Around the world, reported measles cases jumped 31 percent in 2017
Political unrest and refusal to vaccinate is driving the disease’s surge, health experts say
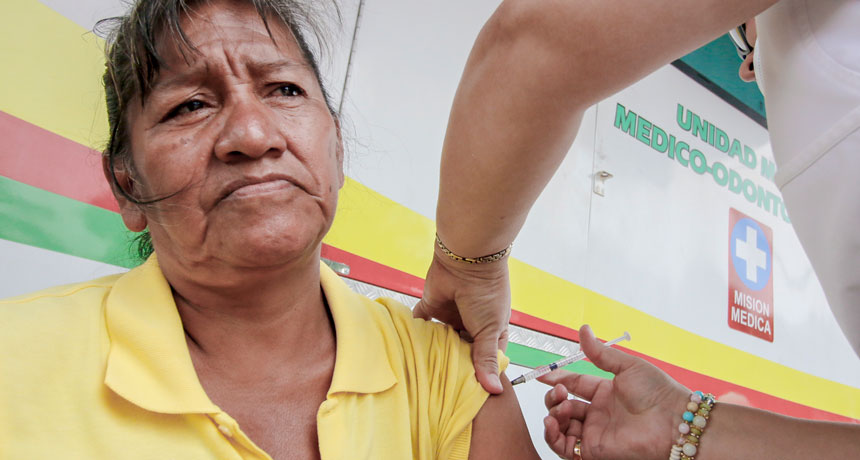
OUTBREAK MEASURES Progress toward eliminating measles has been stymied by recent outbreaks, including in Venezuela. Here, a Venezuelan woman receives a measles vaccine as she enters neighboring Colombia, part of an effort to control the spread of the disease.
SCHNEYDER MENDOZA/AFP/Getty Images