A brain chemical tied to narcolepsy may play a role in opioid addiction
Heroin and other opioids increase the amount of hypocretin-producing nerve cells
SIDE EFFECTS Long-term use of opioids, such as heroin, increases the number of brain cells that release a molecule called hypocretin that’s known to regulate wakefulness.
Thomasaf/iStockphoto
Using opioids gives some brain cells a call to action.
Opioid addicts’ brains, examined after death, contain about 50 percent more nerve cells that release a molecule called hypocretin, compared with people who didn’t use the drugs, a new study finds. Giving the opiate morphine to mice also induced similar changes in their brains. But the increase didn’t come from new nerve cells, or neurons, being born. Instead, once-dormant neurons appear to rev up their hypocretin machinery in response to the addictive drugs, researchers report June 27 in Science Translational Medicine.
The findings fit with a growing body of research that suggests that hypocretin, a brain chemical that regulates wakefulness and arousal, may also be involved in addiction.
“I think there is extensive evidence now that shows that the hypocretin neurons are supporting motivated behavior in general,” and addiction falls under that umbrella, says Rodrigo España, a neurobiologist at Drexel University in Philadelphia who wasn’t involved in the new study. For example, his lab recently showed that rats with a less sensitive hypocretin receptor (and therefore a weaker response to the brain chemical) showed less motivation to seek out cocaine rewards.
The new study comes from the opposite angle, showing changes in hypocretin neurons in response to drug use, rather than the other way around. “It does suggest the possibility that part of the reason it’s so hard to get off drugs is there’s this massive change in the brain,” says study coauthor and neuroscientist Jerome Siegel of UCLA.
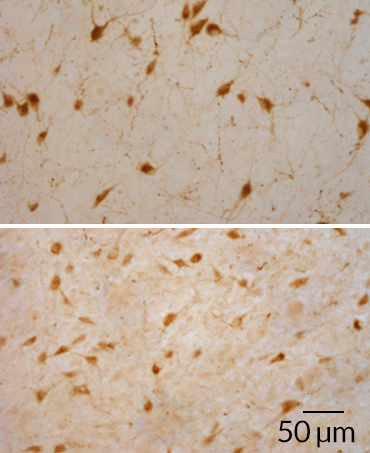
Now, analysis of four more brains from people addicted to heroin and other opioids suggests that the elevated number of hypocretin neurons in that first brain wasn’t a fluke.
Addicts’ brains had 54 percent more hypocretin-producing neurons, on average, than healthy controls, the team found. Follow-up experiments in mice showed that morphine, when given to mice for two weeks, increased the number of hypocretin-producing neurons in their brains. Narcoleptic mice’s symptoms even disappeared when injected with morphine.
The findings suggest that, with proper dosing and monitoring, opioids might be an effective treatment for some of the roughly 200,000 people in the United States who have narcolepsy, Siegel says. In the past few years, opioid prescriptions have come under increased scrutiny because of the risk of addiction and the nationwide opioid epidemic (SN: 1/20/18, p. 8). Historically, he says, people with narcolepsy have been treated with addictive stimulant drugs, such as methamphetamine, and haven’t shown the same desire to keep upping the dose that’s seen in addicts.
Further testing is needed to determine whether opioids are actually more effective than other, less addictive drugs given for narcolepsy today.







