A new ketamine-based antidepressant raises hope — and questions
The anesthetic drug’s long-term effects on people aren’t clear

FAST RELIEF A new drug based on the anesthetic ketamine relieves depression in hard-to-treat cases, but its long-term consequences are unknown.
Janssen Pharmaceuticals, Inc.
With great fanfare, a new antidepressant entered the U.S. market in March, the first fundamentally new medicine for depression in decades. Based on the anesthetic ketamine, the drug — called Spravato — is intended to help people with severe depression quickly, taking effect within hours or days instead of the weeks that typical antidepressants take. But for all the hubbub, big questions have gone unanswered about the drug, developed by Janssen Pharmaceuticals, Inc.
Some psychiatrists are concerned that the drug was approved by the U.S. Food and Drug Administration based on skimpy data, under standards that were less rigorous than those required for previous antidepressants. It remains unclear, for example, what happens as someone stops taking the drug, as well as whether it has long-term effects.
The data on Spravato raise more questions than they answer, says psychiatrist Alan Schatzberg of Stanford University. “And I think that’s unfortunate.”
Despite those unknowns, some psychiatrists are relieved to have another drug to try, particularly for people with depression so severe that other drugs have failed to help. Spravato “does something that very few things in psychiatry can do — it works for people who didn’t respond to other treatments, and it works fast,” says psychiatrist Dan Iosifescu of New York University’s School of Medicine. “I really welcome having another powerful tool in my toolbox.”
Old drug, new use
Ketamine, an FDA-approved anesthetic that has been in use for decades, comprises two mirror image molecules: esketamine and arketamine. Spravato, a nasal spray, is made of just esketamine (SN: 3/30/19, p. 13). And like ketamine, which is abused in part for the floating sensation it produces, esketamine may be used illicitly. That has prompted the FDA to put tight controls over the new drug, which can cause hallucinations, sedation and dizziness.
In the weeks since the FDA’s approval of Spravato, receptionists at the clinics of Gerard Sanacora, a translational neuroscientist at Yale School of Medicine, are answering “dozens of phone calls every day” from patients and their loved ones eager for esketamine’s promise of quick relief. But “this is not a medicine for everybody,” says Sanacora, who has consulted for Janssen. Spravato, which is intended to be used with another antidepressant, was approved for use only in people who have not gotten relief from at least two other treatments. An estimated 5 million people in the United States live with this type of severe depression.
But because the drug is liable to be abused, and due to its potential side effects, Spravato can be taken only in a clinic, where patients will be monitored for several hours after their dose — “This is not a take-at-home medicine,” Sanacora says.
Those rules were set also because Spravato has largely been tested in people with severe depression, and results of its effectiveness have been mixed. So far, three one-month clinical trials have been conducted in which patients were randomly assigned to receive either the drug or a placebo, and neither patients nor doctors knew who belonged to which group. In two of the three trials, participants didn’t get any better on the drug than they did on the placebo.
In the third monthlong trial, which included 224 people, participants had their depression symptoms improve after a four-week stint of taking Spravato twice a week. That improvement held up to standard statistical analyses, but it wasn’t huge. The researchers measured depression symptoms on a 60-point scale, with lower numbers being better. Over the month of the study, people who took the placebo dropped by 15.8 points on average; people who took esketamine dropped an average of 19.8 points, beating the placebo group by four points on the 60-point scale.
In the past, the FDA had required that at least two short-term studies show that a drug was effective. With Spravato, those requirements were loosened, says Erick Turner, a psychiatrist at Oregon Health and Science University in Portland.
This time, the extra evidence for the drug’s approval came from a longer-term study that kept half of its participants on esketamine, and switched half to a placebo. That clinical trial, however, included some of the same people who responded positively to esketamine in the shorter trials. “It’s cherry-picking” the study sample, says Turner, who is a member of an FDA advisory committee on new psychiatric drugs. He did not participate in Spravato’s approval.
Unanswered questions
That longer-term study, which spanned more than a year, found that 39 of 86 people, or 45 percent, who had been switched to a placebo after taking esketamine for four months relapsed on their depression scores. In contrast, 24 of 90 people, or 27 percent, relapsed while they continued to receive esketamine. Those relapses in people who switched from ketamine to a placebo are concerning, Schatzberg says. “Doesn’t that say something about coming off the drug? What are we going to do in practice, just keep people on the drug forever?”
Some participants in the longer-term study were switched to a placebo spray after 16 weeks of esketamine. “It is not expected that patients in real-world clinical practice would have their medication stopped abruptly,” Janssen says in a March 20 statement to Science News. “Most patients with TRD [treatment-resistant depression] will require maintenance treatment.”
Three of the patients who had received esketamine in the trials died by suicide four, 12 and 20 days after the patients’ last doses of the drug. According to an FDA document, given the small numbers of people studied, their severe illnesses and the lack of similarities in these three deaths, “it is difficult to consider these deaths as drug-related.”
Janssen’s statement also notes that the suicides took place during a part of the clinical trials that did not include a comparison group of people who didn’t receive esketamine. The company says, in line with the FDA statement, that most of the suicide events were determined to have been caused by the severe depression — not the drug.
Schatzberg disagrees with those arguments, saying that stopping the drug may very well have had something to do with the suicides. “Are you inducing some sort of dependence? And when you get the people off, they feel lousy and could become suicidal?” he asks. “That, to me, is a worry.”
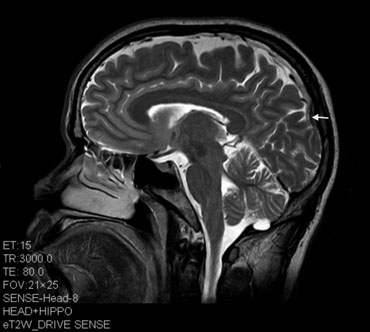
The data that do exist are concerning.
MRI scans of people who have abused ketamine for a long time reveal brain damage (though other factors could be sources of that damage). And studies on animals show ketamine-induced brain damage, too. But not much is known about esketamine’s long-term effects in people taking it for severe depression. “If you take ketamine for too long — and it’s unclear what too long is — that’s going to be a problem,” Iosifescu says. “Nobody can really tell you where this boundary is.”
Moving ahead
As more is learned about how ketamine and esketamine alleviate depression, scientists may come up with other drugs that are perhaps less problematic. Carlos Zarate, Jr., a clinical neuroscientist at the National Institute of Mental Health in Bethesda, Md., helped make some of the early discoveries about ketamine’s fast antidepressant effects. These days, he is studying a molecule that’s made when ketamine gets broken down in the body. Tests in animals hint that this molecule has rapid antidepressant properties without ketamine’s baggage.
But Zarate is circumspect. “We still aren’t really sure what the key targets are in depression,” he says. Ketamine and esketamine, many scientists suspect, work by spurring brain cells to release a chemical messenger called glutamate, which might spur nerve cell connections to form. But a small study by Schatzberg and colleagues suggested that ketamine’s antidepressant effects somehow work through the body’s opioid system — a contested idea, but one that would have big implications for addiction to ketamine.
For now, clinicians and patients are moving forward without all of the answers. Ultimately, “it’s not about being a fan of ketamine or a hater of ketamine,” Iosifescu says. “It’s about understanding what is it good for.”







