Bad News, Good News: ADHD-risk gene has silver lining
A gene variant that increases the risk for attention-deficit hyperactivity disorder also appears to help children grow out of the worst of their behavioral problems as certain brain structures normalize, new research suggests.
“It looks like a double-edged sword,” Philip Shaw says of the gene variant. Shaw led the work at the National Institute of Mental Health in Bethesda, Md.
Previous research found that children with a particular version of the DRD4 gene had an additional 15 to 45 percent risk of being diagnosed with ADHD. It’s the strongest known heritable risk factor for the disorder, which affects an estimated 3 to 6 percent of school-age children in the United States.
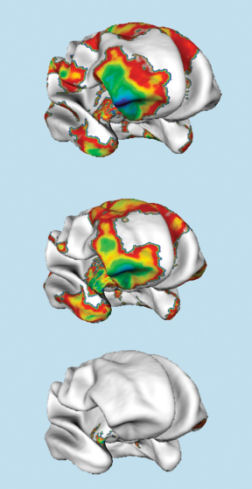
Last year, Shaw and colleagues reported that certain brain regions in children carrying this gene variant were unusually thin. That finding buttressed theories suggesting that those regions, on the right side of the brain’s outer layer, or cortex, serve as attention centers.
Shaw’s team now finds that in those same children the affected brain regions normalize in thickness during adolescence. At age 8, children carrying the gene variant had a much thinner-than-normal cortex in the key areas, but by age 16 those differences had all but disappeared.
At the same time, behavioral symptoms such as poor concentration and weak impulse control improved more in ADHD children with the gene variant than in ADHD children who carried other versions of the gene. After 6 years in the study, 79 percent of children with the gene variant had shed the diagnosis, compared with only 49 percent of the other children.
Shaw and his colleagues looked at brain scans and DNA from 105 children with ADHD and from 103 children without the disorder, they report in the August Archives of General Psychiatry. Overall, 45 percent of the children with ADHD had the gene variant in question, and 34 percent of non-ADHD children had it.
The new research builds on prior evidence that youngsters with ADHD, who lack concentration, self-control, and organizational skills, possess smaller brain volumes than psychiatrically healthy children do (SN: 10/12/02, p. 227). The findings also bolster the case that the brain’s dopamine system is impaired in ADHD, says Shaw. Dopamine is a key nerve-signaling molecule. The DRD4 gene encodes a dopamine receptor, a lock-like molecule that triggers nerve activity when dopamine fits into it like a key. Methylphenidate (Ritalin) and other drugs prescribed for ADHD change how the brain responds to dopamine.
In addition, the new research supports the idea that there are at least two subtypes of ADHD, says James Swanson of the University of California, Irvine. His research shows that children carrying the DRD4 variant don’t have the cognitive impairment shown by some children with ADHD.
“I think there is a personality characteristic that leads to the diagnosis of ADHD related to the DRD4 gene,” he says. “Then you have another group that’s ADHD because they have some sort of minimal brain damage” that’s probably not in the part of the brain affected by the gene variant.