Getting the Bugs Out of Blood
The quest for a zero-risk blood supply
Over the past few years, the crows in much of the Eastern United States fell silent. Many of the birds were victims of the emerging pathogen called West Nile virus. Originally from Africa, the virus entered the United States only a few years ago and is now spreading across the country in migrating birds (SN: 12/11/99, p. 378: http://www.sciencenews.org/sn_arc99/12_11_99/bob1.htm). The disease typically jumps from birds to people via mosquitoes. In September 2002, however, scientists with the Centers for Disease Control and Prevention (CDC) in Atlanta reported that a few people had been infected with West Nile virus through blood transfusions. That worries officials who recall the tragedies of the late 1970s and early 1980s, when thousands of people contracted HIV from contaminated blood products and later developed AIDS. While the West Nile virus usually causes few symptoms in people, it can trigger encephalitis and even death in elderly people and those with impaired immune systems (SN: 9/28/02, p. 197: Another Polio? Alarming West Nile fever risks emerge). The CDC findings are a reminder that despite elaborate screening procedures to eliminate pathogens from the blood supply, infections can still be transmitted through blood products.
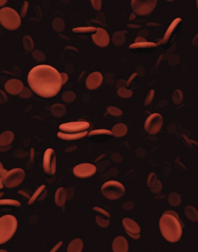
Blood banks test donated blood for syphilis bacteria and the viruses HIV, hepatitis B and C, and strains of human T-lymphotrophic virus that cause an unusual type of leukemia. They reject blood donors who have injected illicit drugs, engaged in homosexual sex, or traveled to areas where some of these diseases are widespread. Since such screening was introduced, the risks of becoming infected with these diseases through a blood transfusion have been reduced to less than a thousandth of what they had been, says Harvey Klein of the National Institutes of Health in Bethesda, Md.
But screening blood for these diseases won’t detect emerging viruses, such as West Nile. “What we’ve just seen with the West Nile virus really demonstrates the susceptibility of the blood supply to a new virus,” says Bernadette Alford of the Watertown, Mass.–based company Vitex. Developing screening tests for new diseases takes months, if not years. Several teams are already working on a test for West Nile virus.
Even more worrisome than West Nile virus is the prospect of another new disease–perhaps more deadly–spreading through the blood supply.
As a complement to screening, Alford and many other scientists are pursuing technologies that will eliminate, or at least reduce, a variety of pathogens that might get into the blood supply or therapeutic products derived from blood. Because there is such demand for blood, blood banks often separate it into components to be used for different purposes. Red blood cells carry nutrients and oxygen-carrying hemoglobin to tissues. Platelets are very small, cell-like components of blood that speed the clotting process by sticking to the lining of blood vessels. Plasma, the liquid in which blood cells are suspended, contains hundreds of proteins, some of which may be isolated into specific products such as the clotting factors used in treating hemophilia.
Since the early 1980s, researchers have developed chemical and heat treatments that inactivate a variety of pathogens in blood-derived proteins. But such treatments aren’t applicable to whole blood because they destroy red blood cells and platelets as well as inactivating some key proteins in plasma. Now, scientists are attempting to inactivate pathogens while not damaging either whole blood or its separated parts.
New methods of inactivating pathogens would be especially advantageous for reducing bacterial contamination of platelets, which are particularly vulnerable because they must be stored at room temperature, says Roger Dodd, president of the American Association of Blood Banks in Bethesda, Md. Though estimates vary, about 1 in 2,000 units of platelets is contaminated with measurable amounts of bacteria, and about 1 in 50,000 units has a high enough concentration of bacteria to trigger severe or life-threatening reactions in a person who gets a platelet transfusion.
Pathogen-reduction technologies would probably not significantly lessen the already low risk–less than 1 in a million–of catching currently recognized viral diseases from blood products, Dodd says. “The area which we feel most hopeful about, but for which there is least data, is the ability of such technologies to reduce the chance of new and emerging infections, like West Nile, from being transmitted in the blood supply,” he adds.
Protecting platelets and plasma
Some pathogen-fighting techniques damage the nucleic acids of genes and chromosomes to prevent infectious agents from replicating. Because mature red blood cells, platelets, and the other components of blood that are used therapeutically don’t have nuclei, they are unaffected by these methods. Such processes would destroy white blood cells, but for most transfusions, white blood cells are more likely to trigger unwanted immune reactions than to provide benefits.
Despite the effectiveness of nucleic acid damage at discriminating between useful blood components and pathogens, some physicians worry that introducing into patients even trace amounts of compounds that damage their genetic material would perhaps trigger cancers. There’s also a possibility that, like many drugs, these pathogen-inactivating compounds might have unexpected side effects in people.
Even very rare side effects would affect more people than do the current pathogens that slip through donor screening and blood testing. Since risk of bacterial contamination is greatest among platelet recipients, Klein says, pathogen-inactivation technologies should probably be tested in that blood product.
Another concern is that the treatment will lower the effectiveness of blood products, which are already in short supply. For example, treated cells might not function as well or survive as long in a transfusion recipient as untreated cells do. Such a difference could translate into a need for more transfusions. “Given the chronic shortage of platelets, this additional burden might overstress the system,” says James P. AuBuchon of Dartmouth-Hitchcock Medical Center in Lebanon, N.H. However, many researchers argue that a trade-off between blood-product effectiveness and safety would be acceptable.
Cerus Corp. of Concord, Calif., has already gotten approval in Europe to market a system for inactivating pathogens in platelets and plasma. The Cerus system uses flat molecules called psoralens–in particular, one dubbed S-59–that slip into double-stranded DNA and RNA. After workers add the product to a unit of platelets or plasma, they expose the unit to ultraviolet light. That activates the psoralen molecules so they bind to three of the DNA and RNA building blocks and encourages them to form abnormal bonds that essentially zip up the genetic material. That stops pathogens or white blood cells from reproducing. In a bag of platelets or plasma, the psoralens break down after a day, and an absorbent resin wafer in the bag removes the byproducts.
Over the past few years, researchers have shown that S-59 destroys many types of bacteria and viruses, including HIV and hepatitis viruses, says Laurence Corash, chief medical officer at Cerus. At the annual meeting of the American Association of Blood Banks in Orlando last September, Cerus scientists showed that the technology is also effective against some parasites, such as the one that causes most malaria.
However, Cerus studies showed a drop of 10 to 20 percent drop in platelet concentrations in blood treated with psoralens and ultraviolet light.
So far, the psoralen-treated platelets seem safe and reasonably effective in people, says Corash. Among 645 people with thrombocytopenia–a bleeding disorder in which a person has abnormally low concentrations of platelets–the half who got platelets treated with S-59 were no more likely to have episodes of bleeding than those who received normal platelets. However, 1 hour after a transfusion, the platelet count was lower in the patients receiving treated platelets than in those given untreated platelets, Corash reported last month at the American Society of Hematology meeting in Philadelphia.
In plasma, the technology is effective against the same pathogens, Corash adds. In the October 2002 Transfusion, he and his colleagues showed that in healthy volunteers who received a blood thinner for the purposes of the study, treated plasma and untreated plasma were equally effective in promoting blood clotting.
Another recent approach to purifying plasma and platelets uses riboflavin, or vitamin B2, plus ultraviolet light, says Ray Goodrich of the company Gambro BCT in Lakewood, Colo. Like the psoralens, riboflavin slips into genetic material and can cause abnormal bonds to form after exposure to ultraviolet light. “We’ve tested riboflavin against malaria, West Nile virus, herpes, intracellular viruses, and bacteria at levels hundreds of times higher than might be found [in blood products], and it’s effective,” Goodrich says. He and his colleagues presented some of these results at the September 2002 meeting of the American Association of Blood Banks. A benefit of using riboflavin, he says, is that it and its byproducts seem to be extremely safe.
AuBuchon notes that there are also nonchemical methods of addressing bacterial contamination. For example, he says, nurses could more carefully clean donors’ arms before inserting needles to obtain blood, and they could discard the first few drops of blood collected, which are the most likely to be contaminated with bacteria. Blood banks could test bags of platelets for bacteria and discard any bags that appear contaminated. “None of these approaches would harm platelets or put the recipient at risk,” says AuBuchon.
Red-cell and whole-blood safety
Red blood cells are the most widely used component of blood. Their bright color, contributed by the cells’ hemoglobin, poses a problem for some pathogen-reduction technologies that depend on ultraviolet light because the red blood cells absorb those wavelengths before they can activate the treatment chemical.
Goodrich and his colleagues are working with riboflavin in part because it jams up nucleic acids when exposed to either ultraviolet light or blue light, which isn’t blocked by red blood cells. Goodrich and his colleagues reported at the American Association of Blood Banks meeting that riboflavin plus blue light eliminated HIV and malaria from whole-blood samples.
In a different approach to sidestepping the light-absorption problem, scientists at Cerus have developed a psoralen-like compound that’s activated by acid instead of light. The compound, called S-303, is effective against a wide variety of pathogens, Corash reports. After activation, S-303, like the psoralens, forms abnormal bonds in DNA and RNA and then quickly breaks apart into unreactive chemicals, he says. Furthermore, mice injected with large doses of treated red blood cells for 26 weeks showed no sign of cancer or gene damage.
Vitex is developing a third approach to reducing pathogens in red blood cells. A chemical called PEN110 also slips into the nucleic acid guanosine in pathogens and causes the strand of genetic material to break. Subsequent washing of the red blood cells in saline removes PEN110.
As a bonus, says Vitex’s Alford, experiments have shown that the washing treatment used to eliminate PEN110 from blood also reduces or eliminates prions. These are abnormally folded proteins that seem to transmit Creutzfeldt-Jacob disease in people and disorders such as mad-cow disease in animals (SN: 11/30/02, p. 346: Mad Deer Disease?.). Washing red blood cells also clears away many immune globulins, which are proteins that cause a lung problem called transfusion-related acute lung injury. This side effect occurs once for every 5,000 transfusions.
In laboratory studies, PEN110 inactivates a wide range of pathogens including HIV, hepatitis, malaria, a relatively common parasite called babesiosis, and a notoriously tough virus called parvovirus B19. Alford reported at a CDC meeting last fall that the product can inactivate West Nile virus in whole blood.
So far, Vitex has completed two small safety studies of PEN110-treated blood given to people. A larger study is currently under way, Alford says. In includes people getting repeated infusions for sickle-cell anemia and thalassemia, as well as patients getting PEN110-treated transfusions during surgery. Neither the chemical nor the washing process seems to damage the red blood cells, she says. On the other hand, about 10 percent of the red blood cells in a unit of whole blood is lost during washing, which may lead to the need for additional transfusions in some people.
Safety tradeoffs
Finding West Nile virus in the blood supply was “a wake-up call” for the medical and blood-banking communities, says Klein. It underlined the need for pathogen-reduction technologies in whole blood and its components. All the newly developed methods inactivate West Nile virus. “If any of these technologies had been available and used, you wouldn’t have seen West Nile virus transmitted,” Klein says.
Nevertheless, Klein cautions, there’s no guarantee that any of them will eliminate all infectious agents. Some viruses have proved particularly resistant to inactivation. Also, in the earliest stages of infections, when a person hasn’t yet developed antibodies to the disease, blood viral concentrations can soar and might overwhelm a pathogen-reduction technology. Questions remain, too, about the cost that each of these technologies will add to blood products. “If we’re convinced that it’s safe, then we’ll use it,” says AuBuchon. “The Holy Grail of blood banking is a technology that will kill all the bugs and keep the cells intact.”
In the final analysis, “we need to be very careful that the benefits outweigh the risks,” says Klein. “But we’re not going to find anything that’s absolutely perfect. . . . After all, unlike most drugs, blood comes from an inherently unsafe source–you and me.”
****************
If you have a comment on this article that you would like considered for publication in Science News, please send it to editors@sciencenews.org.







