Brain holds more than one road to fear
Drug elicits anxiety-producing reactions in people without working amygdalae
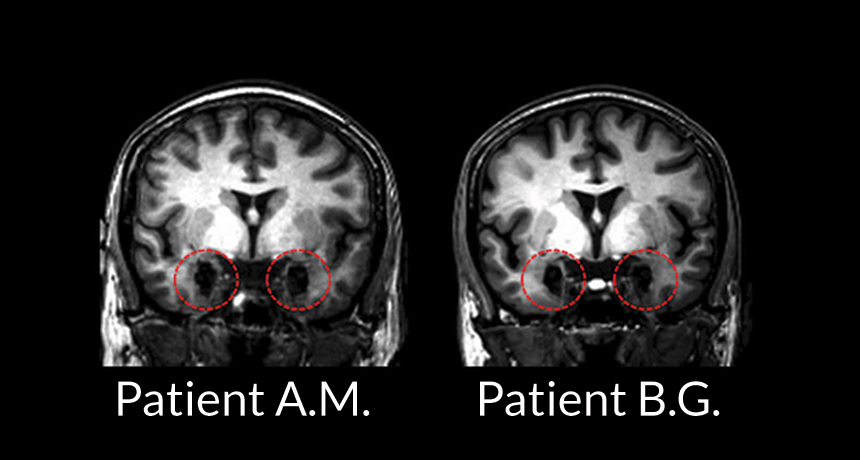
FEAR FACTORS Despite extensive damage in their amygdalae (red circles in these MRI scans), twin sisters A.M. and B.G. still can experience anxiety prompted by bodily cues, a new study shows.
S. Khalsa et al/Journal of Neuroscience 2016