Is taking birth control as a teen linked to depression? It’s complicated
It’s hard to study hormones and the teen brain
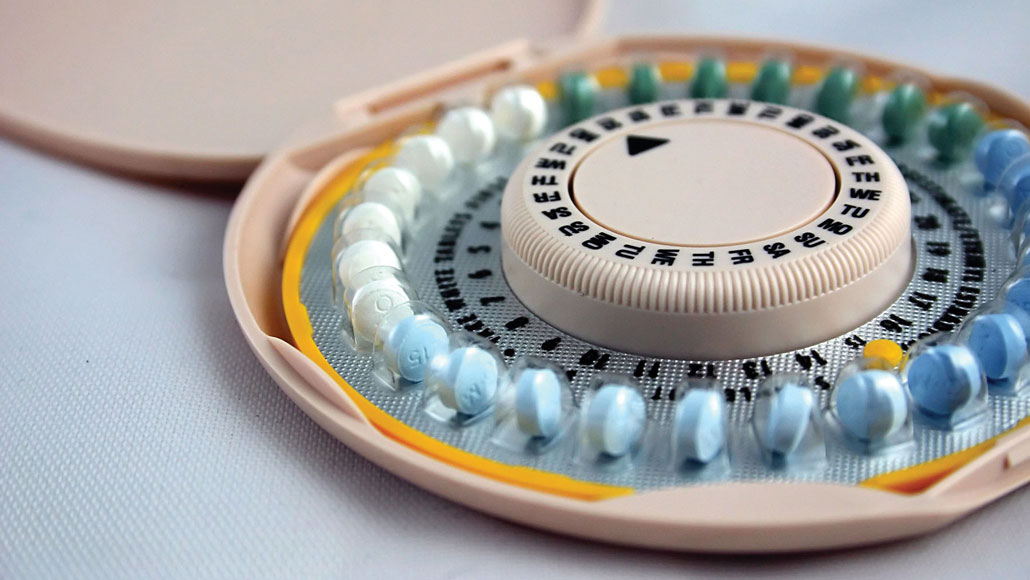
Hormonal birth control pills give women control over their lives. But whether the pill has any effect on teenage brains is not settled.
crankyT/iStock/Getty Images Plus