
About 3.6 million children were hospitalized and more than 100,000 died from RSV in 2019. Vaccines and preventive antibody injections in clinical trials may soon ease the burden of infection on kids and older adults too.
Jill Lehmann Photography/Getty Images
Editor’s note: On September 22, 2023, a U.S. Center for Disease Control advisory board recommended that an RSV vaccine, made by Pfizer, be given between the 32nd and 36th week of pregnancy. Pregnant people would get the vaccine before and during RSV season from September to January to protect babies born from October through April. The committee wrangled over how to use the vaccine instead of or in combination with a lab-made monoclonal antibody approved by the FDA in July. In most cases, the vaccine and antibody would not be used in the same infant. The antibody would be given to babies 8 months old and younger who are born to unvaccinated people or to infants born April through October.
Finally, researchers may have ways to combat a deadly respiratory illness.
The disease is not the flu or COVID-19, but respiratory syncytial virus, or RSV.
The virus was first identified in 1957 in Baltimore, but it has probably been around for millennia, says Jim Boonyaratanakornkit, a virologist and transplant immunologist at the Fred Hutchinson Cancer Center in Seattle. “It’s always been a plague for the very young and the very old,” he says.
In Europe, people age 60 and older may soon get some protection against the virus. An advisory committee recommended April 26 that a vaccine against RSV made by the pharmaceutical giant GSK should be approved for use. That decision will go to the European Commission for final approval.
No RSV vaccine has been approved in the United States. And there are no specific antiviral medications to combat RSV, and only one preventive treatment — a monoclonal antibody — is reserved for a small number of babies at high risk of severe disease. But that could soon change. Several companies now have clinical trial data suggesting that their various vaccine candidates or lab-made monoclonal antibodies can protect against RSV’s worst consequences.
Those treatments are geared, in part, toward the youngest children. People of all ages can contract the virus, but it tends to hit the youngest the hardest. In 2019, RSV caused an estimated 33 million infections worldwide in children ages 5 and younger. About 3.6 million children were hospitalized and more than 100,000 died, researchers reported last year in the Lancet. Their calculations revealed that RSV causes 1 in every 28 deaths of children 28-days- to 6-months-old.
“This is why we should care,” Penny Heaton of Janssen Pharmaceuticals, a company owned by Johnson & Johnson, said April 4 at the World Vaccine Congress, held in Washington D.C. Vaccines and antibodies might be able to prevent some of those deaths. “This is the amazing impact that … RSV vaccines [and] monoclonal antibodies … can have on the health of children globally.”
But it’s not just the 5-and-under crowd who will benefit. Their grandparents, great-grandparents and other older adults could soon get RSV shots. That could mean an easing of the burden of RSV in the two groups hit hardest by the virus.
Two companies — GSK, formerly GlaxoSmithKline, and Pfizer — are close to getting approval from the U.S. Food and Drug Administration for their RSV vaccines. Moderna isn’t far behind with an mRNA-based RSV vaccine. Meanwhile, Danish company Bavarian Nordic expects results from a clinical trial soon for its vaccine, and several other companies also have RSV vaccines in the works.
Other companies are developing monoclonal antibodies to give to babies and infants as preventives against RSV. Those lab-made antibodies aren’t vaccines, but a dose given before the start of RSV season may temporarily protect vulnerable babies from becoming very sick if they get infected.
There are so many options on the horizon that Janssen decided to bow out. “As we looked across our portfolio, and we looked across the RSV landscape,” Heaton said, “we have made the decision to discontinue our RSV program,” and to stop a late-stage clinical trial. The company also announced the decision in March, saying it wanted to focus on unmet medical needs. RSV, it seems, may soon no longer fit that bill.
For now, the virus is still very much a problem. Usually, RSV season starts in October and peaks in December or January — at least in the United States. It generally ends in April.
The virus almost vanished in the winter of 2020–21. In that first year of the COVID-19 pandemic, RSV-positive PCR tests never rose above 3 percent — the U.S. Centers for Disease Control and Prevention’s threshold for an epidemic. Before the COVID-19 pandemic, RSV positivity rates peaked each season at about 13 to 16 percent. RSV’s disappearance was thanks mostly to precautions, including social distancing and mask-wearing, put in place against COVID-19.
But the virus rebounded, appearing in the summer of 2021, researchers report April 7 in Morbidity and Mortality Weekly Report. That year RSV season shifted, starting in May. It hit its zenith in July and ended in January 2022.
The 2022–23 RSV season shifted closer to the prepandemic pattern but was still early. The 2022 season started in June and peaked in November with a positivity rate of 19 percent. The season ended sometime between December and February, depending on which part of the country you live in. This latest RSV season hit kids hard, overwhelming children’s hospitals in some places.
No one knows when the next RSV season will begin. But some of the vaccines and treatments in development could be ready for deployment this fall, potentially reducing the number of doctor visits, hospitalizations and deaths from the infections.
Here’s a breakdown of the vaccine and treatment candidates.
What is in the vaccines?
Three companies — Pfizer, GSK and Moderna — have based their vaccines on one of RSV’s proteins. That protein, called the F protein, sits on the virus’s outer membrane and helps it fuse to human cells. The F protein is a shapeshifter. Before fusion, it looks like a rounded knob. After fusion, it resembles a needle or pointy tower.
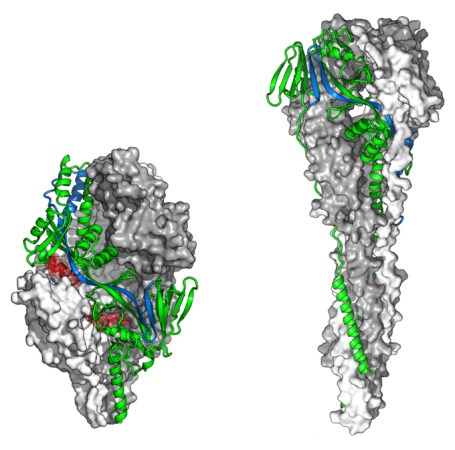
A decade ago, researchers at the U.S. National Institutes of Health figured out that locking the protein into its prefusion knob state causes the immune system to react more strongly than to the virus’ shapeshifting form. All three companies use some version of the F protein locked in the prefusion state in their vaccines. Pfizer described the nitty-gritty details of making this stabilized F protein April 6 in Science Translational Medicine.
Pfizer and GSK’s vaccines contain the protein itself. Moderna’s candidate, like its COVID-19 vaccine, is an mRNA vaccine that tells the body to produce the protein.
Bavarian Nordic is taking a different approach. The company makes a vaccine that works against both smallpox and mpox, formerly called monkeypox (SN: 12/12/22). That vaccine is live vaccinia virus, a pox virus that has been engineered so that it can’t replicate well in the body. Many vaccines, including those against flu, measles and chicken pox are also such live attenuated, or weakened, viruses.
For its RSV vaccine, Bavarian Nordic engineered the vaccinia virus to make five of RSV’s proteins, including the F protein. At the World Vaccine Congress, one person asked whether such a hybrid virus might give protection against RSV, mpox and smallpox. But the company has no data yet to suggest the vaccine would protect against all three, Peter Costa, Bavarian Nordic’s U.S. medical affairs regional lead, said April 5 during a session in which multiple companies presented data on RSV vaccines and monoclonal antibodies.
Another company, Codagenix, is working with the RSV virus itself, tinkering with its genetic instruction book to make the virus unable to cause disease. For its vaccine, the company’s researchers introduced more than 1,000 mutations in one gene to slow replication of the virus, says Jeffrey Fu, the company’s chief business officer. Those mutations change the virus’s RNA but don’t alter the amino acids in its proteins.
“We’re able to design viruses … that look identical or nearly identical to the real virus,” Fu told me. Because the virus replicates slowly, it doesn’t cause disease but stimulates an immune reaction. The vaccine will be given as nose drops, unlike the other vaccines, which are given as shots.
Codagenix plans to start testing its vaccine’s safety at a low dose in healthy 5-year-olds this spring. If safe, the company wants to gradually increase the dose as well as begin testing the vaccine candidate in younger children, working down to 6-month-olds.
Pfizer’s vaccine is being tested for its ability to protect newborns, babies and older adults. The rest of the companies’ vaccines are for use in older adults.
How well do the RSV vaccines work in newborns and babies?
Only Pfizer is testing a vaccine to protect newborns. And it doesn’t give shots to babies. Instead, the company gave its vaccine candidate to more than 7,300 healthy pregnant women age 49 or younger. The idea is that the mother will produce antibodies against RSV that will transfer through the placenta to the baby. Those antibodies would give babies temporary protection against the virus in the especially vulnerable first six months of life.
Most children get infected with RSV by the time they are 2 years old. The disease may be just a coldlike illness for many kids, with a runny nose, decrease in appetite and a cough. But wheezing or difficulty breathing can also occur, and very young infants might pause breathing for more than 10 seconds. RSV can also lead to more severe illnesses including bronchitis and pneumonia.
Pfizer’s strategy to protect babies from these consequences of RSV seems to have worked. In the 90 days after birth, six infants born to moms who got the vaccine had severe RSV lung infections requiring medical attention. In the placebo group, 33 babies had severe lung infections. That’s a vaccine efficacy of 81.8 percent, researchers report April 5 in the New England Journal of Medicine.
Over time, that vaccine efficacy slipped a bit as mothers’ antibodies wore out. Within six months after birth, 19 babies of mothers in the vaccine group and 62 infants of mothers in the placebo group developed severe lung infections, a vaccine efficacy of about 69 percent.
The vaccine didn’t meet statistical criteria for preventing less-severe lung infections, but there were about half the number of such infections in babies whose mothers got the vaccine compared with babies whose mothers got a placebo. Within 90 days after birth, 24 infants in the vaccinated-mom group and 56 in the placebo group got lung infections. That’s roughly 57 percent efficacy. That efficacy against less-severe lung infections also slipped slightly, to 51 percent, within 180 days of birth.
The vaccine kept babies out of the hospital too. In the first 90 days of life, the vaccine’s efficacy was almost 68 percent at preventing hospitalization, falling to about 57 percent efficacy within 180 days of birth.
Like the COVID vaccines and most vaccines for respiratory illnesses, the vaccine wasn’t great at preventing infection (SN: 5/29/22). The vaccine’s efficacy against any RSV illness requiring medical attention was about 39 percent in the first three months of life and 38 percent in the six months after birth.
As for safety, there weren’t side effects beyond what researchers expected; some pain at the injection site, some muscle aches. “This was a maternal trial, so obviously moms were tired [and] had headaches. You can see that from the placebo numbers,” Barbara Pahud, the clinical lead for Pfizer’s ongoing study, said at the vaccine congress. No serious safety concerns caused by the vaccine appeared during the trial in either mothers or babies.
Pfizer is continuing to follow the children and will have two years’ worth of data to present ahead of an FDA meeting to discuss the vaccine’s approval in August, she said.
Protecting babies
Giving an RSV vaccine to pregnant women helped protect those women’s infants from severe RSV lung infections that required medical attention. Antibodies transferred from the vaccinated mothers were most effective in the first 90 days after birth. The vaccine’s efficacy was 81 percent in that period. As babies’ bodies broke down the antibodies, the vaccine’s efficacy waned a bit, but was still more than 69 percent effective six months after birth.
Cases of severe RSV in babies of vaccinated people vs. a placebo group
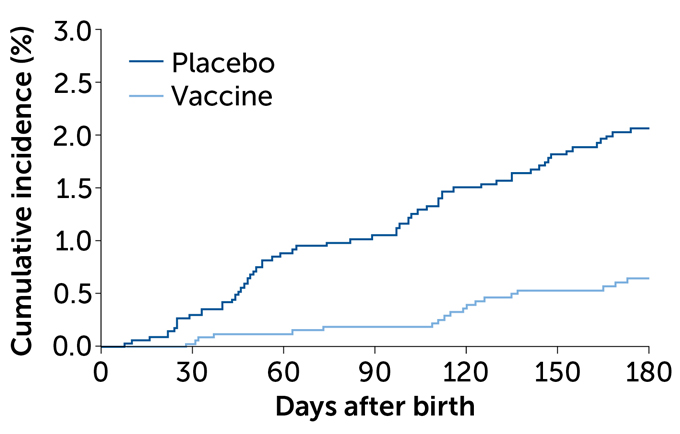
Codagenix has data from lab animal studies suggesting its vaccine can trigger the production of protective antibodies. But its trial in children is just getting started, and there are no results to report yet.
Do monoclonal antibodies help protect newborns and babies?
Giving monoclonal antibodies to newborns and babies might help against RSV too. Like antibodies passed from mothers to babies, lab-made antibodies targeted against the virus’s F protein are showing some signs of success at protecting infants against RSV.
One monoclonal antibody, palivizumab, was approved by the FDA in 1998. But that antibody is used only for babies at the highest risk of severe illness from RSV. That includes babies born prematurely, those with a chronic lung condition called bronchopulmonary dysplasia and infants with certain heart conditions. That’s only a fraction of the babies born in the United States each year. And palivizumab isn’t available in most of the low- and middle-income countries where the virus is the biggest problem, Codagenix’s Fu says.
What’s more, palivizumab doesn’t last long. Vulnerable babies need an injection every month during RSV season. And at more than $1,800 per dose, the medication is expensive.
Some companies have been working on more potent, longer-lasting monoclonal antibodies for use in babies and infants. Sanofi and AstraZeneca teamed up to make one called nirsevimab. That antibody was approved for use in the European Union and the United Kingdom in November. It is being considered for approval in the United States.
In a clinical trial, about 2,000 newborns got an injection of nirsevimab and about 1,000 babies got a placebo. Through 150 days after getting the shot, the antibody’s efficacy against hospitalization was 76.8 percent, researchers report April 5 in the New England Journal of Medicine.
Merck also has a long-lasting monoclonal antibody being tested in clinical trials. Results from those studies aren’t yet available.
Do the vaccines protect older people?
Babies, toddlers and preschoolers are perhaps the population that people worry most about when it comes to RSV, but the virus hits older people hard too.
In the United States alone, between 60,000 and 160,000 older adults are hospitalized with RSV each year, and 6,000 to 10,000 die, the CDC estimates.
In 2019, an estimated 5.2 million people ages 60 or older caught RSV in high-income countries, researchers reported last year in Influenza and Other Respiratory Viruses. Of the 5.2 million cases, 470,000 people landed in the hospital, with about 33,000 of those dying, the researchers estimate. The study looked only at high-income countries, including the United States, Canada, South Korea, Japan and some European countries. But if the kid data are any indication, the death rate for older folks may have been much higher had people in low- and middle-income countries been included.
“This is a relatively unrecognized infection in adult populations,” Edward Walsh, an infectious diseases doctor at the University of Rochester Medical Center in New York, said April 5 at the World Vaccine Congress.
Walsh was one of the lead researchers testing Pfizer’s vaccine for older adults. He and colleagues conducted a large trial involving more than 34,000 people ages 60 and older in Argentina, Canada, Finland, Japan, the Netherlands, South Africa and the United States. Half got Pfizer’s vaccine candidate, and half got a placebo.
The trial started in August 2021. Though RSV reemerged to infect a lot of children that year, it didn’t come back in prepandemic numbers in older adults, especially not in the over-60 crowd, Walsh said. “They continued to stay away from grandchildren, stay away from crowds and wear masks,” preventing transmission.
Walsh told me later that he and colleagues found only 16 percent of prepandemic numbers of infections in older adults in the Rochester area during the study period. With such low numbers of infections, “we were very nervous that [the trial] wasn’t going to show us anything.”
The Rochester area was just one of 240 sites in the study. With the information collected from each site, the researchers had enough data to calculate the vaccine’s efficacy. The researchers considered different levels of severity based on whether the virus infected the lungs and how many symptoms, such as cough, wheezing or shortness of breath, that participants reported.
In the placebo group, 14 participants developed lung infections with three or more symptoms. Only two participants who got the vaccine developed that level of illness for an efficacy of 85.7 percent, Walsh and colleagues report April 5 in the New England Journal of Medicine. Against RSV lung infections with two or more symptoms, the vaccine had an efficacy of 66.7 percent, with 33 cases in the placebo group and 11 in the vaccine group.
Those efficacy numbers are lower but similar to those reported by GSK on February 16 in the New England Journal of Medicine. But results from the vaccine trials are not directly comparable because they were conducted in different countries and used different measurements.
GSK tested its vaccine on about 25,000 participants age 60 and over from 17 countries across five continents. In the trial, seven people who got the company’s vaccine and 40 who got a placebo developed RSV lung infections with two or more symptoms lasting at least 24 hours. That is an efficacy of 82.6 percent. The European Medicines Agency’s committee for human medicines recommended the vaccine for approval on the strength of those data.
Moderna hasn’t yet published results from its vaccine trial in a scientific or medical journal, but it issued a press release in January with the numbers. The company gave its vaccine or a placebo to about 37,000 adults ages 60 and older in 22 countries. Only nine people in the vaccine group got lung infections with two or more symptoms compared with 55 in the placebo group, for a vaccine efficacy of 83.7 percent.
Bavarian Nordic gave healthy 18- to 50-year-olds a shot of vaccine or placebo and then purposely gave them RSV in a human challenge trial (SN: 2/18/21). The vaccine prevented symptomatic infections with 79 percent efficacy, the company reported in a press release in 2021. But that was among healthy younger adults who have less risk of severe complications than elderly people do.
Bavarian Nordic also conducted a clinical trial in the United States and Germany of 20,000 people age 60 and older. Results of the study should be available later this year, Costa said.
Without masking and social distancing, RSV probably isn’t going to disappear again. As for the new vaccines and monoclonal antibodies, they probably won’t stop RSV’s spread. But they may at least protect the most vulnerable among us against the virus’s worst effects.








