No-pain gene discovered
Genetic culprit for inability to perceive pain could lead to new treatments for chronic pain
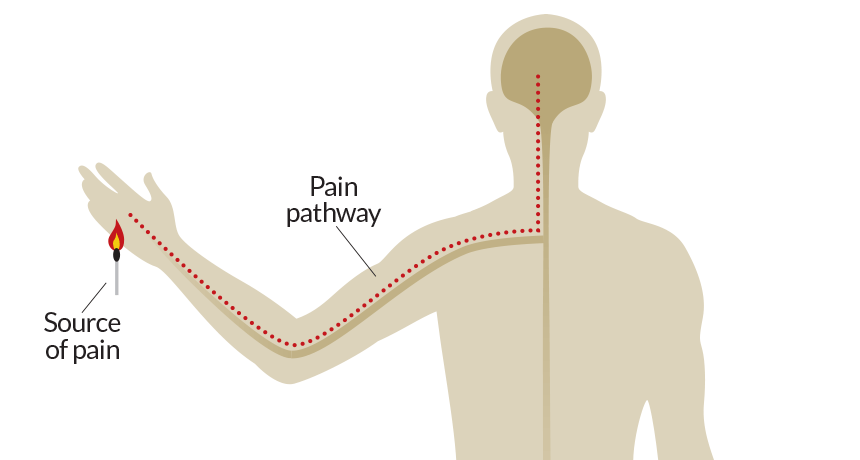
HOW IT HURTS Rare mutations in the gene PRDM12 prevent proper development of pain-sensing fibers that carry pain signals from the skin to the brain, rendering people impervious to pain, a new study suggests.
E. Otwell