Vaccines could counter addictive opioids
Shots that harness the body's immune system may help addicts stay clean
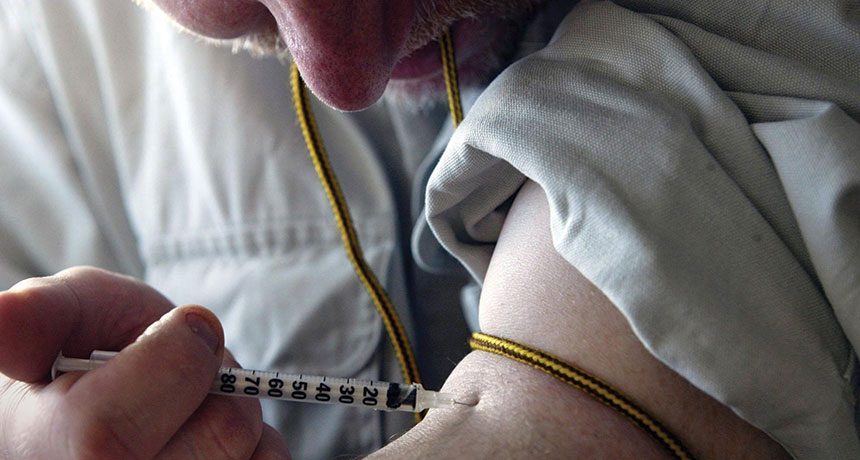
ADDICTION EPIDEMIC The power of opioid dependence sends growing numbers of people to street drugs and deadly chemical mixes.
Paul Faith/AP Images
By age 25, Patrick Schnur had cycled through a series of treatment programs, trying different medications to kick his heroin habit. But the drugs posed problems too: Vivitrol injections were painful and created intense heroin cravings as the drug wore off.