What we know about the Ebola outbreak, and the vaccine that might help
The first reported case in a big city has health officials worried
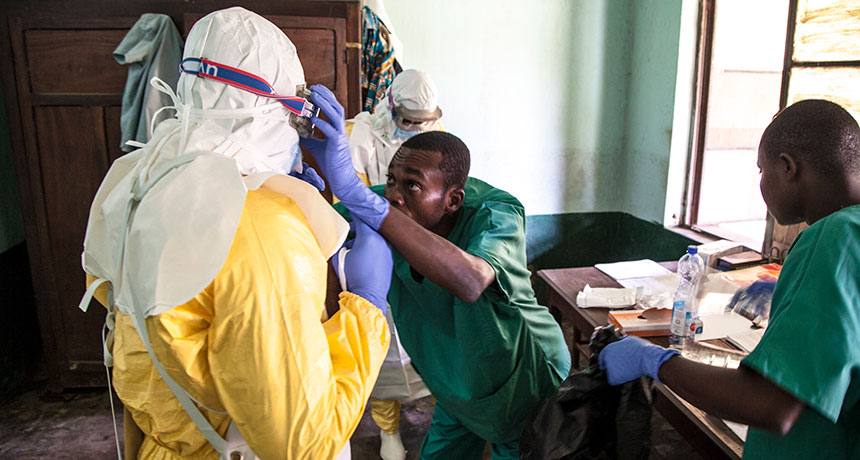
SUIT UP Congo is battling its ninth outbreak of Ebola virus. Here health workers prepare to care for possible Ebola patients at Bikoro Hospital in the center of the outbreak.
Mark Naftalin/UNICEF