Lack of sleep is tied to increases in two Alzheimer’s proteins
It’s not just A-beta levels that rise in the sleep deprived; tau levels do too
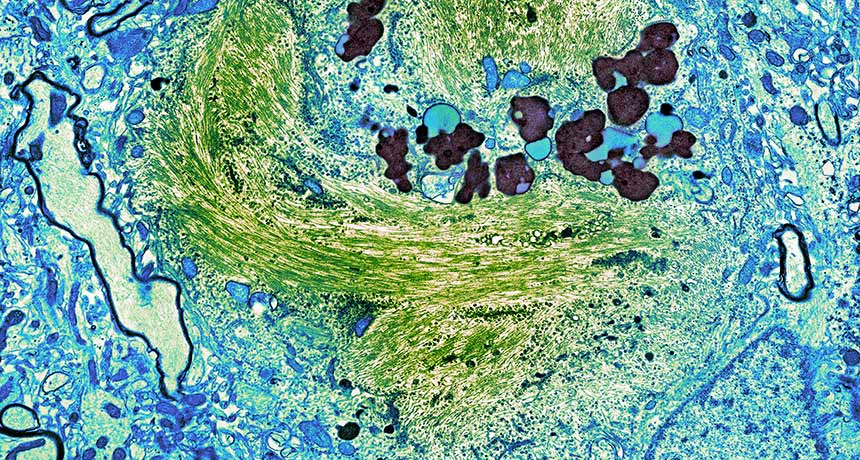
TANGLED UP Tangles of tau protein (green) muck up a nerve cell from a patient with Alzheimer’s disease, as seen in this transmission electron micrograph.
Thomas Deerinck, NCMIR/Science Source
A sleep-deprived brain is awash in excess amounts of not one but two proteins whose bad behavior is implicated in Alzheimer’s disease.
A new study finds excessive amounts of a protein called tau in the fluid that bathes the brain and spinal cord of extremely sleep-deprived adults. Tau, which is tied to nerve cell death, tangles and spreads throughout the brain during Alzheimer’s. An earlier report on these sleepy adults found that the protein amyloid-beta — globs of which dot the brains of Alzheimer’s patients — also increased.
Samples of cerebrospinal fluid collected from eight adults, monitored during a night of normal sleep and over the course of 36 hours of sleep deprivation, revealed a 51.5 percent increase in tau in participants robbed of shut-eye. And sleep-deprived mice had twice the amount of tau as well-rested mice, researchers report online January 24 in Science. Earlier work by these researchers had suggested that the quality of sleep might affect tau levels; this time, it’s been linked to duration of sleep.
With both A-beta and tau increasing with a lack of sleep, “it certainly argues that treating sleep disorders during mid-life as well as getting appropriate levels of sleep is likely to decrease risk for Alzheimer’s disease,” says coauthor David Holtzman, a neurologist and neuroscientist at Washington University School of Medicine in St. Louis. During sleep, the brain appears to flush out excess proteins and other debris (SN: 7/21/18, p. 22), so perhaps less sleep means that wash cycle is curtailed.
An estimated 5.7 million people in the United States have Alzheimer’s disease, according to the Alzheimer’s Association. A type of dementia, Alzheimer’s leads to problems with thinking, memory and behavior that eventually interfere with one’s ability to function day-to-day. Plaques of A-beta and twisted bits of tau litter the brains of those with the disease, producing damage that leads to Alzheimer’s symptoms.
In 2017, Holtzman and colleagues had reported that a night of poor-quality sleep raised levels of A-beta in the cerebrospinal fluid, and if that night had been preceded by a week of less-than-sound snoozing, the amount of tau also increased (SN Online: 7/10/17). In that study, volunteers were monitored on a night of sound sleep and a night in which they got the same amount, but their deep sleep was disrupted.
Evidence suggests that when brain nerve cells are highly active — that is, busily firing away electrical messages to other neurons — they release more tau. Since being awake appears to result in more nerve cell activity, Holtzman says, “we wondered whether the release of tau from nerve cells might also be accelerated during wakefulness versus during sleep.” In fact, when mice were awake, tau levels were 90 percent higher in the fluid between neurons than when the animals were slumbering, the researchers found.
And sleep deprivation seems to impact tau more than A-beta. In the samples of cerebrospinal fluid from the sleep-starved adults, the increase in tau surpassed the 30 percent increase in A-beta. The excessive amounts of these two proteins in the fluid may set the stage for later problems. The more A-beta released from cells, the more likely it is to clump up and accumulate over time, Holtzman says, while chronic increases of tau — driven by sleep deprivation or other means — may push the spread of its tangled, destructive form throughout the brain.
The findings show that just as the sleep-wake cycle regulates the release of A-beta from neurons, it also affects the amount of tau those cells release, says Bess Frost, a tau biologist at the University of Texas Health San Antonio, who was not involved in the study. “The two main pathological hallmarks of Alzheimer’s disease are both affected by sleep.”
Frost says that the effect of the sleep-wake cycle on tau is also important to know for other neurodegenerative diseases that feature tau tangles, such as chronic traumatic encephalopathy, or CTE (SN: 8/19/17, p. 15).