A Gasping Heart
Cardiac quirk may worsen sleep apnea, invite altitude sickness
A common imperfection in the structure of the heart may worsen breathing difficulties in people who have sleep apnea and provoke a life-threatening condition called high-altitude pulmonary edema in mountaineers who ascend too quickly. In both scenarios, new studies suggest, the cardiac abnormality contributes to a rapid drop in the blood’s oxygen content.
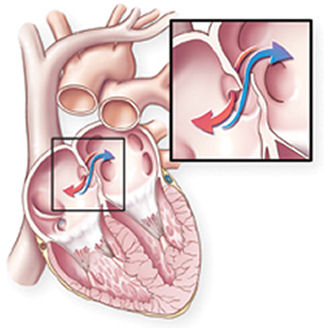

In newborn babies, the wall of tissue that separates the left and right sides of the heart has a small opening called the foramen ovale. Usually, flaps of tissue that surround the hole fuse soon after birth, sealing the opening. In about a quarter of people, however, the flaps remain unsecured—and the opening stays “patent”—into adulthood.
A patent foramen ovale (PFO) generally causes no problem unless the flaps of tissue part and a gap forms between them. That can happen if pressure in the heart’s upper-right chamber temporarily becomes too great. Past studies have linked PFO to increased risks of stroke, migraine, and decompression illness, an injury that occurs in scuba divers.
When a gap opens, deoxygenated blood from the heart’s right side can mix with oxygenated blood on the left, attenuating the latter’s oxygen content.
Sleep struggle
The abnormality can be a problem for people who experience obstructive sleep apnea, says Magnus C. Johansson, a clinical physiologist at Sahlgrenska University Hospital/Östra in Gothenburg, Sweden. Apnea affects up to one in five adults.
An episode of apnea occurs when a person’s upper airways collapse during sleep and breathing ceases for 10 seconds or more. As such a person unconsciously strains to inhale, pressure changes in and around the heart can force open a PFO, Johansson says.
In certain people, bouts of apnea cause oxygen desaturation, which is an unusually large and rapid drop in blood-oxygen concentration. Desaturation appears to be a factor in the high rates of cardiovascular disease associated with apnea, Johansson says.
To see whether PFOs might contribute to oxygen desaturation, Johansson and his colleagues monitored blood-oxygen concentrations throughout the night in people who had apnea. The researchers identified 15 volunteers who frequently experienced oxygen desaturation and another 15 who experienced it rarely. The scientists then directed sound waves at the heart to assess blood-flow patterns in the 30 participants. Those tests revealed PFOs and quantified how much blood, if any, shunted between chambers.
The abnormality was present in nine members of the frequent-desaturation group but only two members of the other group, Johansson and his colleagues report in the January European Respiratory Journal.
Using a minimally invasive procedure, cardiologists can seal a PFO to prevent recurrent decompression illness or stroke. Some researchers are also studying PFO closure as a possible treatment for migraines (SN: 2/19/05, p. 119: Against the Migraine). Closure in people who have sleep apnea might mitigate the problem of oxygen desaturation, too, Johansson suggests.
Franco Ferrillo, a sleep specialist at the University of Genoa in Italy, agrees that closing the hole might help such patients, but he points out that it’s not the only potential treatment. He suggests that people who have apnea and a PFO are particularly likely to benefit from continuous positive airway pressure, or CPAP, a widely used mechanical treatment for apnea.
In this therapy, a patient wears a face mask while sleeping. A machine continuously forces air through the mask to prop open the sleeper’s airways. Although the treatment has proven effective against apnea, many patients don’t use it because they find it hard to sleep while wearing the air mask.
Ferrillo and his collaborators recently completed a 2-year trial of the forced-air treatment in patients who had both apnea and a PFO. They found that, in addition to lessening the severity of apnea, long-term treatment shrank the holes in patients’ hearts.
By repeatedly forcing open a PFO, untreated apnea may gradually enlarge the defect, Ferrillo suggests. That would feed a vicious cycle in which the hole worsens apnea and apnea expands the PFO.
It’s important to use CPAP to break the cycle, Ferrillo concludes. “Doctors must look for a patent foramen ovale every time they see an apnea patient with higher desaturation than expected,” he says.
Sky high, oxygen low
The 35 intrepid mountaineers in a recent medical study set out from an elevation of about 1,100 meters above sea level. Less than 24 hours later, they reached a small research station called Capanna Regina Margherita, which stands on a 4,559-m-high peak in the Italian Alps near the Swiss border.
Their rapid ascent put them in dangerous territory, as 16 of the veteran climbers knew from personal experience. Those men and women had previously experienced high-altitude pulmonary edema, a potentially life-threatening condition in which fluid collects in the lungs. Eight of them would soon experience it again.
As people climb mountains, the air they breathe gets thinner and thinner, and the blood pressure in their lungs increases to compensate for the blood’s relatively low oxygen content.
For reasons that aren’t yet understood, that response is exaggerated in some people, and a quick increase in elevation to an altitude of 2,500 m or higher can cause edema in their lungs. The fluid can block gas exchange and lead to respiratory failure.
Although medical treatments are available, the best way for a climber to reverse high-altitude pulmonary edema and prevent permanent harm is to return promptly to a lower elevation, says Yves Allemann, a cardiologist at the University Hospital’s Swiss Cardiovascular Center in Bern. “It’s only life threatening if you do not take the necessary therapeutic measures,” he says.
The researchers tested each volunteer twice to see whether he or she had a PFO and, if so, to determine the size of the opening. PFOs were more than four times as common in the volunteers who had previously experienced high-altitude pulmonary edema as in the other climbers, Allemann and his colleagues found. In the test conducted at the top of the peak, PFO was present in 69 percent of the former group and just 16 percent of the latter group.
Moreover, blood-oxygen saturation at high elevation was significantly lower in the edema-prone volunteers than in the comparison group, and it was particularly low among volunteers who had large PFOs.
Eight members of the edema-prone group—six of whom had a PFO—again developed pulmonary edema. No one in the control group developed the problem, Allemann’s team reported in the Dec. 27, 2006 Journal of the American Medical Association.
Professional mountain guides led ill volunteers down to a lower elevation. “As soon as they go down and have normal oxygen [concentrations] in the air, they heal,” says Allemann.
The findings suggest a physiological connection between having a PFO and being prone to high-altitude pulmonary edema, Allemann concludes.
Climbers who have experienced pulmonary edema might seek testing to determine whether they have a PFO, and the presence of the abnormality might discourage them from making extreme climbs, Allemann says. In the future, doctors might seal PFOs in an attempt to eliminate such climbers’ susceptibility to altitude sickness, he suggests.
There’s some precedent for that approach. Allemann’s boss, Bernhard Meier, was among the first researchers to link PFO to decompression illness. He’s now conducting a trial designed to test whether sealing divers’ PFOs can reduce their risk of recurrent illness.







