Scientists are seeking new strategies to fight multiple sclerosis
To find clues to origins of MS, researchers look beyond the immune system
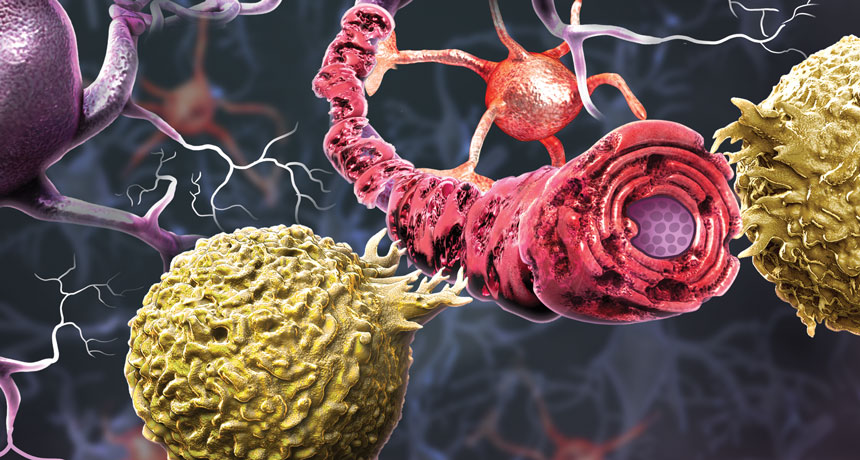
BREAKING DOWN MULTIPLE SCLEROSIS Taking narrow aim at the immune system isn’t enough, so researchers are looking for new treatment targets within nerve cells and even in the gut.
Nicolle Rager Fuller
James Davis used to be an avid outdoorsman. He surfed, hiked, skateboarded and rock climbed. Today, the 48-year-old from Albuquerque barely gets out of bed. He has the most severe form of multiple sclerosis, known as primary progressive MS, a worsening disease that destroys the central nervous system. Diagnosed in May 2011, Davis relied on a wheelchair within six months. He can no longer get up to go to the bathroom or grab a snack from the fridge.
Davis hoped life might improve when he was chosen in 2012 to participate in a clinical trial of a drug called ocrelizumab. The drug offered a first sliver of hope for patients waiting for a cure, or at least something to slow down the disease’s staggering march. Early research suggested the drug could help some of the roughly 60,000 people in the United States, like Davis, suffering from primary progressive MS. The drug also held promise for patients with the other major form of the disease, relapsing-remitting MS, which afflicts about 340,000 people nationwide.
For some people, ocrelizumab seemed to work. Brain scans of patients with primary progressive MS showed fewer signs of damage and the patients’ ability to walk deteriorated more slowly than in individuals who received a placebo, researchers reported in January in the New England Journal of Medicine. The drug also helped people with relapsing-remitting MS, which, as the name implies, includes shifts between disability and wellness. Over a year’s time, these patients experienced about half as many flare-ups as those taking another commonly prescribed drug, a different research group reported in the same issue of the journal.
Ocrelizumab was heralded as a breakthrough, and in March, the U.S. Food and Drug Administration approved it as a treatment for primary progressive and relapsing-remitting MS. Genentech now sells the drug as Ocrevus.
“We finally have an approved therapy for primary progressive MS,” says Fred Lublin, a neurologist at the Icahn School of Medicine at Mount Sinai in New York City. The first drug to treat relapsing-remitting MS came on the market in 1993, Lublin notes. Now, nearly a quarter century later, there’s something that helps some people with the most aggressive form of the disease.
With that hopeful note, though, comes frustration. Ocrevus isn’t a cure, and it offers no relief for 30 to 40 percent of patients with primary progressive MS. Davis was in that disappointed group.
In fact, none of the 15 FDA-approved drugs for MS, which all modify or suppress the immune system, actually stop the disease. The drugs only reduce the number and severity of flare-ups and, in some cases, slow the visible marks of brain damage.
“Multiple sclerosis is arguably the most complex disease ever described,” says Sergio Baranzini, a geneticist at the University of California, San Francisco. The disease is so complicated, he says, because it involves two of the body’s more complex systems — the nervous and immune systems. Scientists don’t yet have a good handle on where the damage begins. Does a problem in the nervous system spur an immune response that leads to additional damage to the brain and spinal cord? Or does the immune system attack first, dispatching disease-fighting cells into the brain, where they batter and kill nerve cells? What causes the initial nerve damage or incites the immune attack is still a big question. Scientists aren’t even clear whether multiple sclerosis is a single disease or a multitude of maladies.
With so many unanswered questions, researchers have begun looking for potential treatment strategies outside the immune system. Targeting problems in the nervous system, together with the harmful immune reactions, is essential, scientists say. Some researchers have begun scrutinizing the malfunction of specific organelles within nerve cells, or neurons. Others are analyzing the gut’s community of microorganisms, its microbiome, which is considered a bridge between the environment and the body. Those researchers are following up on observations that environmental influences play a role in MS. The research is in early stages. But for a challenging disease like MS, attacks on multiple fronts may be exactly what it takes to help Davis and others who are running out of time.
Story continues after graphic
Doing damage
One clear characteristic of MS is scarring of myelin, the protective substance surrounding the axons that extend from nerve cells. When immune cells attack myelin, nerve cells can’t send their signals.
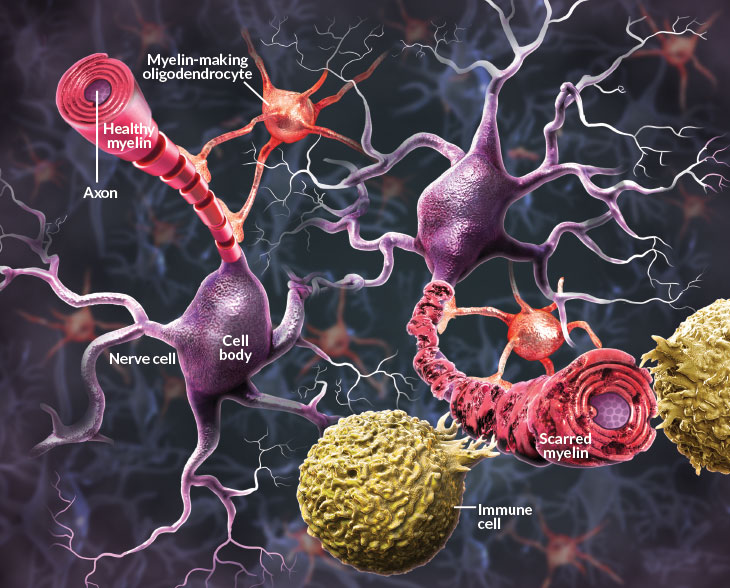
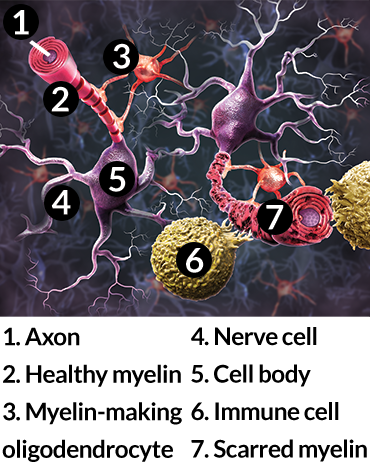
Disrupted signals
More than 2.3 million people worldwide suffer from multiple sclerosis, according to 2013 data, the most recent, from the MS International Federation in London. The disease affects people of all ages, and is more often diagnosed in young adults, women and people who live in northern latitudes. Certain gene variants are associated with an increased risk of disease, but MS is rarely directly inherited. In studies of identical twins, if one has MS, the other’s risk increases by about 25 percent. But if a parent has MS, a child’s risk of developing the disease is only 2.5 to 5 percent higher than in children of people who don’t have MS.
Like Davis, most patients learn they have the disease after experiencing tingling or numbness in the fingers or toes, loss of balance or trouble walking. Vision problems are another early sign. Such symptoms are a result of faulty electrical signals in the central nervous system. Those signals are disrupted because myelin, the insulating sheath around a nerve cell’s message-transmitting axons, becomes damaged. Many researchers think that breakdown is driven by the body’s immune system: Immune cells flock to the brain, causing inflammation and myelin destruction, which leads to continued nerve cell damage. Depending on the damage and how quickly it accumulates, patients are diagnosed either with the primary progressive form, with a relatively quick decline in health, or the relapsing-remitting form. About half of people with the intermittent form eventually move into the progressive disease, typically within about a decade.
Overworked organelles
Because most if not all people with MS experience nerve cell damage, researchers have begun to focus on two organelles within the neuron’s cell body: the power-generating mitochondria and the labyrinth-like endoplasmic reticulum, which makes many of the proteins, lipids and other molecules needed by the cell. These organelles keep a nerve cell running, but in MS, they are pushed into overdrive, working much harder than they should.
Over the last 20 years, researchers have linked malfunctions in mitochondria to neurodegenerative disorders such as Alzheimer’s and Parkinson’s. More recently, MS has joined the list. In a study published in January in the Journal of Neuroinflammation, cellular biologist Thomas Simmen of the University of Alberta in Edmonton, Canada, and colleagues revealed at least one way that mitochondria in nerve cells fail in people with MS.
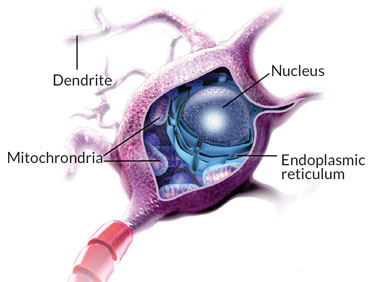
In nerve cells, Rab32 is a troublemaker. It gloms on to the surfaces of the endoplasmic reticulum and mitochondria, controlling the organelles’ interactions and mitochondrial behavior. In separate experiments, when Rab32 rises in response to stress in the endoplasmic reticulum, or ER, several things happen: The nerve cell fibers (both axons and the message-receiving dendrites) are shorter, mitochondria are bulkier than normal and their numbers spike. These changes indicate that the mitochondria are not working correctly, says Paul Eggleton, an immunologist at the University of Exeter in England and a coauthor of the study. Eventually, the nerve cell commits suicide.
The researchers call Rab32 a marker of MS progression. Other proteins are involved, which Simmen and Eggleton hope to identify. If researchers could develop drugs that target those proteins, perhaps they could stop nerve cell death and prevent MS from progressing, the two scientists say. However, scientists still want to figure out what causes the ER stress that leads to the protein rise. Simmen suggests that it could be a yet-to-be-determined defect with the endoplasmic reticulum itself.
Figuring out how that stress starts is important, as it ties into one of the major characteristics of MS: damage to myelin.
Making myelin
Oligodendrocytes are the central nervous system cells that make myelin. One mature oligodendrocyte can coat about 50 axon segments with myelin. Like spiders, the oligodendrocytes sit alongside nerve cells tending to their myelin webs. When there’s damage to myelin, oligodendrocytes repair it, or new oligodendrocytes take over for old ones.
But in people with MS, some oligodendrocytes stop making myelin altogether and young oligodendrocytes have trouble maturing. Most researchers think an immune attack blocks the oligodendrocytes from doing their job. But recent work raises questions about that idea.
In experiments in mice, researchers used a toxin to destroy myelin and kill oligodendrocytes. The mice had difficulty running on a spinning rod and showed other symptoms of nerve cell deterioration. Five weeks after the toxin injection, the neurological symptoms were at their worst, suggesting the toxin did its job. At 10 weeks, the mice recovered, probably because the brain can heal itself, says study coauthor Brian Popko, a neurologist at the University of Chicago. The brain creates new oligodendrocytes that wrap fresh myelin around the affected axons, Popko and colleagues reported in January 2016 in Nature Neuroscience.

Popko says myelin-making cells are damaged regularly in healthy individuals and in those with MS. “Our idea is that these hits to the central nervous system in most people do not have long-term detrimental effects,” he says. But people with MS have trouble making new oligodendrocytes and so, “central nervous system insults can lead to the development of the disease.”
Popko and others are testing an approach to stop disease development: preserve oligodendrocytes’ ability to handle stress.
Strengthening nerve cells
Oligodendrocytes have mitochondria and an endoplasmic reticulum too. If oligodendrocytes are making myelin in an environment with a lot of inflammation, as seen in MS patients, then the ER must work extra hard to make proteins to rebuild myelin and respond to surrounding inflammation. The cells eventually can’t keep up, so they program their own death.
Preventing the ER from being overwhelmed and signaling cell suicide could be a strategy to treat MS, Popko wrote, along with University of Chicago neurologist Sharon Way, in a 2016 review article in Lancet Neurology. That’s the aim of two drugs currently in testing. The drugs keep the ER working at a comfortable level, even during stress.
One of the drugs, Guanabenz, is a hypertension medication. In animal studies, the drug kept oligodendrocytes alive, easing MS symptoms and even delaying their onset. But there were side effects, including drowsiness and lethargy, effects sometimes experienced by people with high blood pressure who take the drug. An early trial in MS patients recently ended, but results haven’t been reported yet. A second potential drug, Sephin1, which is still in animal testing, keeps oligodendrocytes alive without the side effects of Guanabenz, Popko says. Another drug, salubrinal, also designed to reduce ER stress, wasn’t as effective in lab tests as researchers had hoped, he says, so testing has stopped.
Cleveland Clinic neuroscientist Ranjan Dutta says it is not clear that an overstressed ER and resulting mitochondrial failure, causes MS. There is no question mitochondria are defective in individuals with MS, he says. But the problem may be that the organelles cannot keep up with the energy demand of the cell as it tries to fend off an immune attack. And, if the immune attack comes first, as Dutta and Lublin suspect, what is the trigger?
Drug options
Fifteen medications are available to treat multiple sclerosis, each suppressing the immune system (five are described below). At least a dozen other drugs (two listed) are in various stages of development.
Available to patients
| Drug | Mode of action | Year approved |
|---|---|---|
| Betaseron® (interferon beta-1b) | Cell-signaling protein that boosts anti-inflammatory and reduces pro-inflammatory molecules in the brain | 1993 |
| Novantrone® (mitoxantrone) | Chemotherapy drug that blocks creation of immune cells (T cells, B cells and macrophages) | 2000 |
| Tysabri® (natalizumab) | Monoclonal antibody that prevents T cells from crossing into the brain | 2006 |
| Gilenya® (fingolimod) | Small molecule that prevents T cells from crossing into the brain | 2010 |
| Ocrevus™ (ocrelizumab) | Monoclonal antibody that triggers death of B cells | 2017 |
In development
| Drug | Mode of action | Phase of testing |
|---|---|---|
| Guanabenz | Hypertension drug that protects cell from endoplasmic reticulum stress and preserves oligodendrocytes and myelin during inflammation | Early human studies |
| Sephin1 | A derivative of the drug Guanabenz with the same action but fewer side effects | Animal testing |
Sources: National MS Society; S.W. Way and B. Popko/Lancet Neurology 2016
Going with the gut
The gut is where the immune system learns about what’s going on outside the body, says UCSF’s Baranzini. Environmental factors are known to increase risk for MS (SN: 4/16/16, p. 4). Such factors include smoking and low levels of vitamin D in the blood (which may explain why MS is more common at higher latitudes, since sun exposure boosts vitamin D).
“We see the microbiome as a window into the environment,” Baranzini says. With that in mind, he and colleagues compared the gut bacteria of 71 people with relapsing-remitting MS with bacteria from 71 healthy people. Two bacterial groups, Acinetobacter and Akkermansia, were four times as abundant in MS patients as in healthy individuals. Another bacterial group, Parabacteroides, was four times as abundant in people without the disease.
Next, the team exposed immature immune cells from the blood of healthy people to the bacteria found in the guts of MS patients. When the immune cells encountered Acinetobacter and Akkermansia, they matured into the T helper cells that trigger inflammation. Acinetobacter also tamped down regulatory T cells, which keep autoimmune diseases at bay.
When the researchers transferred gut microbes from MS patients or their healthy spouses into mice that had an MS-like condition, the mice given the MS gut microbes got much sicker, Baranzini and colleagues reported in the Oct. 3 Proceedings of the National Academy of Sciences.
“It was surprising to see that the differences in bacteria were enough to cause immunological imbalances in the mice,” he says. “It implicates the gut microbiome as a cause of MS.”
Dutta and other scientists are not yet convinced. Microbiome studies are “encouraging, despite early days,” Dutta says. He notes, however, that researchers need to develop more rigorous ways to test the role of the gut microbiome in controlling immune reactions. “This is primarily because of the difference between the mouse and human immune systems.” It will also be important to know how the bacteria operate to affect the immune system, he adds.
The results aren’t completely unheard of. In the same issue of PNAS, researchers found higher levels of Akkermansia in twins with MS versus their healthy sibling. The scientists transferred the twins’ gut bacteria to mice predisposed to develop a disease that mimics MS. Twelve weeks after the transplant, about 40 percent more mice with gut microbes from a twin with MS developed brain inflammation compared with mice that got gut microbes from a twin without disease.
If researchers can get a handle on the gut microbiome’s role, Baranzini can imagine a day when probiotics can be used to shift the composition of microbes in the gut to reduce inflammation. But more work needs to be done, and at least one major question needs answering: Do people with relapsing-remitting MS have a different set of gut bacteria than people with the primary progressive form of the disease?
“We’re doing that experiment right now,” Baranzini says. He also hopes to expand his analysis to include MS patients from around the world, who eat different diets and may have different gut bacteria, to help pinpoint the microbes that may be contributing to the disease.
MS drugs that target the immune system provide some benefit by reducing relapses, but these drugs can’t seem to prevent long-term neurodegeneration, Popko says. Combining current drugs with strategies to protect oligodendrocytes, enhance myelin-making and possibly wrangle the immune system through the gut might be the best strategy for achieving prolonged benefit for people with MS.
This story appears in the December 9, 2017 issue of Science News with the headline, “Breaking Down Multiple Sclerosis: Researchers seek solutions beyond the immune system.”






