What experts know so far about COVID-19 boosters for immunocompromised people
A third dose might help better protect some, but the CDC is still deciding on official guidance
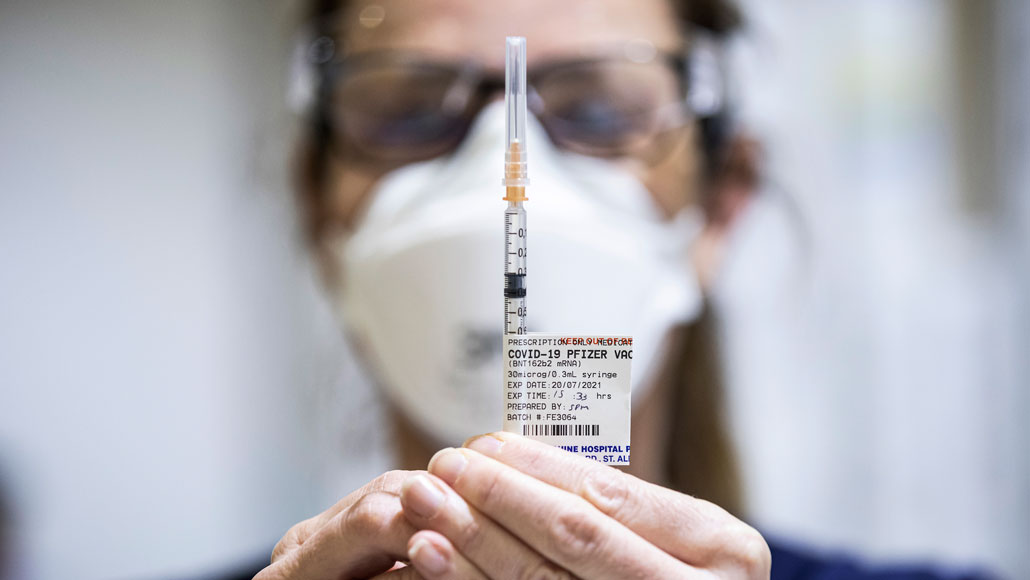
A staff member at the Melbourne Showgrounds in Australia prepares a Pfizer COVID-19 vaccine dose. While Australia, the United States and other countries focus on vaccinating the unvaccinated, France and Israel are also offering booster shots to immunocompromised individuals.
Daniel Pockett/Getty Images
People with weak immune systems don’t always mount strong defenses against the coronavirus, even after being fully vaccinated. A third COVID-19 vaccine dose might help protect some immunocompromised people, evidence suggests. But for now, there’s not enough data to say how much such a shot might help, experts with the U.S. Centers for Disease Control and Prevention said July 22. As a result, the agency isn’t yet recommending a third dose and says that vaccinated people in this group should keep wearing masks.
With global COVID-19 cases on the rise, finding ways to protect millions of immunocompromised people who are at high risk for severe disease is crucial. In the United States, an estimated 2.7 percent of adults, or 6.8 million people, are immunocompromised.
Studies suggest that until transmission of the coronavirus is squashed, millions of organ transplant recipients, cancer patients undergoing treatment and others are still susceptible to severe COVID-19, even if they are lucky enough to have access to shots (SN: 2/26/21). Of 45 vaccinated people admitted to 18 U.S. hospitals for COVID-19 from March 11 to May 5, twenty, or 44 percent, were immunocompromised, according to data presented in a July 22 meeting of the CDC’s Advisory Committee on Immunization Practices.
A third dose of COVID-19 vaccines can boost coronavirus-fighting antibodies in the blood of some immunocompromised patients, laboratory studies suggest. But it’s still unclear whether specific groups might benefit more than others and how effective extra doses might be at preventing severe COVID-19. The immune system, for instance, has more than antibodies in its arsenal to attack the coronavirus and prevent severe disease (SN: 1/27/21). Studies from the real world would provide a clearer picture for how well additional doses might work, and for which groups.
At the very least, an additional dose appears safe for immunocompromised individuals, epidemiologist Sara Oliver of the CDC said at the July 22 meeting. For example, a study that included patients on dialysis for kidney disease showed that “symptoms reported after the third dose were consistent with what has been seen after the second dose,” Oliver said. Most vaccine side effects — such as fatigue, pain at the injection site, chills or soreness — were mild.
While U.S. officials are still discussing the benefits of the additional dose, some countries have already taken steps to get those doses to immunocompromised residents. Severely immunocompromised people in France, for instance, can get a third dose a month after their second dose, officials announced April 11. Officials in Israel announced July 11 that they too would begin giving immunocompromised individuals a third shot. And officials in the United Kingdom have proposed distributing additional doses between September and December.
Here’s a summary of what studies have found so far about the merits of an extra COVID-19 shot for the immunocompromised:
- A third dose of a COVID-19 vaccine — either Pfizer’s, Moderna’s or Johnson & Johnson’s — boosted the antibody levels of some organ transplant recipients with previously weak responses to the vaccine, researchers reported June 15 in Annals of Internal Medicine. Of 30 vaccinated patients, six people had low levels of antibodies that recognized the coronavirus before getting a third dose. Another 24 did not have detectable antibodies. Two weeks after their third shot, all six patients with initially low antibody levels now had high amounts. Of the 24 people without antibodies, 16 still didn’t develop any, two had low levels and six developed high levels of antibodies.
- Another study showed that 67 out of 99 organ transplant recipients vaccinated with Pfizer’s jab had detectable antibodies after a third dose, researchers reported June 23 in the New England Journal of Medicine. That’s compared with four of 101 individuals after a first dose and 40 of 99 after a second. Of the 59 people who didn’t have antibodies after the second dose, 26, or 44 percent, mounted the immune proteins after the extra dose.
- More than 75 percent of blood, or hematopoietic, stem cell transplant recipients had detectable antibodies after two doses of Pfizer’s COVID-19 vaccine, researchers reported July 13 in the Lancet. Fifty-two of the 88 patients in the study had antibody levels above a threshold that corresponds to how well the immune proteins stop the coronavirus from infecting cells. Those who had received the transplant more than a year before getting vaccinated, and who had high numbers of pathogen-fighting white blood cells, were more likely to have lots of antibodies. Patients given treatments that suppressed their immune systems within three months of getting vaccinated, on the other hand, had low antibody levels, the team found. A third dose might be helpful for that group, but experts don’t know yet.
- Third doses can also help some patients on dialysis for kidney disease, studies suggest. Of 12 dialysis patients who initially didn’t generate antibodies after two vaccine doses, half mounted an antibody response after an extra shot, researchers reported in a preliminary study posted July 6 at medRxiv.org. Forty-two percent, or 5 out of 12 antibody-negative patients, had antibodies after a third vaccine, another group of researchers reported May 31 in Nephrology Dialysis Transplantation.
In the United States, a recommendation for an additional dose for immunocompromised people probably won’t come unless the Food and Drug Administration permits extra doses under current emergency use authorizations for COVID-19 vaccines or until the agency fully approves the vaccines for widespread use, CDC officials said during the meeting. For now, the health agency isn’t aware of any data submitted to the FDA that might support such a change to the emergency use authorizations, the officials said.
In the meantime, experts are keeping a close eye on emerging data about additional doses. “However, while we do that, we need to remember what we can do now,” Oliver said. That means immunocompromised people should continue to wear masks, stay six feet away from others and avoid crowds or indoor spaces.
Sign up for our newsletter
We summarize the week's scientific breakthroughs every Thursday.







