A mysterious dementia that mimics Alzheimer’s gets named LATE
It’s possible about a quarter of people age 85 and older have the newly described disease

MEET “LATE” A disease now dubbed LATE causes memory trouble in elderly people, similar to what’s seen in Alzheimer’s disease, but it looks different in the brain.
Robert Kneschke/Shutterstock
A newly described dementia strikes people in their last decades of life. The disease, aptly named LATE, comes with symptoms that resemble Alzheimer’s disease, but is thought to be caused by something completely different.
An international team of scientists and clinicians describe the disease and officially christen it LATE, which stands for the more technical description, “limbic-predominant age-related TDP-43 encephalopathy,” online April 30 in Brain. Study coauthor Peter Nelson, a neuropathologist at the University of Kentucky in Lexington, helped organize a meeting last year that addressed a growing realization among doctors and scientists: “There’s this disease, and it doesn’t have a name,” he says.
Estimates vary, but it’s possible that about a quarter of people age 85 and older have LATE, Nelson says. “This is a disease that really attacks the very latest portion of the human aging spectrum,” he says.
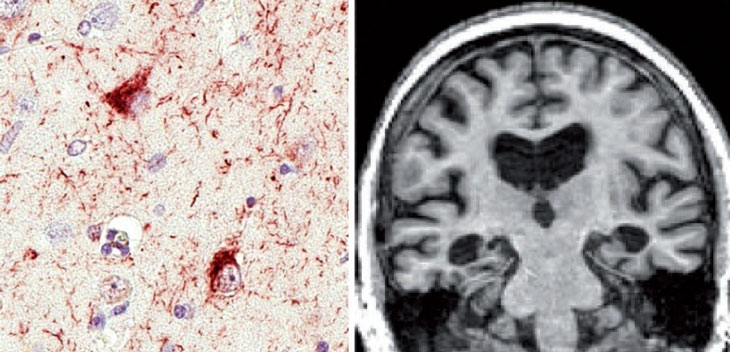
LATE comes with memory trouble and dementia — symptoms that mirror Alzheimer’s, Nelson says. But instead of the plaques and tangles that mark the brains of people with Alzheimer’s disease, LATE is characterized by a lesser-known protein called TDP-43. In LATE, that protein accumulates and spreads through parts of the brain that are key to thinking and memory, including the amygdala and hippocampus.
In Brain, Nelson and his colleagues describe the signs of LATE in the brain in a series of stages, from less severe to most severe. But the trouble is that these signs, which include the spread of TDP-43 and occasionally signs of damage to the hippocampus, can be found only after a person has died.
There are currently no surefire clinical tests that identify LATE in a living person. LATE is diagnosed largely after other disorders have been ruled out, making it a “diagnosis of exclusion,” says neurologist Michael Greicius of Stanford University, who was not involved in the study.
The researchers hope that giving the disease a name and description will make it easier to spot. Take a hypothetical 80-year-old patient with memory loss who tests negative for signs of Alzheimer’s in the brain, and whose MRI shows a smaller-than-normal hippocampus. “There, I think this notion of LATE is going to start rising quickly to the top,” Greicius says. Still, he cautions that “this is a disorder that we’re beginning to get a handle on. We’re not quite sure yet.”
Greicius also points out that brains, particularly older ones, often contain a mixture of different problems, each of which might be contributing to dementia. That makes pinning symptoms on TDP-43 a challenge. “The minute you have other pathologies in there, it’s really hard to tease those out of the picture,” he says. Many brains with LATE also show some of the signs of Alzheimer’s disease, a comingling that may confound easy diagnoses, the researchers write in the new study.
As scientists gain more tools that pinpoint various brain diseases, one thing is becoming clear, Nelson says: “It’s complicated.” There’s a growing realization that many different — and perhaps interconnected — pathways can lead to dementia. “Grappling with this complexity is necessary,” Nelson says, and could ultimately point to subsets of people who could be treated for their particular form of dementia, should a therapy become available.
That complexity may also be behind some of the recent failures of drugs to treat Alzheimer’s disease, Nelson says. People who actually had LATE — not Alzheimer’s — may have been included in those clinical trials, masking potentially positive results, he says. That’s a problem for Alzheimer’s research, but also for people with LATE, who may want to participate in trials of their own.
For now, with the new description of LATE, scientists and doctors at least have a starting point for understanding the disease, says Nina Silverberg who directs the Alzheimer’s Disease Centers Program at the National Institute on Aging in Bethesda, Md. “This is the beginning.”







