The fluid part of semen plays a seminal role
An absence of seminal fluid produces signs of metabolic syndrome in male mouse offspring
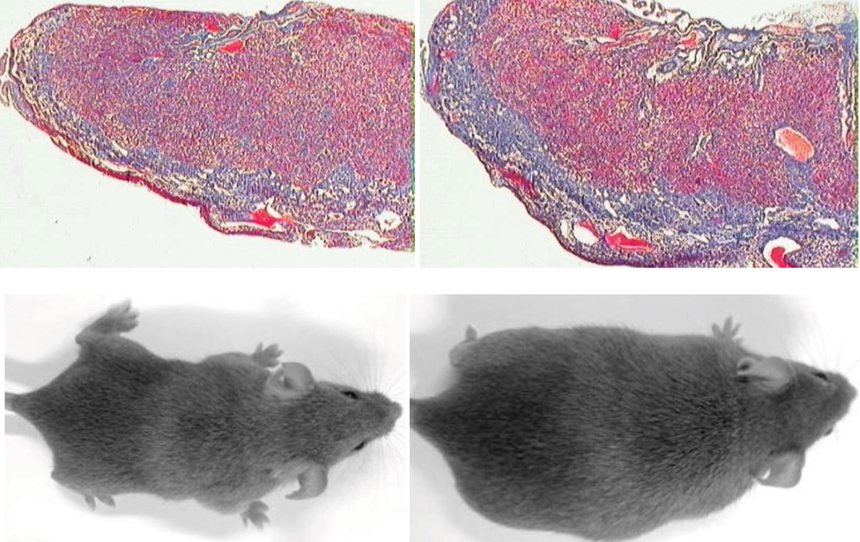
Offspring of male mice without seminal fluid had bigger placentas (top right) and increased body fat (bottom right) compared with offspring of normal male mice (left images).
J. Bromfield et al/PNAS 2014
Most of us remember that awkward class in school. It all starts with “when a man and a woman decide to make a baby…” and ends with some variation on birth control methods. Somewhere along the line, you’re shown a wriggling sperm diving into a waiting egg. And usually that’s the end of it. The sperm and egg are the most important parts. As far as you know, seminal fluid is just a swimming pool for sperm.
But it turns out that the fluid components of semen play a seminal role indeed. A new study in mice shows that without seminal fluid, fertility decreases. Not only that, the male offspring of this dry union end up with symptoms of metabolic syndrome. There is a conversation going on between the seminal fluid and the uterine environment, with long-term consequences for offspring. The results, published January 27 in the Proceedings of the National Academy of Sciences, suggest that the male contribution to conception and development is far more than a few swimming sperm.
Sarah Robertson, a reproductive biologist at the University of Adelaide in Australia, and her then-graduate student John Bromfield (now a reproductive biologist at the University of Florida) wanted to examine how seminal fluid could affect fetal development and the future the health of offspring long after sperm meets egg. So Bromfield carefully cut out the seminal vesicles of male mice. Without seminal vesicles, all the liquid is gone from the sperm swimming pool. With intact male mice, female mice conceived about 85 percent of the time. But when the mice without seminal vesicles mice mated with female mice, only around 30 percent of the females managed to conceive.
That wasn’t all. The females that did get pregnant by males without seminal vesicles showed changes through pregnancy and beyond. Their embryos showed developmental delays and had enlarged placentas. And after birth, the male offspring from these pregnancies were overweight, with increased body fat, higher blood pressure and other symptoms of metabolic syndrome.
The key appears to be seminal fluid exposure. The scientists showed that the female’s uterus responds to seminal fluid with increases in certain proteins called cytokines that promote an embryo’s development and survival. “This causes a more supportive environment for the embryo,” Robertson says. When seminal fluid is missing, cytokine levels decrease, and the promotion is gone.
The scientists also found that exposing the uterine tract to seminal fluid decreased Trail, a cytokine that usually induces cell death. In contrast, fertilization without seminal fluid increased Trail. So seminal fluid not only promoted cytokines that created a better environment for embryos to flourish, it also decreased levels of a harmful cytokine.
That seemed a bit off. After all, why should females have naturally higher levels of Trail, if Trail is potentially harmful to embryos? Robertson says that this challenges how scientists think that the female tract contributes to pregnancy. “We’ve always thought, isn’t the female always interested in getting pregnant?” But, she explains, “we need to turn that idea on its head. In fact, the female reproductive tract has a quality control function to prevent investment in pregnancy.” It could be a way for the female’s body to recognize a lower quality male by his lower quantity of seminal fluid.
Tracey Chapman, an evolutionary geneticist at the University of East Anglia in Norwich, England, says the paper is an exciting development. “The fact that molecules in seminal fluid can have striking effects on behavior and physiology has been known for a long time,” she says. But she says this paper is something new. “It’s quite a strong insight into new mechanisms,” she explains, “and it gives us new ways in which the early implantation environment is affected.”
Matt Dean, an evolutionary biologist at the University of Southern California in Los Angeles, agrees. “None of the previous studies had a direct link to any molecular mechanisms that might be going on,” he says. But he also wonders if there might be other changes, caused by the lack of seminal fluid, that contribute to the difference in fertility. He notes that without seminal fluid, male mice can’t secrete the proteins to form the usual copulatory plug. These plugs block a female’s vagina following mating (nothing tells other males to keep out like an inability to get in). He says that the proteins that form the copulatory plug might be one signal to the female reproductive tract that gets lost when there is no seminal fluid.
He also notes that the cytokines that Robertson and her colleagues examined are probably not the only ones involved. “There could be thousands of genes that are misregulated,” he says. One way to follow up, he suggests, might be to take some of these cytokines and manipulate them one by one without getting rid of the seminal fluid all together. This approach could help identify which molecules are most important for creating a comfortable uterine environment.
Seminal fluid varies from mouse to mouse. It also varies from human to human. Most studies of fertility focus on the sperm itself, looking at influences such as smoking, TV watching, pollution or nutrient consumption. It could be time to focus on seminal fluid as well. Robertson wants to use the results to encourage men to take care of their reproductive health.
They may have good reason. The male offspring in this study conceived in the absence of seminal fluid showed evidence of metabolic syndrome, a condition that persisted well into adulthood. This could be particularly important for children conceived by in vitro fertilization. During IVF, sperm are united with eggs and implanted into a woman without seminal fluid. If the findings in mice translate into humans, it may mean that children born via IVF are at increased risk for metabolic syndrome. But the findings may not move so cleanly into humans. Bromfield notes that studies of children born via IVF are “a mixed bag.” And most IVF babies are not yet old enough for signs of adult metabolic syndrome to be apparent. In the end, says Bromfield, “there’s haven’t been enough long-term studies to look at metabolic syndrome in those children.”
What is clear is that seminal fluid is far more than a proteinaceous liquid. It is a substance full of chemical signals entering into communication with the uterine tract. Proper communication leads to a supportive embryonic environment. Lack of seminal fluid means lack of communication. When this biological talk means the health of an embryo, the liquid in semen plays a seminal role, indeed.







