Bacterial meningitis keeps falling
Vaccinations cut cases nearly one-third over past decade
Just a few decades ago, a pediatrician getting a frantic phone call from a parent whose child was running a high fever would immediately consider bacterial meningitis. Today, that diagnosis is unlikely: Vaccination against meningitis-causing bacteria has slashed incidence of the deadly brain inflammation, a nationwide survey shows.
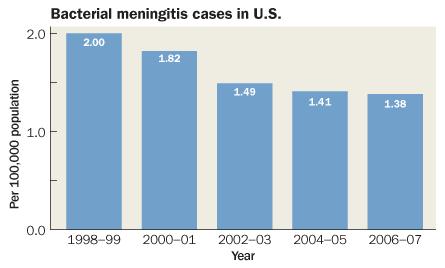
Researchers scanned data from more than 17 million people nationwide and found that bacterial meningitis incidence in the United States had fallen by 31 percent from 1998 to 2007, researchers report in the May 26 New England Journal of Medicine.
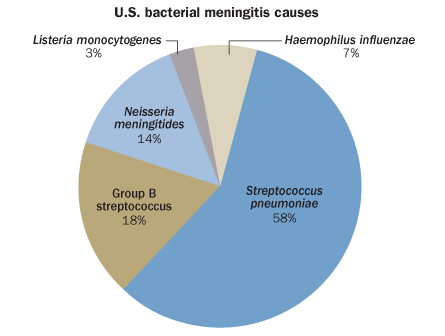
“For people taking care of kids since the 1980s, the world of meningitis has completely changed in the United States — and it’s because of two vaccines,” says Matthew Davis, a pediatrician at the University of Michigan Medical School who wasn’t part of the new study. Parents know these as Hib, the vaccine for Haemophilus influenzae type B, and PCV, for Streptococcus pneumoniae. These two microbes were historically among the chief causes of bacterial meningitis.
The first hit came in the 1980s and 1990s with the introduction of Hib, which remains a routine immunization for children. Then in 2000 the Food and Drug Administration approved a PCV vaccine called Prevnar-7 for S. pneumoniae, a microbe that can cause meningitis, pneumonia, ear infections and other ailments (SN: 4/7/07, p. 222).
That vaccine has reduced meningitis due to S. pneumoniae by 26 percent between 1998 and 2007, the new data show. A recently approved version of the vaccine will reduce cases further by broadening coverage to 13 strains of the bacterium, predicts study coauthor William Schaffner, a physician at Vanderbilt University School of Medicine in Nashville.
A third vaccine, aimed at another meningitis bacterium, Neisseria meningitidis, was also approved in recent years. Called the meningococcal vaccine, it is commonly given at the start of adolescence and as a booster for college freshmen.
The new study suggests that giving these vaccines to kids has also limited meningitis outbreaks among adults, who are now less likely to catch the microbes from youngsters, says study coauthor Cynthia Whitney of the Centers for Disease Control and Prevention in Atlanta. Screening pregnant women for another kind of strep has further reduced cases.
Bacterial meningitis is treated with antibiotics, but the inflammation that it causes in the membrane covering the brain and spinal cord can be lethal. Although the number of cases has dwindled, the fatality rate for bacterial meningitis in the nationwide sampling remained around 15 percent. Even wiping out the bacteria with antibiotics doesn’t rescue some patients if inflammation has already caused chemical imbalances, intracranial pressure and nervous system dysfunction, Schaffner says.
The authors estimate that 4,100 cases of bacterial meningitis occur annually in the United States.
Meningitis can also arise from viruses. While viral meningitis is more common than bacterial, it is less likely to be fatal unless a person has a weakened immune system. Viral meningitis can stem from infections with enteroviruses, which include polio and coxsackie viruses, or other common viruses.







