After West Nile Virus
What will it do to the birds and beasts of North America?
The alligators at Clabrook Farm were under the weather last fall. Some seemed depressed, others were wobbly, and a few crawled in circles. Within a few days of first showing such symptoms, alligators at the farm near Christmas, Fla., sank into neurological meltdown and died. During September and October,


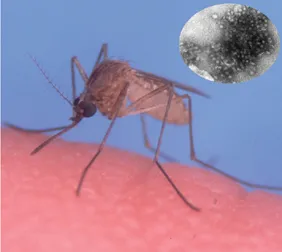

the farm lost about 300 of the 9,000 gators that it was raising for meat and hide.
In mid-October, one of the farm’s baffled owners took three of his sick hatchlings, to reptile veterinarian Elliott R. Jacobson of the University of Florida in Gainesville. Recognizing that they had some kind of brain malady, Jacobson ordered tests for West Nile virus and several other pathogens.
No North American alligator had ever been diagnosed with the infection, but then again North American alligators hadn’t had much of a chance to catch it. The virus was reported in the Western Hemisphere for the first time in August 1999 in New York City, where it caused a cluster of human cases of flulike symptoms, some of which turned into fatal brain inflammation. The first West Nile cases confirmed in Florida were a horse’s and crow’s demise reported in July 2001.
Moreover, people pick up the disease from the bite of an infected mosquito, so the notoriously tough-skinned alligators didn’t seem an obvious candidate for that infection route.
Yet when Jacobson tested the animals’ blood and organs, West Nile virus was evident. Although scientists are still debating how the North American alligator catches the disease, the species now appears on the official roster kept by the National Wildlife Health Center in Madison, Wis., that lists the more than 200 “species found positive for West Nile virus.”
This month, biologists report that the disease has reached birds in the Caribbean. A bananaquit in Jamaica has turned up with West Nile–virus antibodies in its blood, says Peter P. Marra of the Smithsonian Environmental Research Center in Edgewater, Md. This bird doesn’t migrate, so it must have caught the virus locally.
Because New World wildlife has not had to contend with the virus before, defenses aren’t in place. Some species are experiencing what appears to be an animal version of the epidemics of smallpox and other new diseases that devastated native peoples when Europeans arrived.
West Nile virus is hardly kind to its human victims. Of the 2,300 people in the United States known to have caught the virus in 2002, more than 4 percent died.
Wildlife mortality sometimes runs much higher. Two field studies of the American crow estimated local losses in New York and Oklahoma last year at 30 percent and 50 percent, respectively. In one lab test, crow mortality hit 100 percent.
Biologists are debating how such drastic mortality will affect the fauna of the Western hemisphere. Dozens of scientists presented data at a workshop in early February at the Smithsonian Environmental Research Center. The crows and other abundant species that are sustaining great losses worry the biologists less than the species with only small populations. However, as the fate of the farm alligators suggests, biologists are almost certainly in for plenty of surprises.
Potent pathogen
Greater travel and commerce in the modern world encourage the emergence of new diseases in animal populations, as well as among people, argues parasitologist Peter Daszak of the Consortium for Conservation Medicine in Palisades, N.Y. He sees the West Nile–virus invasion of the Western Hemisphere as an excellent example. “The surprising speed of its spread, its impact on human populations, and its impact on wildlife populations have caught many of us off guard,” Daszak said at the annual meeting the American Association for the Advancement of Science in Denver last month.
Scientists first recognized West Nile virus as a distinct organism in 1937, when they isolated it from the blood of a woman in the West Nile region of Uganda. The pathogen belongs to a family of viruses that can cause brain inflammation, such as Japanese encephalitis and North America’s St. Louis encephalitis. West Nile virus had spread through Africa, the Middle East, and the warmer parts of Europe and Asia before it landed in New York. Animals as well as people in the Old World can get the disease, but researchers–perhaps because they missed the initial invasion–haven’t documented big die-offs of animals there.
Geneticists have worked out the path that the virus probably followed to the New World. Comparing a particular section of the genome of the virus identified in the New York outbreak with that of viruses collected around the world, researchers found the New World invader to be virtually identical to a strain from a bird in Israel and distinctly different from the Far Eastern strains. They conclude that the Americas’ invader originated in the Middle East. How it got here remains uncertain, but researchers spin plenty of scenarios. An infected mosquito might have caught a plane ride to a New York airport, or a bird shipped either legitimately or smuggled might have brought in the infection.
After reaching New York about 4 years ago, the virus’ impact was small at first. During an outbreak, many people don’t even notice that they’ve been infected with the virus, and others just drag around with flulike symptoms for a few days. By the time the first New York outbreak subsided in the fall of 1999, however, doctors had confirmed 62 cases of severe illness and 2 deaths. The next summer brought a similar number of cases but more deaths and an expanded geography: 66 cases of severe illness and 9 deaths in the eastern United States.
The 2002 season was strikingly different, with 2,530 North American cases and 125 deaths. Also, the disease revealed some nasty twists in the way it’s transmitted. The Centers for Disease Control and Prevention (CDC) in Atlanta confirmed that three people acquired it from blood transfusions (SN: 1/25/03, p. 59: Available to subscribers at Getting the Bugs Out of Blood) and that a baby probably contracted the virus from its mother’s milk. Another infant appeared to have received the virus before it was born. By October, the disease had moved into 32 states and Washington, D.C.
With every surge in human disease, a wave hit wildlife, too (SN: 12/11//99, p. 378: http://www.sciencenews.org/sn_arc99/12_11_99/bob1.htm). By the end of 2002, the virus had struck a remarkable range of animals, including both dirt-common ones and nearly extinct species. It infected at least 186 wild and captive bird species, including pigeons, house sparrows, chickens, cardinals, mockingbirds, mallards, parakeets, peacocks, macaws, flamingos, bald eagles, and whooping cranes. The virus had also turned up in 17 other vertebrate species, including cats, dogs, chipmunks, striped skunks, bats, and alpacas.
The range of animals that pick up the virus and the breadth of its geographic spread have squelched any hope of getting rid of it. Even though it appeared in New York only 4 years ago, Daszak concludes, “West Nile virus is here to stay in North America.”
What’s the catch?
To start figuring out how the virus will transform wildlife of the Americas, researchers have been delving into the details of how animals pick up the virus.
Although biologists have known for decades that mosquitoes are an important carrier, it now looks as if mosquito bites don’t tell the whole story.
Mosquito transmission of viruses results from a quirk of the insect’s nutrition. A female mosquito needs to find a blood meal to provide nourishment for the big job of creating eggs. At the beginning of a cycle of egg making, she homes in on some unlucky hunk of walking nutrition, jabs in her sucking equipment, and dines.
If the nutrition provider carries at least a certain concentration of West Nile virus in its bloodstream, the mosquito picks up the virus, too. The next time she bites, some of the virus is transferred to her second victim’s blood.
What then happens to that animal depends on its species and the individual’s physical condition. Some animals get sick more readily than others do. From the start of the West Nile virus invasion of the United States, American crows have developed severe symptoms and died by the hundreds, dropping on roadsides and at least twice on the White House lawn. Yet health officials didn’t confirm that the disease had killed a single dog until September 2002, when an 8-year-old mixed breed died in Illinois.
Also, some species may get sick but not build up enough viruses in their blood to turn a biting mosquito into a disease spreader. Such dead-end hosts include people and adult chickens. Newly hatched chicks, however, transmit virus to a mosquito when bitten. And Jacobson now reports the high virus concentrations in the blood of North American alligators.
To identify particularly important species in the mosquito spread of West Nile disease, a research team let infected insects bite captive birds of 25 U.S. species. The five species that showed the highest virus concentrations in these tests–the “most competent reservoirs,” as epidemiologists put it–are widespread birds, Nicholas Komar of the CDC branch in Fort Collins, Colo., said at the recent Edgewater meeting. The list: blue jays, common grackles, house finches, American crows, and house sparrows.
That’s not good news. Abundant, broadly distributed reservoirs mean that mosquitoes are likely to happen upon a virus-hot meal and then spread the disease.
Komar and his colleagues also documented mosquito-free ways for birds to catch the virus. It passed by direct bird-to-bird contact in four species–blue jay, American crow, black-billed magpie, and ring-billed gull–Komar says. His team also observed birds in five species–great horned owl, common grackle, house finch, American crow, and house sparrow–picking up the virus just by eating a bit of infected flesh or even infected mosquitoes.
Biologists suspect that migrating birds are spreading West Nile virus. They are “excellent candidates,” says Marra, but “there has yet to be an actively migrating bird found with live virus.”
Sampling some 800 birds last fall in Alabama turned up no migrators that tested positive for West Nile virus, Jennifer Owen of the University of Southern Mississippi in Hattiesburg reported at the Edgewater meeting. Perhaps sick birds just don’t survive for long during the rigors of migration, or maybe they get too sick to even begin the journey.
In her presentation, she outlined a different approach to studying the interplay between migration and disease. She and her colleagues collected a total of 30 individuals from among gray catbirds, Swainson’s thrushes, and wood thrushes. By using artificial lighting to prolong day in the laboratory, the researchers plan to rev up the birds into migratory form. Then the team will expose some of the travel-ready birds to West Nile virus and see whether they lose the urge.
Bad spots
Even without many of the details of viral spread, researchers are starting to make some guesses about the ultimate impact of West Nile disease. The broadest data on bird populations come from the North American Breeding Bird Survey, which began in 1966. Since then, volunteers across the continent have spent one morning each June counting birds at prescribed roadside points along some 4,000 migration routes.
|
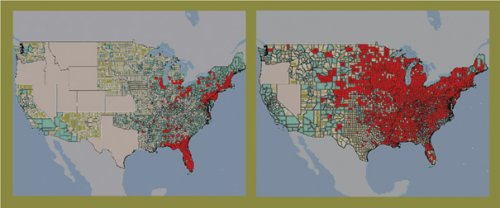
JUST ONE YEAR. West Nile virus may have started small in 1999, but it swept rapidly through the bird population between 2001 (left) and 2002 (right). Counties in which the virus turned up in birds are marked in red.
|
Marra and his USGS colleague John Sauer checked the survey for population declines as West Nile virus moved into a region. The researchers indeed found temporary declines in some areas but no overall decline for any species.
These and other data, have led Jeff Burgett of Hawaii’s Hakalau Forest National Wildlife Refuge to predict that West Nile virus won’t wipe out the American crow or other common species, despite their susceptibility to the disease. The virus may temporarily fell all individuals in some locales, but Burgett suspects that such species will hang on while they develop resistance to the disease.
Much more worrisome, he says, are the animal populations that are already small. Blast a hole in them, and there may be nothing left.
Burgett’s thoughts run to such scenarios because he works with endangered birds in Hawaii, where the West Nile virus hasn’t yet reached. He serves as recovery team leader for the endangered species called the Hawaiian crow. While mainland crows are falling out of the sky by the hundreds and yet surviving as a species, Hawaiians don’t have many crows to lose. Only 39 Hawaiian crows currently remain.
Other Hawaiian birds, such as the 20 or so diverse and colorful honeycreepers, face equally grim prospects if the disease hits, Burgett predicts. Roughly a third of the birds on the U.S. Endangered Species list live in Hawaii, so Burgett says that preventing the disease from reaching the islands is his top priority. “If we didn’t do anything about West Nile virus, the other things are moot,” he says.
Once the virus arrives in Hawaii, “there’s no conceivable program short of a neutron bomb that could keep it from becoming established.”
And the virus is moving toward him rapidly. “It took the Midwest in 1 year, and, bang, it’s in Seattle,” says Burgett.
He’s fighting hard, though. He notes that an obvious loophole through which the disease could reach the islands was the U.S. Postal Service policy of permitting shipments of live birds as first-class mail. Poultry chicks and gamecocks entering Hawaii in this way skipped the regular agricultural inspections. But Burgett led negotiations for increased protection. In the most promising step toward protecting Hawaii from West Nile disease so far, says Burgett, the post office last year stopped bird mail to the islands.
Daszak agrees that wherever they’re struck, small populations will suffer from West Nile virus. “There will be extinctions,” he says.
He, too, calls for more rigorous inspection and control of shipped birds, and he argues that it’s not just for this invading disease but the next one and the one after that.
****************
If you have a comment on this article that you would like considered for publication in Science News, send it to editors@sciencenews.org. Please include your name and location.
To subscribe to Science News (print), go to https://www.kable.com/pub/scnw/
subServices.asp.
To sign up for the free weekly e-LETTER from Science News, go to http://www.sciencenews.org/subscribe_form.asp.