Defects in early immune responses underlie some severe COVID-19 cases
Genetic flaws and rogue immune responses can cause life-threatening disease, studies find
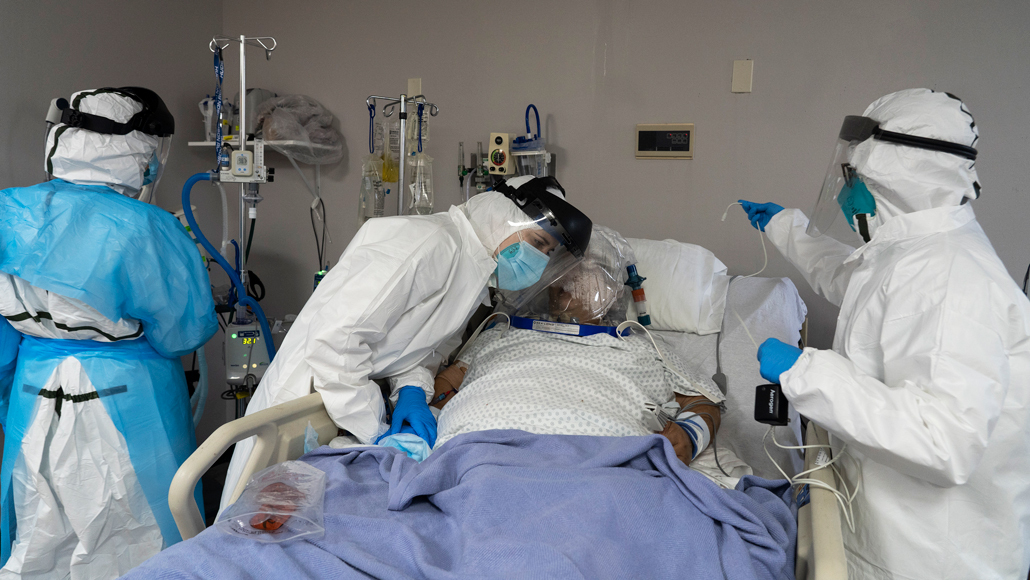
COVID-19 is a disease with wide-ranging symptoms, but it’s unclear why some people die or end up on ventilators — like the pictured ICU patient at Memorial Medical Center in Houston in July — while others never show signs of illness.
Go Nakamura/Getty Images
COVID-19 kills some people and leaves others relatively unscathed. But why? Age and underlying health conditions are risk factors, but scientists are trying to tease out other differences, including in people’s genes or immune systems, that may play a role.
Two new studies show that flaws in the body’s early response to viral infection, one caused by genetic defects and one by traitorous immune responses, are behind some severe COVID-19 cases.
In one study, published online September 24 in Science, researchers identified certain genetic defects in some people with severe COVID-19 that make the body produce fewer interferons, proteins that are part of the immune system’s early warning system. In other people with severe disease, however, the body’s own immune responses disable interferons, a second study published online in Science the same day finds.
These defects mean that the coronavirus that causes COVID-19, SARS-CoV-2, can infect cells without raising red flags, evading the usual onslaught of defenses brought on by interferons and leading to more severe disease, the researchers say.
The results add to growing evidence that strong early immune responses to COVID-19 are crucial to protect people from becoming severely ill (SN: 9/23/20). The findings may eventually lead to treatments that can better help those people who do get very sick, says Brianne Barker, an immunologist at Drew University in Madison, N.J., who was not involved in either study.
But “it’s really clear here that we can look at our severe patients and see that there’s not going to be a one-size-fits-all kind of treatment for them,” Barker says. For instance, while people with the genetic defects might benefit from receiving additional interferon early during an infection to boost their levels, those whose immune systems are going to mount a defense against the proteins would not.
It’s known that an overactive immune response to SARS-CoV-2 can do more harm than help. People with serious symptoms tend to have high levels of immune proteins linked to inflammation, a sign that the immune system failed to control the virus early during infection and is overcompensating in an effort to get it under control.
Interferons are a key part of the body’s early warning system (SN: 8/6/20). They alert uninfected cells that a virus of any type has invaded the body. In response to interferons, cells crank up protection measures that aim to curb viral replication. But in a minority of people with life-threatening COVID-19, there was a problem with that alarm system, the studies found.
“For [the researchers] to have found evidence of interferon being important in 14 percent of their severe patients is huge,” Barker says. It’s incredible to see one factor play such a large role in an infectious disease.
In one of the new studies, infectious diseases geneticist Jean-Laurent Casanova and colleagues analyzed the genetic blueprints of 364 patients who had been hospitalized with severe COVID-19. From another 295 critically ill people, the researchers examined smaller pieces of DNA that together form genetic messengers that help make proteins. For comparison, the team also analyzed 534 mildly symptomatic or asymptomatic people.
Of those 659 severely ill patients, 23 people had defects in immune genes that are involved in viral defense. Typically, the identified genes — known to play a role in life-threatening pneumonia caused by influenza — produce proteins that sense viral invaders or alert immune cells to begin making interferons. But flaws in some patients’ genetic code yield proteins that don’t work properly, causing the body to produce fewer interferons than usual. Experiments on cells in lab dishes and measuring interferon levels in blood show that people with these genetic defects didn’t produce many interferons.
In other people with severe COVID-19, the immune system turns against interferons themselves to cause severe disease, Casanova and his team found in the second study. Of 987 patients hospitalized with severe COVID-19, 135 people, or nearly 14 percent, had immune proteins in their blood that could attach to interferons.
In 101 severely ill patients, those immune proteins — called auto-antibodies because they recognize parts of the host rather than foreign invaders — could also stop interferon from activating other parts of the immune system. When researchers used plasma, the part of blood that contains antibodies, from eight patients with the auto-antibodies on lab-grown cells in dishes, the team found that the coronavirus could infect those cells even in the presence of interferon.
None of 663 people with mild or asymptomatic disease had those proteins. The team also tested blood samples taken from 1,227 people before the pandemic began and found that that only four people had auto-antibodies that recognized interferon.
In the severely ill patients, those auto-antibodies probably existed in their blood before they got sick, says Casanova, a Howard Hughes Medical Institute investigator at the Rockefeller University in New York City. There are several known autoimmune conditions, for instance, where people generate auto-antibodies that attach to interferon, including one called autoimmune polyendocrinopathy syndrome type I, or APS-1.
“The eureka moment came when we heard of three APS-1 patients with critical COVID-19, Casanova says. “That connected the dots and from there we tested [almost 1,000] patients.” Clinicians may be able to test for auto-antibodies to help determine who is at high risk for dangerous symptoms.
What’s more, the results may explain why men are more likely than women to become severely sick or die (SN: 4/23/20). Of the 101 people who had the auto-antibodies, 94 percent were men. The immune proteins may also increase by age: More than half of the people with auto-antibodies were older than 65.
The presence of auto-antibodies in some people may also present a problem for treatments like convalescent plasma (SN: 8/25/20). People who have recovered from a serious bout of COVID-19 tend to have higher amounts of antibodies that recognize the coronavirus in their serum, which is ideal for treating patients with such plasma. But if auto-antibodies that block interferon are also present in the plasma, that might thwart the interferon-related immune response in patients that receive them. “That means a lot of caution is needed, and a lot more studies need to be done with convalescent plasma,” Barker says.
Sign up for our newsletter
We summarize the week's scientific breakthroughs every Thursday.







