Old Drug, New Uses?
Anemia drug also protects against nerve damage
Reduce, reuse, recycle. Most people are better at recycling their trash than at either reducing or reusing it. But the idea of turning old products to new uses has a long history–and drug companies are now benefiting from the approach. Testing the safety of drugs in people takes years and can cost millions of dollars. However, research often suggests novel uses for drugs that have been on the market for years.
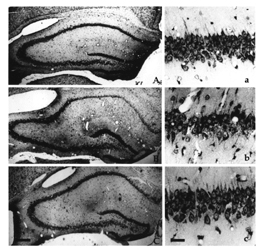

One of the most recent additions to the list of old drugs with new possible uses is a hormone called erythropoietin, or EPO. It’s been used for about a decade to treat anemia in people and, less openly, to boost endurance in athletes. Now, laboratory studies and preliminary trials in people indicate that EPO may be useful in treating nerve damage caused by stroke and spinal cord injuries.
The drug speeds formation of iron- and oxygen-carrying red blood cells. The body naturally increases its production of EPO to compensate for a shortage of oxygen, whether from high altitudes, breathing problems during sleep, or lung disease. Doctors use EPO to treat people suffering from anemia, a condition in which patients have fewer red blood cells than normal. Athletes use EPO because extra red blood cells can carry additional oxygen to hard-working muscles during exercise.
The hormone is made primarily in the kidneys. Just a few years ago, though, researchers found signs that EPO is also made by cells in the brain and spinal cord.
The researchers guessed that, as in the rest of the body, EPO might help protect nerve cells against a lack of oxygen. Of all the tissues in the body, active brain tissue uses the most oxygen.
Indeed, research shows a beneficial effect of added EPO on nerve cells. It doesn’t, however, act primarily to increase red blood cells around them. The hormone seems to prevent healthy nerve cells from dying in response to signals sent by damaged nerve cells. That’s important because in both stroke and spinal cord injury, signals from acutely injured nerves send other nerves into death spasms. This effect accounts for most of the ultimate damage from those traumas.
Scientists are still trying to tease out the variety of pathways through which EPO protects nerves. Even without that information, the researchers are excited about using the drug to treat often-crippling neurological ailments.
“There’s a great need for drugs that can protect against nerve damage,” says Anthony Cerami of the Kenneth S. Warren Laboratories in Tarrytown, N.Y. “Most neuroprotective drugs fail because of side effects. We already know EPO is safe and well tolerated in people. I think the life that it will have as a tissue-protecting factor is at least as extensive as the life it has had as a treatment for anemia.”
Head to the brain
Interest in new applications for EPO took some time to gain momentum. In the early 1990s, a team of Japanese scientists unexpectedly identified EPO-producing brain cells called astrocytes. At first, says lead researcher Ryuzo Sasaki of Kyoto University, “I was quite doubtful that EPO had a physiological function in the brain.” But he says that further studies by other teams showed that brain cells have docking spots for EPO, suggesting that the compound must play some natural role.
Sasaki and his colleagues hypothesized that the hormone might affect how brain cells respond to insufficient oxygen. In many strokes, an oxygen deficiency–such as that caused by a clot cutting off blood flow–typically causes some nerve cells to die. Over the next few hours, nearby cells die in response to distress signals that had been sent from the oxygen-deprived cells.
The researchers showed that injecting EPO into gerbil brains protected cells from dying after an animal’s blood flow to the brain was temporarily blocked. Further, agents that soak up naturally produced EPO made cells in the gerbils’ brains dramatically more sensitive to low oxygen concentrations. That finding implies that EPO normally plays an important role in minimizing nerve damage, he says.
Sasaki’s team injected EPO directly into the brain because few hormones or other large molecules can cross the blood-brain barrier, a tight network of cells along blood vessels that limits which molecules cross from the blood into the brain and spinal cord. However, Cerami and his colleagues, who were studying other actions of EPO, wondered whether the hormone might be among the molecules that the body specifically pumps across the blood-brain barrier. They had found that when healthy animals had the drug injected into their abdomens, they learned new tasks faster and remembered old tasks better than did animals that didn’t get EPO.
Cerami reports that high doses of EPO injected into the rats’ bloodstream guards the animals against brain damage caused by temporarily obstructing the blood vessels in the brain. “We can protect against about 90 percent of the cell damage in the brain” by administering EPO before or up to 3 hours after inducing strokes in the rats, Cerami says. The hormone also seems to reduce inflammation near the injury, which can further damage nerve cells.
When it was given up to 6 hours after the rats suffered strokes, EPO protected nerve cells from the secondary cell damage, albeit not as well, Cerami says. That long period of effectiveness is appealing because many people who have suffered strokes take several hours to arrive at hospital emergency rooms. Thus, they’re not eligible to get the only drug currently on the market that can reduce brain damage from stroke.
This clot-busting drug, called tPA, must be given within 2 to 3 hours of a stroke’s onset.
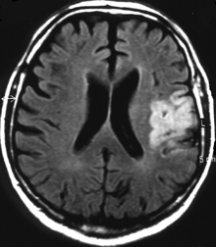
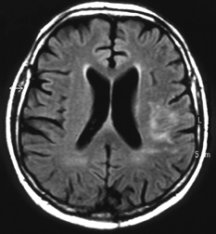
In a small pilot study of people with stroke in Germany, 20 patients treated with EPO within 7 hours of stroke later had fewer physical, speech, and memory problems and needed less day-to-day assistance than did 20 who didn’t get the hormone. People treated with EPO also tended to have smaller areas of damaged brain tissue, as measured by brain scans a month after their stroke.
People who have had the most-severe strokes seem to benefit most from treatment with EPO, reports Hannelore Ehrenreich of the Max-Planck Institute for Experimental Medicine in Göttingen, Germany. She and her colleagues published their findings in the August Molecular Medicine. The German team is now developing a trial of about 500 patients at several medical centers.
“I think this is a stunning result,” says J. Donald Easton of Rhode Island Hospital/Brown University School of Medicine in Providence. “There are fates worse than death, and the disabling consequences of stroke may be one of them.”
At least at this early stage in the evaluation, the benefits from EPO for stroke appear to be at least equivalent to that of tPA, Easton says. However, unlike tPA, which poses life-threatening risks of hemorrhage and thus can only be given in hospitals, EPO may be safe enough for potential stroke patients to get the drug on their way to the hospital, he adds. Since the two drugs work in different ways, physicians might also combine them.
Moving on
Though less common than stroke, spinal cord injuries can be devastating–the 11,000 people who get these injuries each year in the United States tend to be decades younger than stroke patients and are typically severely disabled for the rest of their lives. In most cases, people with spinal cord injuries lose control of whatever muscles are linked to nerves coming off the spinal cord below the damaged point. There are no widely effective therapies to repair spinal-nerve damage, though very high doses of steroids have helped limit it in some patients.
Cerami and his colleagues looked first at an infrequent type of spinal cord injury, one that’s similar to stroke. If blood flow to the spinal cord is blocked–say, during abdominal surgery–paralysis may result. In the Feb. 19 Proceedings of the National Academy of Sciences, the scientists described an experiment in which rabbits received an injection immediately after surgery that blocked blood flow to the spinal cord. Animals given EPO had better muscle control of their hind limbs than did rabbits getting saline instead of the hormone. Over the next 2 days, muscle function worsened in the saline-treated animals, but the EPO-treated rabbits improved. At the end of that time, they also showed less nerve damage than did those that got injections of saline.
In the July 9 Proceedings of the National Academy of Sciences, the researchers demonstrated that EPO counteracts the nerve damage associated with two more common kinds of traumatic spinal cord injury in people. In rats with spines damaged by compression of the nerves, a single dose of EPO after injury boosted the animals’ hind leg movements within 12 hours of the injury compared with those of rats getting placebo injections. After 28 days, the EPO-treated rats–some of which were given additional doses on the second and third days after injury–had near-normal movement of their hind limbs, Cerami says, while animals given the dummy injections were still paralyzed.
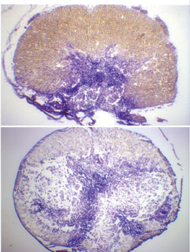
The researchers also examined direct trauma to rats’ vertebrae and spinal cord that caused injuries and paralysis more severe than those resulting from compression. The researchers didn’t see any recovery of muscle movement or limb function in this group at first, whether or not the animals were given EPO. However, between the 4th and 12th day after injury, animals treated with one dose of EPO an hour after injury had better muscle tone and more coordinated leg movements and were also better at swimming than rats treated with a placebo were. When the researchers examined the rat spines 28 days later, the rats given EPO showed fewer signs of swelling and cell death surrounding the injury than placebo-treated rats did.
“I haven’t seen anything [else] that has yielded effects this strong,” says Steven A. Goldman of the Weill Medical College of Cornell University in New York City. Finding a benefit from EPO in a variety of spinal cord injuries is “very encouraging” and suggests the hormone could produce similar results in people, he adds.
Nonetheless, Goldman cautions, “even where things work wonderfully in animal models, it’s not uncommon to fail in human trials.”
“You can always be fooled, so it’s important that other groups replicate these results,” says Ron Cohen, president of Acorda Therapeutics in Hawthorne, N.Y. That said, the magnitude of the effect of EPO on rats’ spinal cord injuries is impressive, he remarks. People with spinal cord injuries would benefit from even slight lessening of their nerve damage. “If you could just give them a little function, in many cases that could be the difference between sitting in a wheelchair and being able to feed yourself versus being in bed and dependent on others,” Cohen says.
Applications abound
Even as researchers are examining basic questions about how the hormone crosses the blood-brain barrier and exploring the multiple actions through which it might exert its beneficial effects, they’re already pursuing EPO’s potential for treating several additional diseases.
Researchers are concerned about potential problems with using the drug to treat chronic diseases. One recent study has suggested that in rare instances the genetically engineered EPO may cause a person’s body to stop producing red blood cells at all, perhaps by causing the immune system to attack both the genetically engineered and normal EPO. In people without underlying anemia, long-term therapy with EPO could conceivably increase the number of red blood cells and thus trigger blood clots.
However, most doctors say this side effect can be easily monitored and treated by simply removing blood from a patient with too many red blood cells.
Researchers are already looking into whether EPO might offer benefits to people with multiple sclerosis, glaucoma, and heart disease. Cerami and Pietro Ghezzi of the Mario Negri Institute of Pharmacological Research in Milan report in the Oct. 11 issue of Brain Research that giving EPO to rats with experimentally induced multiple sclerosis reduces symptoms of the disease.
In the Aug. 6 Proceedings of the National Academy of Sciences, a team of researchers including Cerami reports that EPO may protect against the damage caused by glaucoma–a leading cause of blindness. In glaucoma, high inner-eye pressure blocks blood flow to the optic area and damages cells important to vision.
Cerami says he also has unpublished data suggesting that EPO improves outcomes in animal models of heart attacks, which cause widespread cell death and inflammation.
The hormone may also have applications in infant care. When babies don’t get enough oxygen during birth, some die and many have lifelong neurological problems. Sandra E. Juul of the University of Washington in Seattle is beginning studies to see whether EPO can benefit these babies.
These projects all contribute to a groundswell of scientific interest in studying EPO’s mechanisms and effects. Says Juul, “This is not a silver bullet, but it may be better than what we have, because we don’t have anything. I’m very excited about the possibilities.”
****************
If you have a comment on this article that you would like considered for publication in Science News, please send it to editors@sciencenews.org.
To subscribe to Science News (print), go to https://www.kable.com/pub/scnw/subServices.asp.
To sign up for the free weekly e-LETTER from Science News, go to http://www.sciencenews.org/subscribe_form.asp.







