To treat the heart, start with the gut
Potential drug targeting intestinal bacteria stops chain reaction that leads to artery plaque
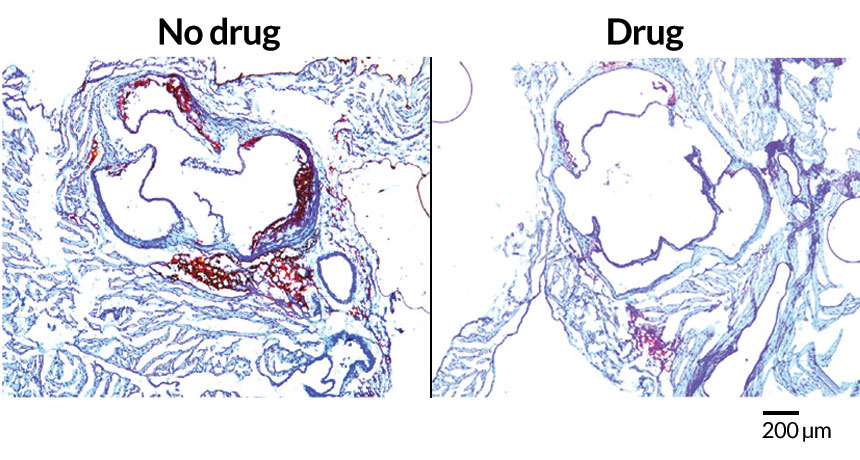
GUT CHECK Mice predisposed to heart disease and fed a diet high in choline — a compound found in meat and eggs — had plaque buildup in their arteries (left: plaques, red; artery, blue). Mice also given a drug to prevent their gut microbes from breaking down the choline had much less artery clogging (right).
Z. Wang et al/Cell 2015