Antimicrobial resistance is a leading cause of death globally
In 2019, 1.27 million deaths were due to treatment-resistant infections
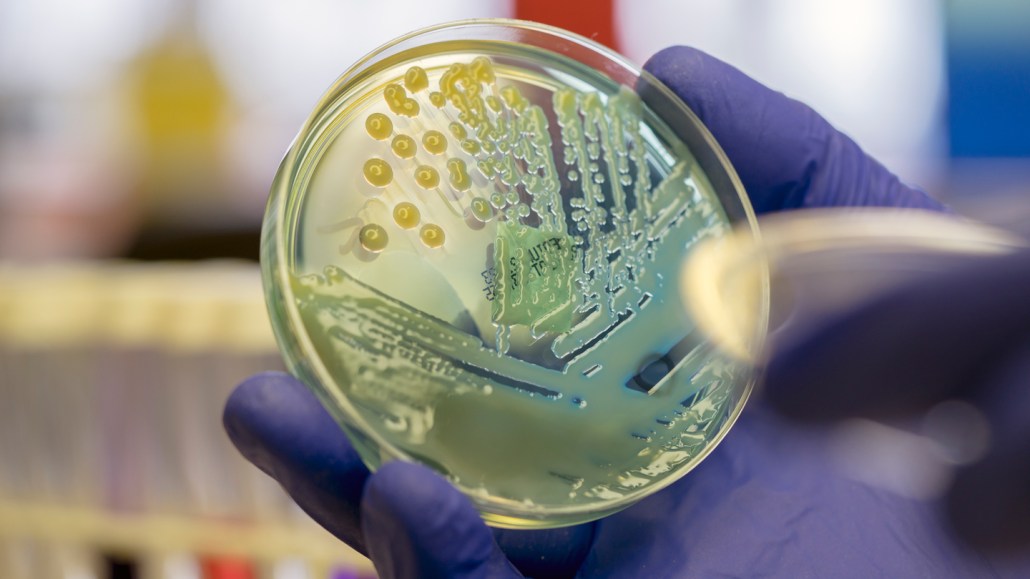
Escherichia coli, Klebsiella pneumoniae (shown here in a culture dish) and Staphylococcus aureus were the top three among the bacteria responsible for fatal drug-resistant infections worldwide in 2019.
Rodolfo Parulan Jr./Moment/Getty Images







