Thugs and Bugs
Cellular pathogens act like human criminals
From across the street, a man clad in a black suit surveys an office building. Several of his henchmen have just cut the building’s phone lines and scrambled its Internet and cell phone signals so that the workers inside have no way to summon help. Striding confidently, the man ducks into the building’s service elevator. After punching in a secret code—learned from covert surveillance—he easily slips inside the thick metal doors and zooms upward.
The elevator drops him off on the top floor, where he spies a young woman sitting in a nearby office. “Can I help you?” she asks.
He says, “The name is Coli. Edward Coli. I’m a friend of your boss.”
But before the assistant has time to dial her boss’ extension, the intruder injects her and then her boss and the floor’s other occupants with a chemical weapon. With these captives set to do his bidding, Coli’s conquest is complete.
Think this takeover artist is just a piece of fiction? Change Edward’s name to Escherichia, and you’ve got a different predator that shares elements of the modus operandi. A slew of findings shows that bacteria, viruses, and other pathogens cause infections with strategies similar to those that Edward and actual human criminals use.
With some laboratory detective work, scientists are discovering how various pathogens interact with their targets. New studies indicate that HIV scrambles cells’ communications so that they can’t summon help and that other viruses barge into a victim’s cells by short-circuiting their protective barriers. Separate research suggests that a worm called the root-knot nematode sneaks past plants’ defenses by disguising itself as a friend and that some bacteria inject one of a group of proteins that co-opt a cell’s actions.
“A lot of things that we know about in cell biology come from studies of interactions with pathogens,” says Jeffrey Bergelson of the Children’s Hospital of Philadelphia. The more that researchers learn about these true crimes, the better they’ll be able to prevent or stop them.
Communication scuttler
At least one virus devastates the immune system by silencing the immune components that sound an alarm when they detect a foreign invader. Normally, an encounter with a pathogenic virus or bacterium prompts these components, helper T cells, to ooze proteins that alert other immune cells to work together to vanquish the intruders. But helper T cells don’t issue their typical cry when they’re attacked by HIV, the virus that causes AIDS.
Some researchers had theorized that HIV silences the cell’s alarm when, to replicate itself, the virus tampers with a T cell’s DNA. But Yechiel Shai and Irun Cohen of the Weizmann Institute of Science in Israel and their colleagues had a different idea. They suspected that the virus might specifically suppress the T cells’ help signals, just as a human crook might cut a building’s phone lines.
In a study published in the August 2005 Journal of Clinical Investigation, the researchers focused on a snippet of a protein that makes up HIV’s viral envelope. This protein piece, called the fusion peptide, plays a pivotal role in merging HIV’s envelope with a T cell’s membrane, the first step in AIDS infection.
Shai’s team affixed glowing molecules to purified fusion peptide and then watched through a microscope to see where the peptide attached when it was mixed with rat T cells. It stuck to two specific cell-surface molecules: one called cluster of differentiation 4 (CD4) and the other, T cell receptor (TCR).
Since both molecules trigger the cascade of gene activity that summons other immune cells to the scene, Shai and his colleagues wondered whether fusion peptide was disabling CD4 and TCR. Sure enough, when the researchers injected the peptide into rats that had been inoculated with protein pieces from tuberculosis bacteria, which normally spur a strong immune system response, the animals’ T cells didn’t secrete the chemicals that call up other immune cells.
“When [fusion peptide] disrupts a T cell’s communication, there is no alarm and HIV gets inside the cell,” says Shai.
That’s bad news for a person fighting HIV, but fusion peptide may be useful as a target for anti-HIV drugs. It might also be redirected to dampen the immune system in autoimmune diseases such as rheumatoid arthritis, Shai suggests. In fact, when the researchers injected fusion peptide into rats with a form of arthritis, the severity of symptoms dropped by more than 50 percent.
Break-in artist
Some viruses seem to have figured out how to take advantage of a signal that sneaks them past strong protective barriers. Researchers have long known that people pick up group B coxsackieviruses (CVBs) through contaminated food or water. These microbes then travel to the intestines and pass into the epithelial cells that line the bowel wall. Once inside the intestines’ tough barrier system, the viruses can cause meningitis or an inflammation of the heart called myocarditis. In infants, they occasionally produce a fatal, systemwide infection.
How these viruses sneak through the intestines’ barrier was a mystery. Asymmetrical, oblong epithelial cells line the intestines. At the inside surface of the intestines, where they come into contact with digesting food and drink, the epithelial cells press snugly against each other to form a seal known as the tight junction.
To get inside the lining cells on their way to the rest of the body, CVBs need to attach to a cell-surface receptor that’s buried within the tight junction. However, CVBs are too large to squeeze through the gap.
To get a look at how CVBs slip into cells, Bergelson and his colleagues used a method similar to one with which Shai’s group studied HIV. The researchers attached glowing antibodies to some CVBs and then added them to human intestinal epithelial cells growing in a lab dish. Every few minutes, the team took a snapshot of the viruses, constructing a series of images while the infection took place.
The scientists report in the Jan. 13 Cell that CVBs, rather than heading straight to the tight junction, first attach to a protein on the surface of epithelial cells that’s easily accessible outside the barrier. The images showed that when a virus sticks to this decay-accelerating factor (DAF), those combination particles clump together and then travel toward the tight junction. Several minutes afterward, the snug link between the cells loosens enough for the virus to slip through.
“Clumping DAF seems to trigger a signal that moves the virus to the tight junction,” says Bergelson.
“Through evolution, variants of these viruses probably bound to lots of different things,” he notes. “The one that bound to DAF hit pay dirt because DAF seems to take it to the tight junction,” he says.
Scientists don’t know what role DAF plays in normal body processes. Learning more about DAF could offer new ways to stop CVBs and related viruses from using it to sneak into cells, Bergelson adds.
Sweet talker
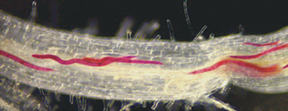
Some pests get into their victims by mimicking beneficial microbes. Root-knot nematodes are destructive little worms, measuring about 1.6 millimeters in length, that cause an enormous amount of damage to agricultural plants. They exact their toll—to the tune of $100 billion per year worldwide—by burrowing into plant roots, then forcing plants to supply them with nutrients. Eventually, the roots become grossly misshapen, impeding a plant’s uptake of water and nutrients from soil.
Since plants have strong defense systems to ward off other nefarious invaders, researchers have puzzled over why plants seem to invite root-knot nematodes inside. “Plants are defenseless against this pathogen—it’s their Achilles’ heel,” says David Bird, a plant pathologist at North Carolina State University in Raleigh, N.C.
In a study published in the Feb. 22, 2005 Proceedings of the National Academy of Sciences, Bird and his colleagues reported evidence backing up a new theory: Root-knot nematodes sweet-talk their way inside plants by pretending to be friendly bacteria called rhizobia.
For about 60 million years, peas, beans, and other legumes have been engaged in a close business relationship with rhizobia. Plants supply the bacteria with energy, and in exchange, rhizobia convert atmospheric nitrogen into a form that plants use to make proteins.
“To set up this partnership, two conversations need to go on,” says Bird. Plants secrete various signals called flavonoids that advertise their energy-supplying services, and in turn, rhizobia put out a chemical called NOD factor that identifies them as friends.
After plants check this natural security badge, tiny hairs on the plant roots become wavy and branched, then curl around the bacteria and welcome them inside.
Bird and his colleagues noticed that when they put root-knot nematodes near the roots of lotus plants, the root hairs branched and curled as if the roots had been introduced to rhizobia instead. Further investigation showed that plants encountering the nematodes activate the same genes that turn on in the presence of rhizobia. This result suggests that nematodes and the bacteria put off a similar—if not identical—signal.
“Our hypothesis is that through evolution, nematodes have learned about the detection system plants use for rhizobia and are exploiting it by secreting their own signal,” says Bird.
When his team introduced nematodes to plants that had been genetically altered to not recognize rhizobia’s NOD factor, the plants’ root hairs didn’t respond to the worms. Although these nematodes were only 10 percent as effective as normal ones in infecting plants, they didn’t fail completely at breaking into plant roots. “Nematodes seem to have lots of arrows in their quiver,” says Bird.
To reduce agricultural losses caused by this devious pathogen, researchers may need to figure out what other means the worms are using to disguise themselves and to find a way to stop plants from being fooled by the nematodes’ signals.
Weapon wielders
A common set of weapons seems to underlie the wide range of bacterial species that cause what’s broadly known as food poisoning. Salmonella, Shigella, and Escherichia coli aren’t closely related, and each exacts its illness in a slightly different way. However, recent research suggests that these bacteria use different members of a family of 24 related proteins to force cells in their hapless victims to act as the bacteria demand.
Pharmacologist Jack E. Dixon of the University of California, San Diego and his colleagues found this group of proteins when they were investigating a single protein, called Map, that’s pivotal in E. coli infections. Previous studies had shown that when this bacterium injects Map into cells, they respond by flexing their cytoskeletons, the internal fibers that set a cell’s shape and move around its contents. The researchers suspected that the motions induced by Map pull apart the tight junction between intestinal cells, causing diarrhea that spreads E. coli to new hosts.
Since Map seems so integral to E. coli infection, Dixon and his colleagues wondered whether other bacteria might inject related proteins into cells to carry out similar functions. To investigate this question, the researchers ran a computer search through databases of known bacterial proteins. “We basically asked ourselves, ‘What else looks like Map?'” Dixon says.
Eventually, the team came up with 24 candidate proteins, which bacteria tend to use in combination. All consist of a similar-length string of amino acids framed by tryptophan on one end and glutamate on the other. When the researchers injected these proteins into human cells growing in the lab, all of them seemed to act, as Map does, on the cells’ cytoskeletons.
However, each protein influenced the function of a different cytoskeletal part. “It’s like these proteins each contain a different zip code, and they’re getting shipped to different places in the cell,” says Dixon. For example, some proteins affected the fibers that shuttle nutrients and immune components around a cell, and others focused on the fibers that set the shape of the cell membrane. Dixon’s team is investigating how each of these actions increases a pathogen’s chance of survival.
Learning more about the mechanisms that these proteins use to seize control of a cell’s normal functions could lead to new ways of stopping the criminal behavior of many types of bacterial infections.
Notes Dixon: “If we can understand how these proteins function, it will give us a leg up on understanding how to combat them.”