Teen hearing loss rate worsens
Percentage of adolescents with some decline has increased since 1990s, study shows
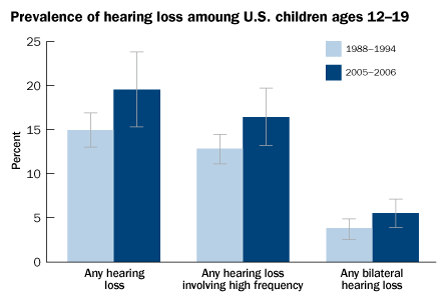
The prevalence of hearing loss in teenagers rose by nearly one-third in recent years compared with the rate in the 1980s and 1990s, a new study shows. The findings come as a surprise to the study’s authors, who had expected overall hearing to improve thanks to publicity about the risks of exposure to loud music and the advent of childhood vaccines against meningitis and pneumonia that can prevent many ear infections.
But in the August 18 Journal of the American Medical Association, the scientists report that the portion of U.S. adolescents aged 12 to 19 with any hearing loss rose from 14.9 percent during the 1988 to 1995 period to 19.5 percent in 2005 and 2006.
Researchers based the analysis on information gathered from nearly 3,000 kids in the earlier time frame and more than 1,700 in the later sampling. The findings suggest that as many as 6.5 million teens in the United States now have some hearing loss.
The surveys used largely similar questionnaires and standard hearing tests in which “any hearing loss” was defined as a loss of 15 decibels in at least one ear. That is, a person was determined to have some hearing loss if a tone had to be increased by 15 dB or more beyond the standard detection level to be heard at least half the time.
Hearing loss of 25 dB or greater is less common, particularly in children. But it also rose, from 3.5 to 5.3 percent, between the study time frames. The rate of hearing loss increased in high — but not low — frequencies, the researchers found.
This study wasn’t designed to ferret out the cause of hearing loss, says study coauthor Sharon Curhan, a physician and researcher at Harvard Medical School and Brigham and Women’s Hospital in Boston. While noise exposure is a known culprit, she says diet, medical care, lack of exercise and obesity might also play a role.
Oddly, when asked about their exposure to loud music, kids with good hearing didn’t give answers substantially different from those offered by kids with poorer hearing. But that may not tell the whole story.
“People underestimate their noise exposure,” Curhan says. A single brief noise can compromise hearing levels. Whether music delivered through headphones or “ear buds” plays a role in the increased hearing loss remains unknown, but the new findings may trigger research into those devices, she says.
Using family income data, the researchers also found that children living below the poverty line were more likely to have hearing loss than were kids above the line, but only in the 2005–2006 analysis. “One hypothesis is that poor people have more untreated middle ear infections,” says Yuri Agrawal, an otolaryngologist at Johns Hopkins University Medical School in Baltimore who wasn’t involved in the study. Such infections sometimes damage the inner ear and sabotage hearing, she says.
Or, she says, the poverty may result from poor hearing, not cause it. Families with mildly poor hearing that is genetically passed on to the children may be impoverished in part because hearing loss can interfere with education and achievement. “This can translate into less opportunity and lower income-earning potential,” Agrawal says.
Poverty-related hearing loss may not have shown up in the earlier years because a different poverty line cutoff point was used then, Curhan says.
While impaired hearing can hamper learning, it also takes an emotional and social toll, Curhan says. Kids who don’t hear well “miss subtle cues in peer-to-peer interactions and can be perceived as quirky or offbeat by not responding or because they respond inappropriately.”
“Our hope is that this study will raise awareness of hearing loss among adolescents because there are things they can do to limit the risk,” Curhan says.







