A blood test could predict the risk of Alzheimer’s disease
High-tech analysis picks up minuscule bits of amyloid-beta floating in plasma
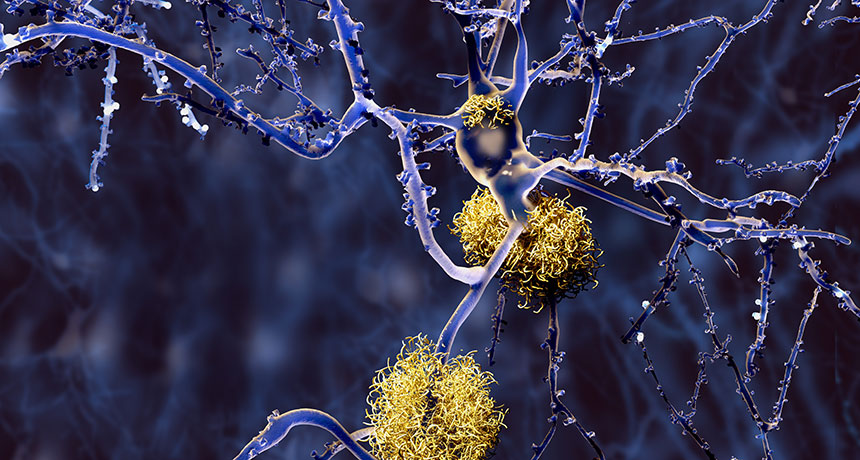
STICKY SITUATION Accumulations of a sticky protein called amyloid-beta (the tumbleweed-like balls in this illustration) can appear in the brain decades before a person develops Alzheimer’s disease.
selvanegra/iStockphoto






