City size and structure may influence influenza epidemics
New research could lead to more accurate predictions about flu seasons

FLU FORECAST The size and structure of a city can affect what kind of flu season its inhabitants will have, a new study finds.
Oregon State Univ., Jordan Masse on Unsplashed
A city itself influences the contours of its flu season – whether flu cases rise to a wintertime peak or plateau from fall to spring, new research suggests.
Flu cases generally peak in winter in certain areas of the United States because the air is drier. That dryness helps the flu virus survive longer once sneezed out of a sick person, for example, allowing the virus to potentially infect more people. But after analyzing data on flu cases reported from 2002 to 2008 in 603 U.S. cities, researchers have found that a city’s size and structure also play a role in shaping local flu epidemics.
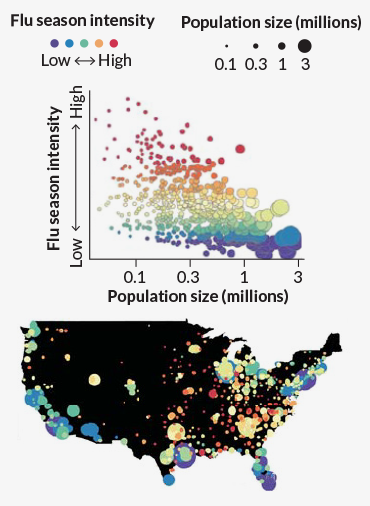
Larger cities with higher levels of crowding were associated with a steady accumulation of cases throughout a flu season. Smaller cities with less crowding tended to have a flu season with a more intense surge in winter, researchers report in the Oct. 5 Science.
“Understanding how the size and structure of cities impacts disease spread may help us to predict and control epidemics,” study coauthor and population biologist Benjamin Dalziel of Oregon State University in Corvallis, Ore., said October 2 at a news conference.
As the United States enters into its next flu season, memories of the previous one, which was especially severe, remain freshly in mind (SN: 7/7/18, p. 16). The U.S. Centers for Disease Control and Prevention just announced that the 2017–18 season killed 80,000 people (SN Online: 9/27/18).
A variety of factors are known to affect the transmission of the flu in a particular area, including humidity, the genetic changes flu viruses acquire and the ways that people interact as they move about their day. Dalziel and colleagues wondered how city size and structure fit into the mix.
The team found that in large cities that have more crowding — that is, concentrated areas where people live and work — there appear to be more opportunities for the virus to find new hosts, even when the air conditions aren’t ideal for virus transmission. So the flu spreads steadily during the season; the virus doesn’t need to wait for winter’s dry air.
But in smaller cities with less crowding, the air conditions seem to be the main driver of new cases, causing a spike in winter. Overall, cities with high-intensity flu seasons, in which cases rise to a peak, tended to be in the eastern part of the country and had wider seasonal fluctuations in humidity levels.
The study reveals “a relative difference in the timing of cases,” study coauthor and epidemiologist Cécile Viboud of the National Institutes of Health in Bethesda, Md., said at the news conference. It’s not that some cities are safer than others. “But those timing differences have important consequences” for health care systems in smaller cities, she said, which may become strained when dealing with a surge in flu cases.
The idea that the structure of cities and the kinds of interactions within them impact the stream of cases during a flu season needs to be tested further, says infectious disease researcher Jeffrey Shaman of Columbia University. But “if we’re seeing these patterns, we have to figure out why,” he says. Doing so could help researchers understand more about how flu is spread so that they “can do more to prevent its transmission.”