Herpes virus homes in on cancer target
A virus well known for the painful cold sores it causes is currently being tested as a treatment for patients’ malignant tumors. New findings by researchers at the University of Calgary in Alberta show how the virus, herpes simplex virus 1 (HSV-1), does selective damage to cancerous tissue. That revelation could point researchers toward ways of exploiting HSV-1 to better fight cancer.
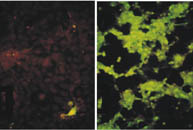
A relative of the herpes virus that causes genital rashes, HSV-1 thrives in many types of cancer cells and can kill them. Patrick W. K. Lee and his group have discovered that the virus replicates most rapidly in cancer cells with particular mutations.
Many tumors contain mutations in their genes that regulate cell growth. Mutations that make one of these, the Ras gene, hyperactive prompt cells to proliferate wildly.
In the Aug. 1 Nature Cell Biology, Lee’s group shows that HSV-1 replicates unusually quickly in cells that have a hyperactive Ras gene. The researchers also show that such cancer cells crank up HSV-1 production by speeding up the manufacture of viral proteins. Lee notes that about 80 percent of tumors have Ras-activating mutations and thus might be susceptible to HSV-1.
In a sense, [this work] is a quantum leap in the field, says virologist David A. Leib of Washington University in St. Louis. Scientists had known that HSV-1 can destroy some tumor cells, he says, but Lee’s group is finally providing a mechanism to explain those observations.
The use of HSV-1 is proving safe as a cancer treatment in clinical trials. In these current experimental treatments, researchers use viruses genetically engineered to not replicate in normal tissue. This built-in limitation is critical for patients undergoing chemotherapy whose weakened immune system leaves them vulnerable to the virus.
When scientists alter the viruses to make them safer, they also make them less effective against cancer cells. The new details about HSV-1’s ability to grow explosively in certain cancer cells increases the chance that we can make the viruses more specific and more potent for treating cancer, says Harvard neurosurgeon Robert L. Martuza.
One way to enhance the virus’ cancer-killing ability might be to apply drugs that increase the activity of Ras and thus promote viral replication, speculates Martuza, who is now conducting clinical trials using HSV-1 to treat brain tumors. He adds that researchers can already ascertain if a tumor has the kinds of defects in Ras that may make it conducive to the viral treatment.
What’s most exciting, says Lee, is that his team is promoting a general concept in cancer treatment. Two years ago, he and his coworkers showed that an unrelated virus also could elicit the death of cancer cells having an activated Ras gene. Many other viruses now under consideration for cancer treatments might work the same way, he says.
Moreover, Lee says, his work could lead to new treatments for herpes infections. His study indicates that drugs that inactivate Ras seem to block HSV-1 replication in cells growing in the laboratory.
Martuza finds this approach speculative, but certainly a possibility.
Lee says he now has preliminary evidence that such anti-Ras drugs also work in cells to fight the sexually transmitted virus, herpes simplex 2.







