When tickling the brain to stimulate memory, location matters
Zapping white, not gray, matter improves memory test results, new research suggests
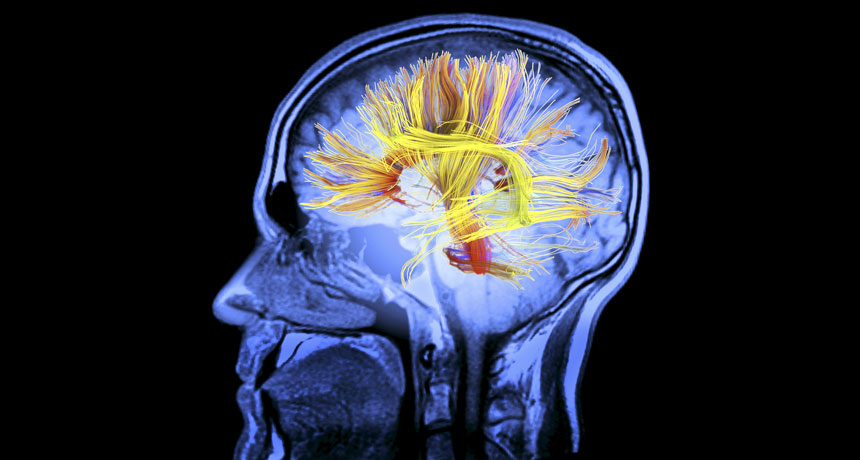
WHITE MAGIC Targeting parts of the brain's white matter, the tissue that connects different brain regions (shown), may be key to whether stimulating the brain with electricity will work as a treatment for memory problems and other ills.
Pasieka/Science Source






