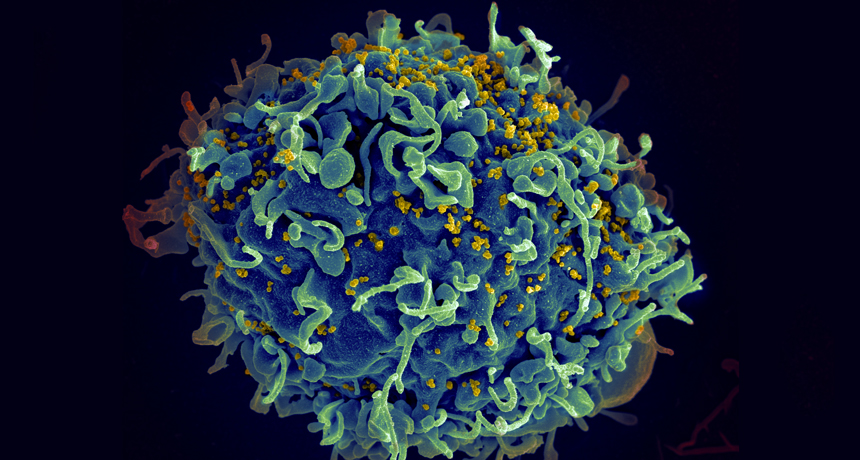
HIDEOUT HIV (yellow) infects immune cells called T cells (blue), as seen in this scanning electron micrograph. The discovery that HIV inserts itself in a host’s genes related to cell growth may help explain how the virus persists in the body for so long.
NIAID
HIV can sometimes create a self-replicating hideout that allows the virus to stay dormant in the body for a decade or more, a new study suggests.
The virus, which causes AIDS, infects immune cells called CD4+ T cells and inserts itself into host cells’ DNA. The virus can lurk in these cells for decades as a dormant, or latent, infection. When patients stop antiviral therapy, the virus can rebound. But no one knew why some T cells serve as the reservoir or how many of these viral hideouts live in the body. Also a mystery was whether the virus persists by lying dormant in long-lived cells or by continually reinfecting new ones, says Charles Bangham, an immunologist and virologist at Imperial College London.
Now, it appears that HIV’s longevity in the body depends on where the virus inserts itself. When HIV lands in a gene involved in cell growth, it can somehow spur the cell to divide, replicating the cell and the virus buried in its DNA. Such clonal expansion — the duplication of cells — can produce populations of infected cells that last for at least a decade, virologist Stephen Hughes of the National Cancer Institute in Frederick, Md., and colleagues report June 26 in Science.
The finding could mean that a cure for HIV would need to stop infected cells from dividing as well as halt the virus from replicating, says Bangham, who was not involved in the work. “It means there is even more of a problem than we have thought.”
Hughes and his colleagues examined white blood cells from five HIV-infected people who had taken antiviral drugs for different periods of time. The researchers mapped where the virus had inserted itself within the people’s DNA.
In total, the team found 2,410 different insertion places. Most locations, 57 percent, were found only once. But the remaining 1,022 sites popped up again and again in different cells, indicating that multiple cells carried identical insertions. That result suggests that the original infected cell had divided many times, giving rise to infected clones. In one person, 58 percent of the infected cells were clones of one cell.
Closer examination revealed that in many of the clones, HIV had inserted into genes that help control cell survival and growth. In one patient, the virus landed in the MKL2 gene 15 different times. About half of the originally infected cells with insertions in this gene expanded into clones. The virus also landed in the BACH2 gene at least 15 times. Mutations in both genes have been linked to cancers.
That’s concerning, says Andrew Rice, an HIV molecular virologist at Baylor College of Medicine in Houston. If the virus inserts into a gene involved in cell growth or survival it could promote cancer by fostering clonal expansion, which might lead to unchecked growth, he says. However, there is no strong evidence that that HIV directly causes cancer. Most of the cancers seen in HIV patients result from other viruses that run amok when patients’ immune systems are weakened.
This discovery that HIV can cause clonal expansion could have implications for gene therapy, says Angela Ciuffi, a virologist at the University Hospital of Lausanne and the University of Lausanne in Switzerland. Researchers have used gamma retroviruses to insert healthy copies of defective genes into children with immune disorders. Although successful, some of the children later developed leukemia because the retrovirus insertions caused mutations in cancer-related genes. Now some scientists are attempting gene therapy using lentiviruses, modified versions of HIV, to deliver genes to patients’ cells (SN: 8/10/13, p. 19). Because HIV has now been shown to stimulate cell growth when it hops into cancer-linked genes, researchers may need to be even more vigilant in monitoring gene therapy patients for cancer, Ciuffi says.
Before worrying too much about clonal expansion, scientists need to determine whether the cloned cells are the source of infectious HIV viruses. Researchers have previously discovered that many HIV insertions are defective and can’t produce infectious viruses, says Janet Siliciano, a biochemist and virologist at Johns Hopkins University School of Medicine. “If they’re defective you don’t need to worry about them” infecting other cells, she says.







