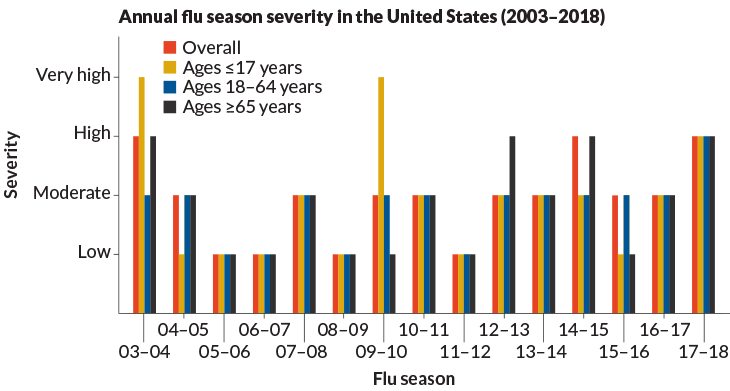
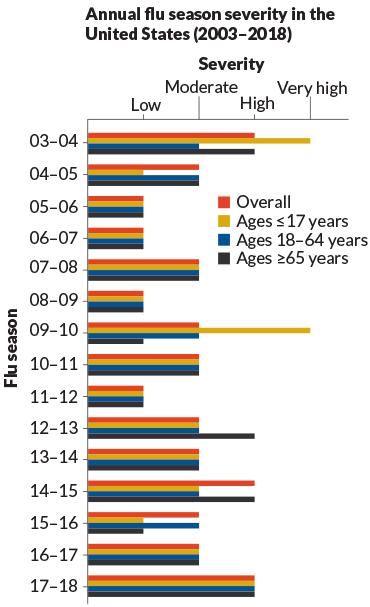
If you thought the most recent flu season was bad, you were right
The U.S. Centers for Disease Control and Prevention classed it in the ‘high severity’ category
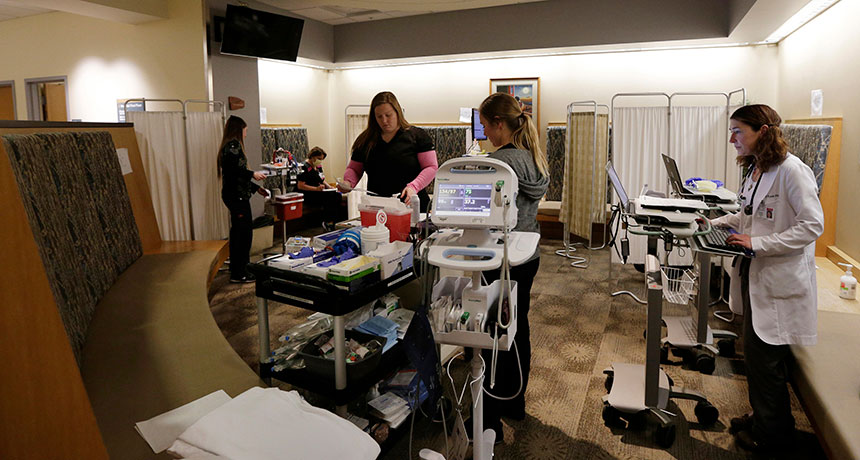
HIGH SEASON Last January, hospital staff saw patients in Bend, Ore., in a waiting area converted to manage more people coming in with the flu. The flu killed more than 170 children this season, the CDC reports.
Joe Kline/The Bulletin, AP