Post-stroke shifts in gut bacteria could cause additional brain injury
Mouse study suggests fecal transplants as therapy
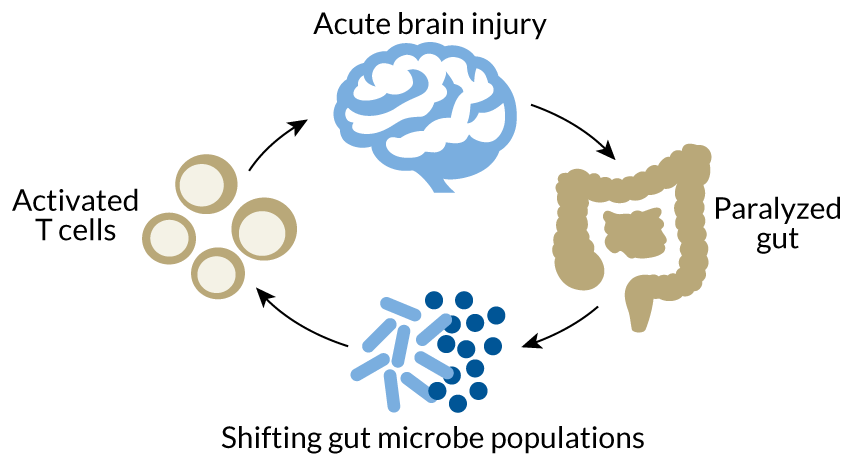
VICIOUS CYCLE After a brain injury, the guts become temporarily paralyzed. That alters gut microbe populations, triggering the activity of pro-inflammatory T cells, which cause further damage in the brain, mouse studies show.
E. Otwell






