Alzheimer’s culprit may fight other diseases
Amyloid-beta protein attacks pathogens in mice, worms
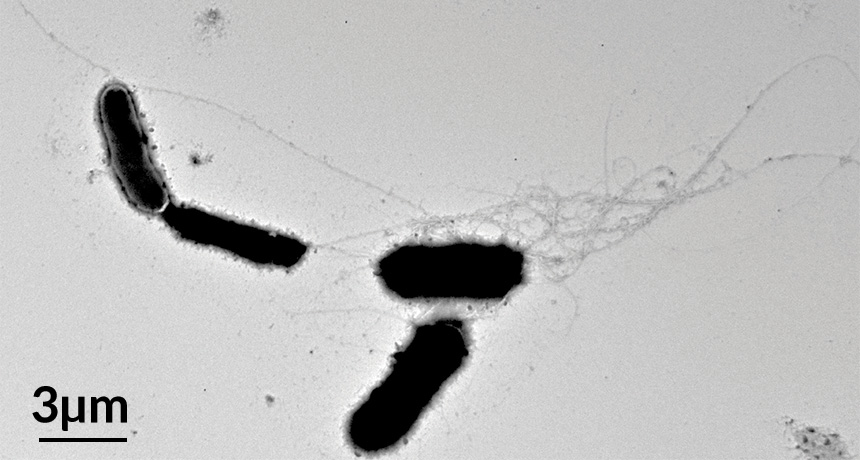
LOCKDOWN Strong A-beta fibrils ensnare dangerous yeast cells (black) in a dish, a defensive move that may serve as an important part of the immune system.
D.K.V. Kumar et al/STM 2016