Boosting estrogen, only in the brain
Selective transformation of protein into sex hormone could limit side effects
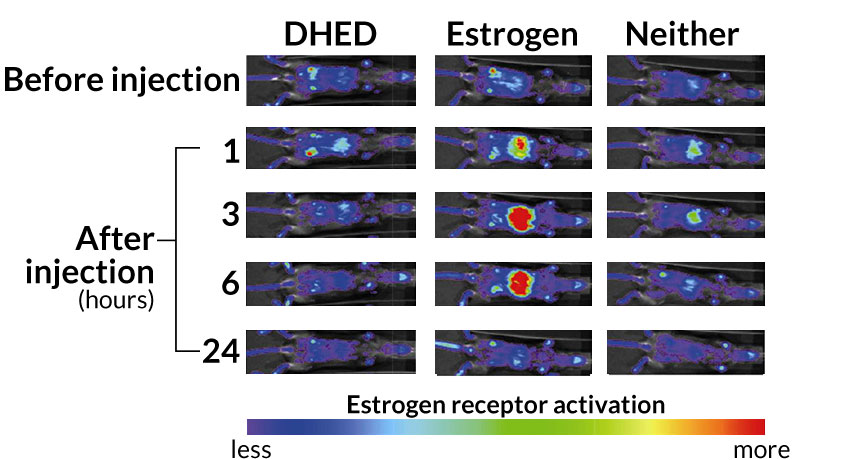
TARGETED EFFECT The chemical DHED produces the hormone estrogen in the brain, but not the body. In mice with tissues genetically modified to light up when exposed to estrogen, pure estrogen produces a bright glowing around the internal organs (center). But mice given DHED (left) do not light up more than untreated mice (right), indicating that DHED does not become estrogen in their bodies.
L. Prokai et al/Science Translational Medicine 2015