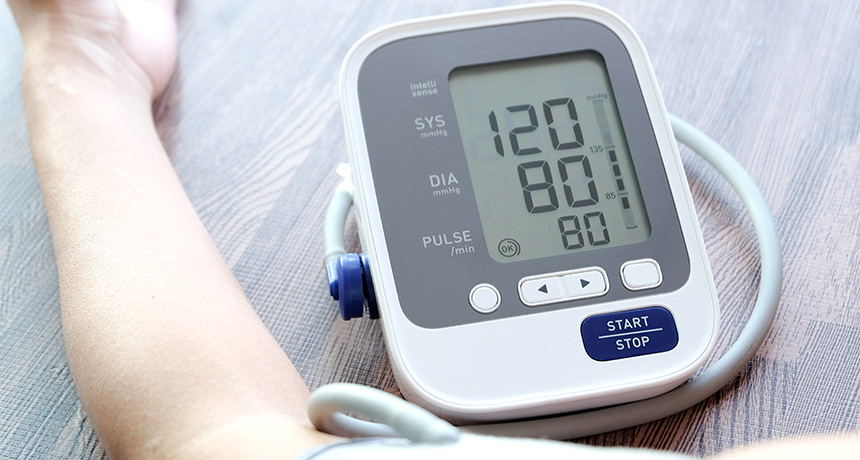
UNDER PRESSURE Dropping blood pressure below 120 millimeters of mercury reduces the risk of developing early memory loss, early results of a major clinical trial suggest.
Seasontime/Shutterstock
Keeping a tight lid on blood pressure isn’t just good for the heart. It may also help the brain.
People given intensive drug treatment for high blood pressure were less likely to develop an early form of memory loss, according to preliminary results from a major clinical trial. This approach reduced the rate of early memory loss, called mild cognitive impairment, by around 19 percent, compared with people who received less aggressive treatment.
And the intensely treated group developed fewer white matter lesions over time, researchers reported July 25 at the Alzheimer’s Association International Conference in Chicago. White matter lesions, which are associated with dementia, are thought to be caused by blood vessel injuries in white matter, the part of the brain that contains nerve fibers.
The brain research is part of SPRINT, the Systolic Blood Pressure Intervention Trial involving more than 9,300 participants. Some received intensive treatment aimed at lowering their systolic blood pressure — the pressure on artery walls when the heart beats — below 120 millimeters of mercury; others got standard treatment to bring it below 140.
The trial had already reported that participants who received the intensive treatment dropped their risk of heart attacks and other cardiovascular problems by 25 percent, compared with the standard group (SN Online: 11/9/2015). The results were the basis for revamped blood pressure guidelines, released last year (SN: 12/9/17, p. 13).
Dubbed SPRINT-MIND, the brain research set out to measure whether aggressively controlling blood pressure benefits the brain along with the heart. Observational studies have shown that people with lower blood pressure have a lower risk of developing dementia, says Jeff Williamson, a geriatrician at Wake Forest School of Medicine in Winston-Salem, N.C.
Using memory tests, experts assessed the trial participants for probable dementia (people unable to perform daily activities independently), early memory loss (people with some difficulty functioning, but still independent) or no impairment. More than 8,600 of the participants completed an assessment up until June 2018; their average age was about 68 years old.
Fewer people in the intensely treated group had the early memory loss, which is often a precursor to dementia, Williamson says. And fewer had probable dementia as well, although the results were not statistically significant. The trial was ended early, in 2015, due to the compelling cardiovascular benefits, so participants’ blood pressure was medically managed for only two to three years. “That’s an encouraging message,” Williamson says. “It doesn’t take but just a few years to see this effect.”
The SPRINT-MIND trial also looked at white matter lesions. These injuries in the brain are a consequence of aging, but they are also associated with hypertension, says neuroradiologist Ilya Nasrallah of the University of Pennsylvania. Previous work has found that white matter lesions increase the risk of dementia in people ages 60 and older.
About 450 participants had MRI brain scans at the start of the trial and roughly four years later. The volume of white matter lesions increased by 0.28 cubic centimeters over that time in the intensive treatment group, compared with 0.92 cubic centimeters in the standard treatment group. With intense blood pressure treatment, Nasrallah says, “we could slow progression of white matter lesions.”
But there is evidence that the relationship between blood pressure and brain health may change with advancing age, notes cognitive neurologist Zoe Arvanitakis of Rush University Medical Center in Chicago, who was not involved with the trial.
In adults 75 and older, past work has found that low diastolic blood pressure — the pressure on arteries when the heart rests between beats — increases the risk of dementia. The age at which people are at high risk for dementia is older than the average age of those in SPRINT, Arvanitakis says. “We really need to study this question in older persons as well.”
Neurologist and neuroscientist Costantino Iadecola of Weill Cornell Medicine in New York City says that, in general, the study shows that lowering blood pressure closer to 120 has beneficial effects on the brain. The problem is that in midlife, when people are 40 to 60 years old, “there is no question that high blood pressure is bad for you,” but that’s not true for those 80 and above, he says. Older people may need higher blood pressure to get enough blood flow to the brain.
Still, the study “is a piece of good news in an otherwise grim landscape” regarding dementia, Iadecola says, because it suggests “you can make the brain better if you take care of your blood pressure.”