U.S. measles outbreaks show no signs of slowing down
International travel and hot spots where too few people are vaccinated is fueling the spread

SHOTS HERE The Rockland County Health Department in New York offered free vaccines on April 5 in the midst of an ongoing outbreak there. According to the department, 81 percent of the 184 cases in the county were in individuals who were not vaccinated.
JOHANNES EISELE/AFP/Getty Images
The year has just started, but it’s already a bad one for measles. The viral disease has sickened at least 555 people in 20 states, according to numbers released April 15 by the U.S. Centers for Disease Control and Prevention.
That’s more than the 372 cases reported for all of 2018 — and it’s only April.
If the outbreak doesn’t get under control, this year could surpass the 2014 high of 667 cases since measles was eliminated from the United States in 2000 (SN Online: 11/30/18). Elimination means that the virus is no longer endemic, or constantly present, though it can still be brought in by overseas travelers. Internationally, outbreaks are ongoing in Ukraine, Israel, the Philippines and Brazil, among other countries.
Imported disease is the just the spark. What’s fueling measles outbreaks in the United States are pockets of vulnerability in the country, especially within states that have made it easier for parents to skip vaccinating their children. As public health officials grapple with containing the disease, here’s the lowdown on this not-so-conquered virus.
Why is measles dangerous?
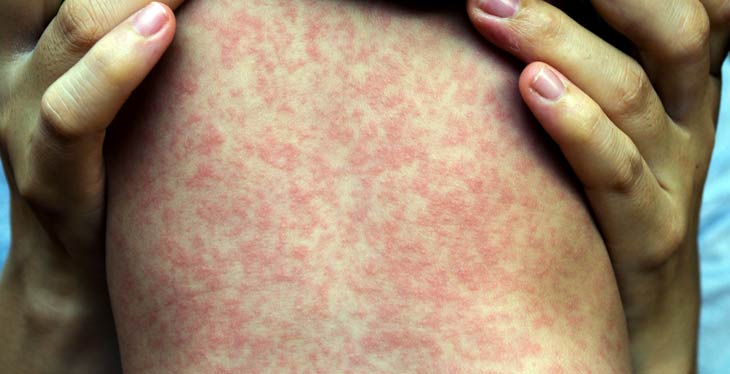
The first signs of an infection include a fever and cough, followed about four days later by a rash of flat, red spots. There’s no treatment for measles, other than managing symptoms with fever reducers, for example. Those who have been exposed to the virus but aren’t immunized can get vaccinated within 72 hours to protect against the illness.
Measles can lead to severe medical complications — particularly for babies and young children — including pneumonia or a swelling of the brain that may result in deafness. A decade before the vaccine became available in the United States in 1963, measles sickened around 3 million to 4 million people and killed hundreds each year.
“Measles is a bad actor,” says pediatrician and vaccine scientist Peter Hotez at Baylor College of Medicine in Houston.
The virus also suppresses the immune system, giving a boost to other infectious diseases. This effect persists for two to three years after a bout of measles, according to a 2015 study published in Science. So getting the measles vaccine is also an effective way of protecting against other infectious diseases, the researchers write.
Why does measles spread so easily?
A single person with measles can infect up to 18 others who haven’t been vaccinated. That makes measles more contagious than smallpox or the flu. The measles virus, which invades a person’s throat and nasal cavity, is spread through coughing and sneezing. It can also linger on surfaces or remain in the air for up to two hours, meaning one can enter a room after an infected person left and still be exposed.
The virus usually has a head start over health officials, because an infected person can begin spreading the virus before being diagnosed, which typically happens once the rash shows up. “There’s this four-day window before you got the rash where you’re infectious,” says Daniel Salmon, who heads the Institute for Vaccine Safety at Johns Hopkins Bloomberg School of Public Health.
To prevent an outbreak of measles, defined as three or more cases, a community needs to maintain herd immunity (SN: 11/11/17, p. 12). That means having enough people vaccinated that the pathogen runs out of new people to infect and transmission dies out. Because measles is so contagious, around 92 to 95 percent of a community must be vaccinated to preserve herd immunity. This protects infants, who aren’t typically vaccinated against measles until their first birthday, as well as children whose immune systems are suppressed due to cancer treatments.
Why are outbreaks happening?
The outbreaks this year — there are currently five ongoing in four states — aren’t entirely surprising. Like past outbreaks, they are hitting areas where too few people have been vaccinated to maintain herd immunity.
A few of the areas that have experienced outbreaks are in states that allow non-medical exemptions for vaccines otherwise required for children to start school. Of 18 states that have such policies, 12 have seen rising numbers of vaccine exemptions since 2009, Hotez and his colleagues reported in PLOS Medicine in 2018. “Measles tends to be a good biomarker of declines in vaccine coverage,” Hotez says.
Measles primarily hits those who aren’t vaccinated, but having pockets of low vaccination can also put those who are vaccinated at risk. Of the 1,416 measles cases reported from 2000 to 2015, more than half, or 804, were in people with no history of measles vaccination, Salmon and colleagues reported in 2016 in JAMA. And 199 cases were in people who had received the vaccine, which provides a very high, but not absolute, level of protection.
Could measles again become endemic in the United States?
The United States could lose its status as a country in which measles has been eliminated if the virus continues to circulate in an area for at least a year. In that case, measles would be considered endemic again. “That’s the big concern,” Salmon says.
To prevent that, the population as a whole has to be vaccinated at a level to establish herd immunity everywhere, health officials say.
Historically, measles season is in late winter to early spring. So “maybe as we move into the summer months, it will start to die down, but it’s unclear” what might happen, Hotez says. “We still have some big epidemics going on.”
As for whether the United States will go back to having sustained measles transmission, “I don’t know that we’re there yet,” Hotez says. “But we’re moving dangerously close to it.”