Lead’s damage can last a lifetime, or longer
Tainted water for kids in Flint could mean problems in adulthood
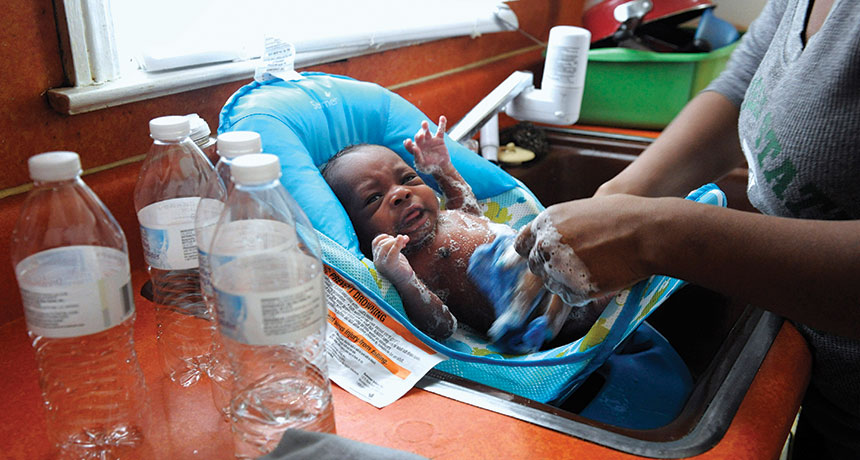
TOXIC WATER A mom in Flint, Mich., uses bottled water to bathe her three-week-old baby. Scientists have linked high levels of lead in the tap water there to elevated blood lead levels in children.
Todd McInturf/The Detroit News via AP
The people of Flint, Mich.,