Dying to Sleep
Getting too little sleep can impair body and brain and could even be deadly
For many people, days just don’t seem long enough. In order to cram everything into one 24-hour period, something has to give. Judging by many surveys of Americans, it’s sleep.


Sleep is regarded by some as unproductive, wasteful downtime. People who would rather hit the hay than the dance floor are told that only losers snooze and that they can sleep when they’re dead.
But new data about sleep’s benefits suggest that losing sleep might speed up death’s arrival. Recent research also shows that people who don’t snooze enough face a higher risk of losing their health than those who regularly get a good night’s sleep.
“What is certain is that we can’t do without sleep,” says Peter Meerlo, a neuroscientist at the University of Groningen in the Netherlands.
Some of the consequences of lost sleep are immediate, obvious and unpleasant, such as a toddler’s crabbiness after missing a nap. Older children and adults get irritable when tired, too. Sleepy students don’t learn or perform as well as their well-rested peers (SN: 09/09/06, p. 174). And nodding off at work probably won’t help anyone get a promotion.
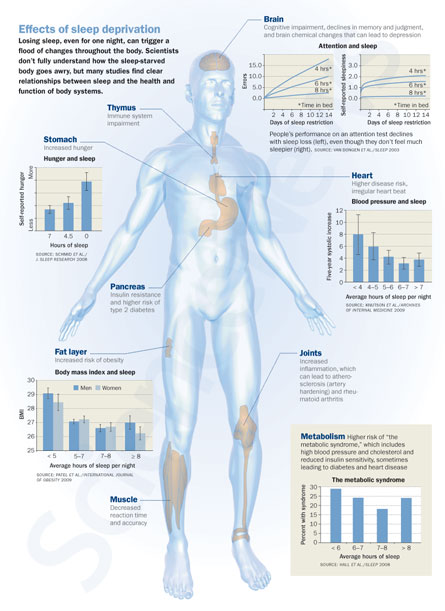
Other penalties for staying up too late can be far more serious, even deadly. Studies have linked chronic sleep loss to obesity (SN: 11/17/07, p. 318; SN: 4/1/06, p. 195), heart disease, high blood pressure, diabetes (SN: 1/3/09, p. 5; SN: 1/19/08, p. 46) and shorter lives (SN: 2/8/03, p. 85) in people and laboratory animals. And now, a new study links sleep loss in mice to Alzheimer’s disease plaques (SN: 10/24/09, p. 11). And some evidence suggests that stinting on sleep night after night may cause long-term — maybe even permanent — changes in the brain, some of which may predispose people to mental disorders such as depression.
Just one night of short sleep has been shown to increase levels of inflammatory chemicals in the blood (SN: 10/11/08,p. 14) and increase hunger-promoting hormones. A week of getting just two hours less sleep per night than usual changed the way people in one study responded to glucose, mirroring a change seen in people who develop diabetes.
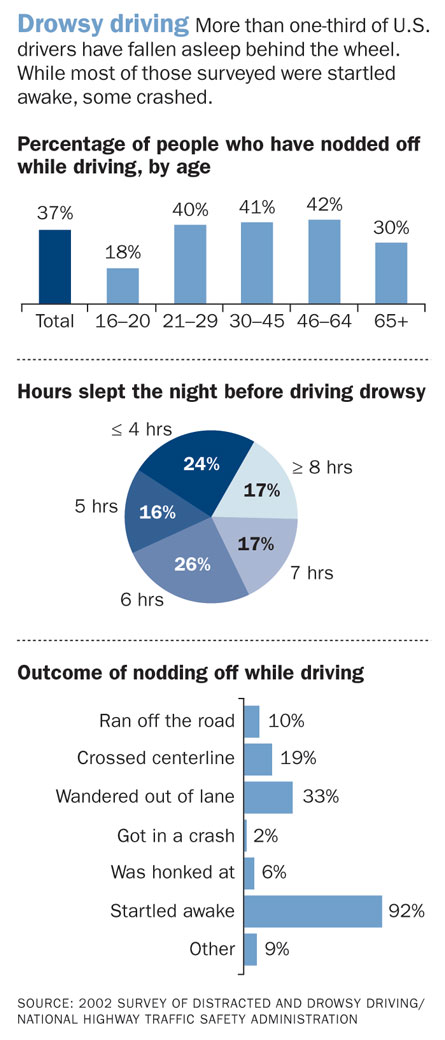
And lack of sleep can also have immediate injurious or fatal consequences: The National Highway Transportation Safety Administration estimates that drowsy-driving crashes result in about 40,000 nonfatal injuries and 1,550 deaths each year, probably a conservative estimate. Now, scientists are trying to understand not only how sleep deprivation affects driving performance, but also why one sleepy person might drive fine while another becomes a road menace.
Too tired to function
Nodding off behind the wheel is a common occurrence in David Dinges’ lab at the University of Pennsylvania School of Medicine in Philadelphia.
Dinges and his colleagues limit volunteers’ time in bed to four hours a night for five nights, then let the volunteers sleep up to 10 hours for two days. The aim of the experiments is to learn more about how the brain responds to the kind of chronic sleep deprivation people experience in real life, and to find out how much sleep is needed to repay the debt.
In the dimly lit laboratory, a volunteer named Heather sits behind the wheel of a driving simulator with electrodes taped to her head. She pushes the accelerator so that her virtual car buzzes along at just over 60 miles per hour on a dark road illuminated only by her headlights. White poles flash by. Suddenly, around a bend, the back of a large cargo truck looms in the darkness. Heather quickly brakes to avoid colliding with the slow-moving truck.
For each of the past four nights, Heather has gotten just four hours of sleep. “My limbs feel heavy,” she reports. She isn’t used to this curtailed sleep schedule. “I never stay up all night,” she says. “I always get my sleep.” She is forgoing shut-eye for a study of genetic differences that may affect people’s responses to sleep deprivation.
The electrodes on Heather’s head are monitoring her brain waves and eye movements so that researchers can detect even brief bouts of sleep. But despite feeling tired, “a little light-headed and dizzy,” Heather hasn’t nodded off when she’s not supposed to, and her performance on the driving simulator and other tests hasn’t deteriorated from her well-rested showing.
The tests in Dinges’ lab have shown just how severely most people’s performance of daily activities can deteriorate with sleep loss. But Heather may be one of a few rare people whose brains don’t become mush when deprived of sleep. By figuring out which genes keep Heather’s brain functioning despite so little sleep, researchers may be able to develop drugs that affect those genes and help ordinary people resist making sleepy mistakes.
James, an architecture student, routinely pulls all-nighters, especially at the end of a semester. He expected to feel horrible after missing out on four hours of sleep each night for several days. “I thought I was going to be like a zombie, not able to process things and short-tempered,” he says. But despite the lab’s dim lighting, “I’m functioning,” he says.
Functioning perhaps, but not as well as he does when well-rested. On this day, he fell asleep while driving the simulator. He woke up to find that he’d smashed into the back of a truck.
James is certainly not alone in misjudging his ability to function while sleepy. Despite evidence to the contrary, many short-sleepers are convinced that they function well on less sleep, Dinges says. One constant is that people are generally not good at predicting how well they will perform when deprived of sleep.
Driving while drowsy was a contributing factor in more than 20 percent of the crashes and near-crashes recorded in a study by researchers at Virginia Tech in Blacksburg. The team fitted 100 cars with cameras and sensors and then recorded drivers’ actions for about a year. A drowsy driver was four to six times more likely to have a crash or near-crash. In contrast, reading, putting on makeup and dialing a cell phone increased crash risks threefold, the researchers found.
No one could have predicted Heather’s and James’ individual responses to sleep deprivation, Dinges says. In his studies, he has found that some people fall apart after missing just a few hours of sleep. Others, like James, show a slow, steady decline in their ability to remain vigilant and sharp on tests as their sleep is cut short over the course of five days. Then there are the people Dinges refers to as “type 1s,” like Heather. Those people’s performance on a variety of attention and response-time tests doesn’t change with five days of restricted sleep. “People are walking around with grossly different brain activity profiles,” Dinges says.
How much is enough
No magic number exists for the amount of sleep people need each night. The “normal” range includes as little as six hours (SN: 9/12/09, p. 11) and as much as 10 hours of sleep per night, depending on the person. But studies of various diseases show that sleeping about seven to eight hours each night carries the least risk of obesity, diabetes, heart disease and other illnesses.
Whatever the need for sleep is, many people don’t get enough. In fact, Americans are sleeping less than ever before, according to the National Sleep Foundation, which conducts periodic surveys of sleep habits. In 2009, 20 percent of survey participants said that they slept less than six hours on weeknights, compared with 12 percent in 1998. That lost sleep isn’t being recovered on weekends, either. On average, respondents in 2009 reported sleeping 7.1 hours on weekend nights, down from an average of 7.8 hours in 1998.
Humans are the only animals that willingly deprive themselves of sleep, says Eve Van Cauter, a sleep researcher at the University of Chicago. “You cannot put a rat in front of the television, give him the remote and tell him, ‘you have to stay awake,’” she says.
People think that they are just too busy to bother with sleep. “We are ignoring that sleep, like exercise and proper feeding, is crucial for health,” Van Cauter says.
Those respondents who slept less than six hours a night were also less likely than people who slept eight hours or more to say that they work well and efficiently, eat healthy diets, engage in leisure activities, exercise or have sex. Short-sleepers also were more likely to smoke, drink caffeinated beverages and eat high-sugar or high-carbohydrate foods.
An analysis of several population studies worldwide showed that children who sleep less than 10 hours a night are nearly twice as likely to be obese compared with children who slept more than 10 hours. The study, published last year in Sleep, also showed that short-sleeping adults (those who got less than five hours of sleep per night) were more likely to be obese, with body mass index increasing with each hour of lost sleep.
Some data suggest that people who sleep far more than average are also at risk for health problems. Both short- and long-sleepers were more likely to have symptoms of “the metabolic syndrome,” a cluster of conditions — including high blood pressure, high cholesterol levels and reduced sensitivity to insulin — that presage diabetes and heart disease.
Among people who get seven to eight hours of sleep each night, only 17 percent had such symptoms, researchers from the University of Pittsburgh and collaborators reported last year in Sleep. But almost a quarter of people regularly sleeping more than eight hours a night had the symptoms, and nearly a third of those getting less than six hours of sleep nightly did too, the researchers reported.
Both short- and long-sleepers were also at higher risk for diabetes than people who sleep seven hours on average, shows another study led by researchers at Columbia University and published in Sleep in 2007.
Most people are fooling themselves if they think they need less sleep than average, Van Cauter says. A study of healthy young adults, published in 2005 in Sleep, seems to back her up. Volunteers were given the opportunity to get some extra shut-eye for three days in a study conducted by researchers at Harvard Medical School in Boston and the University of Surrey in Guildford, England. Everybody slept more the first day of the study, but by day three, people who normally sleep more than nine hours a day had maxed out their sleep. People who normally slept less continued to catch extra z’s. The researchers concluded that people with shorter sleep times probably carry a bigger sleep debt than others, one that couldn’t be paid back in three days.
Sleeping in your genes
Researchers would dearly love to know what makes people like Heather resistant to the attention-degrading effects of sleep loss. (Though scientists don’t know whether these people’s bodies hold up against sleep deprivation as well as their brains do.) Studies of twins suggest that a large part of the resistance is genetic: Identical twins’ responses to sleep deprivation are as similar to each other as an individual’s results in repeated tests.
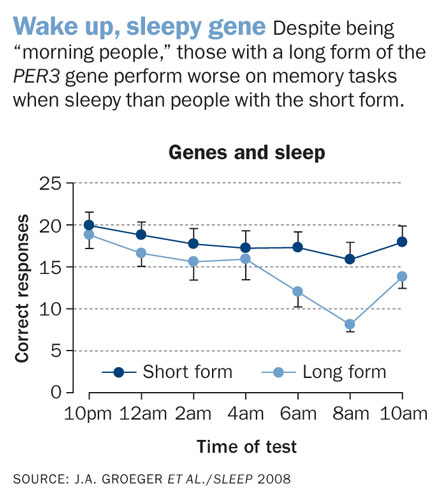
Previously, researchers reported that a gene called PERIOD3, or PER3, might be involved in the response to sleep deprivation (SN: 3/24/2007, p. 190). PER3, a cousin of genes involved in the circadian clock, which governs daily body rhythms including meal times and bedtimes, comes in two common forms. The more common form contains four repeats of a segment of the gene, and a less-common variant contains five repeats of that segment. People who have inherited two copies of the longer form tend to be morning people, while people with two copies of the shorter form tend to be night owls.
When their circadian alertness level was at its lowest daily point, sleep-deprived people with the long form performed worse on some tasks than people with the short gene, researchers led by Derk-Jan Dijk at the University of Surrey reported in 2008 in Sleep. Many researchers interpret that result to mean that the long form of the gene makes people more vulnerable to sleep deprivation.
But people with different forms of the PER3 gene didn’t show any differences in responses to partial sleep deprivation over five nights in a study by Dinges and colleagues published online June 11 in PLoS ONE. The two results can’t be directly compared, because the volunteers in Dinges’ study were asleep during the time of day that the Surrey group found differences in performance. So the jury is still out on whether PER3 protects some people against the effects of sleep deprivation, and researchers are hunting for other genes that may contribute to differences in sensitivity to sleep loss.
No snooze, you lose
All the consequences for chronically missing out on slumber aren’t yet known, but some studies suggest sleeping too little for too long can change the brain. In a study in rats, Meerlo examined serotonin — a brain chemical thought to be important in sleep, depression and many brain functions. The researchers didn’t find any changes in the rats’ brains after a single night of sleep loss, but after a week of getting shortchanged, the rats’ brains became less sensitive to serotonin. Such changes could make rats, and people, more prone to developing depression, Meerlo says.
As bad as that news potentially is, Meerlo has worse news. Even after he let the rats sleep in on the weekend, their brains still didn’t respond to serotonin as effectively as before sleep deprivation, Meerlo and his colleagues reported last year in Sleep.
Even more disturbing is the finding from a study of sleep deprivation in rats conducted by researchers at Northwestern University in Evanston, Ill. The researchers found that rats deprived of about 35 hours of sleep over five days — an extreme sleep loss — didn’t make up that lost sleep when given three days to do nothing but sleep. The result, reported in the Proceedings of the National Academy of Sciences in 2007, suggests that chronic sleep loss may actually prevent the body from sleeping more to recover.
“That would limit your ability to make up your sleep debt,” Van Cauter says.
And sleep deficit is a debt you can’t afford, Meerlo says. “One night of missed sleep isn’t going to kill you,” he says, “but the danger is that if you’re not getting enough sleep night after night, small cumulative effects could add up.”
So while you may be dying to stay up one more hour to finish reading that chapter or reach one more level on that video game, researchers say that in the long run, you could be inching closer to a state of permanent rest.