Resistance to key malaria drug spreads
Parasites less susceptible to artemisinin now affect several Asian countries
Resistance to the top malaria drug has fanned out from its origins in Cambodia to other parts of Southeast Asia. A report in the July 31 New England Journal of Medicine establishes that the scourge has found a way to skirt the effects of artemisinin and its chemical derivatives, the best available antimalarial drugs. Scientists suspect that a genetic mutation in the parasite in these harder-to-treat cases underpins the resistance.
“I’m concerned,” says Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases, or NIAID, in Bethesda, Md. “Artemisinin derivatives used in combination with other drugs have been game changers.”
There were 207 million cases of malaria worldwide in 2012, the World Health Organization estimates, killing 627,000 people, most of them children under age 5. There is no approved vaccine against the protozoan malaria parasite, which is spread by mosquitoes and causes fever, chills, convulsions and more severe symptoms.
Artemisinin and its derivatives have been especially good at hammering Plasmodium falciparum, the protozoan that causes the most severe malaria infections. The drug is based on an ancient remedy that was rediscovered in the 1970s and developed into a pill. Along with mosquito nets, artemisinin-derived drugs used in tandem with other antimalarials have helped ease the global malaria burden in recent years. WHO recommends use of artemisinin derivatives only in combination with other drugs, to limit the survival of parasites that could develop resistance.
But the history of malaria treatment is peppered with drugs to which the parasite has become resistant, and artemisinin might be next. A decade ago, Cambodia emerged as the epicenter for artemisinin-resistant malaria (SN: 11/22/08, p. 9). Hints that resistance there had spread to neighboring countries showed up five years ago (SN: 12/19/09, p. 15). In the new study, researchers provide hard evidence of this proliferation, finding that many patients in Thailand, Vietnam, Laos and Myanmar are now taking longer to clear the parasite from their bodies after artemisinin treatment. Delayed clearance means parasites are surviving the drug’s effects longer – that the drug is losing its punch.
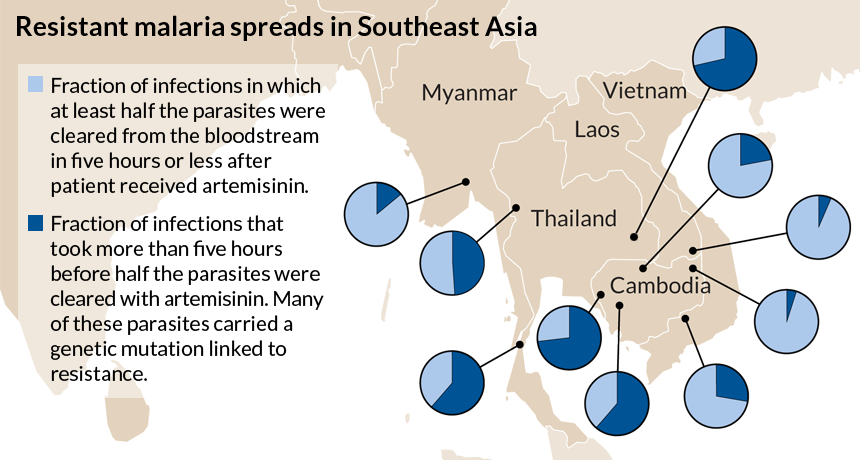
Scientists consider a case resistant to artemisinin if half of the malaria parasites are still alive in the blood more than 5 hours into treatment. Depending on location, the patients in these countries took a median time of 6.9 to 9.6 hours after the first artemisinin dose to halve their parasite load.
The study also solidifies a link, found in earlier research, between delayed parasite clearance and mutations in a P. falciparum gene called kelch13. The presence of these mutations might aid in tracking drug resistance, says study coauthor Nicholas White, a tropical medicine physician at Mahidol University in Bangkok. How the mutation helps the parasite remains unknown, he says.
There is no way of predicting whether this signals the beginning of the end for artemisinin as a frontline drug. “The efficacy of artemisinin is definitely taking a hit right now in Southeast Asia,” says study coauthor Rick Fairhurst, a physician and malaria researcher at NIAID. He expects more malaria parasites across the region to acquire mutations in kelch13.
Patients with parasites resistant to artemisinin will need longer treatment, many will fail on current drug combinations and more may die, White says. But for now, a six-day treatment — rather than the standard three — of artemisinin plus another antimalarial seems able to clear resistant infections, the study shows.
Fauci calls that solution temporary. He notes that six days of pills cost more than three and requires more diligence, increasing the risk that patients won’t take full prescriptions. “If you start feeling better and have 75 percent of your parasites cleared and your fever is gone, you may get to day four and say, ‘I’ve had enough,’ ” he says. Such partial treatment contributes to resistance.
Meanwhile, the malaria drugs used in tandem with artemisinin “are also in trouble,” Fairhurst says. Parasites that survive the rapid artemisinin onslaught might buy themselves time to mutate and become resistant to the partner drug. “That’s evolution for you,” he says.
Editor’s Note: This article was updated August 12, 2014 to correct the number of patients in Southeast Asia who participated in the study.







