COVID-19 plasma treatments may be safe, but we don’t know if they work
Blood plasma from COVID-19 survivors can be used to treat hospitalized patients, FDA says
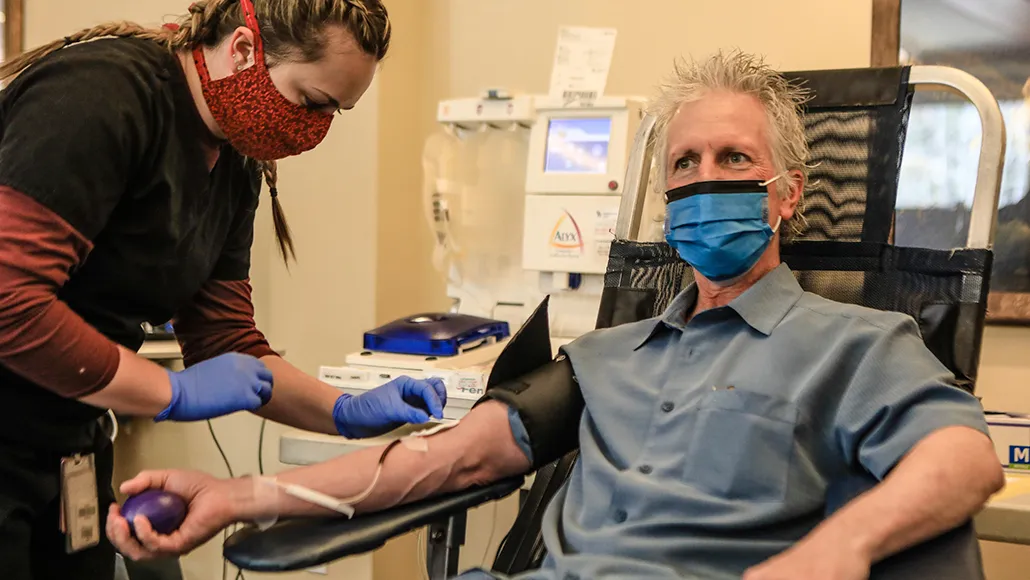
Patients who’ve recovered from COVID-19, like this man in Colorado, can donate their plasma to help those hospitalized by the coronavirus. The treatment, called convalescent plasma therapy, was authorized for emergency use by the FDA on August 23, though some experts worry the move is premature without controlled clinical trials.
Chris Dillmann/Vail Daily/Associated Press
With emergency permission for using plasma donated by recovered COVID-19 patients to treat sick ones, some researchers are once again raising concerns that the push for speed is getting ahead of the science.
No randomized controlled trials have shown that convalescent plasma works against COVID-19 yet. Even so, the U.S. Food and Drug Administration announced August 23 that it would allow convalescent plasma to be used under an emergency use authorization. That move has some experts worried that an unproven treatment may interfere with other more promising therapies, and may make it harder to find out if convalescent plasma really can help against COVID-19.
The authorization came less than a week after the New York Times reported that top National Institutes of Health officials were trying to stop an emergency use authorization for plasma, citing concerns about lack of sufficient data. On August 22, President Donald Trump tweeted dissatisfaction with the pace of FDA approval for new vaccines and therapies to fight COVID-19.
While convalescent plasma appears safe, and there are hints that it may help people in early stages of the disease, not enough data have been amassed to say that the treatment is effective, some experts warn.
“We lack the randomized controlled trial data we need to better understand its utility in COVID-19 treatment,” Thomas File Jr., president of the Infectious Diseases Society of America, said in a statement August 23. There’s a need “to better understand the benefits of convalescent plasma treatment before authorizing its wider use in patients with COVID-19.”
Here’s what the studies have told us so far about using convalescent plasma to treat COVID-19 patients and what we still need to learn.
What is convalescent plasma?
Convalescent plasma is the liquid part of blood taken from people who have recovered from an infection, in this case from COVID-19. Plasma contains antibodies that people have built against the pathogen.
It has been used for decades, with mixed success, to treat other types of infections, including influenza and Ebola. That’s why, early on in the coronavirus pandemic, it was eyed as a potential treatment (SN: 4/3/20).
In the United States, researchers set up clinical trials to test the safety and effectiveness of giving patients plasma from COVID-19 survivors; it has also been given in compassionate use situations, in which a person wasn’t able to join a clinical trial. Plasma from recovered COVID-19 patients has also been used in other countries as a possible therapy.
What does emergency use authorization mean?
Emergency use authorization gives physicians permission to use an experimental therapy in certain circumstances. It is not the same as FDA approval. There are no FDA approved therapies for COVID-19.
Under the new emergency use rules, researchers can still test convalescent plasma in clinical trials. Use of survivors’ plasma can also be extended to people with serious or immediately life-threatening COVID-19 who aren’t eligible for clinical trials. That was previously possible only for certain patients at select hospitals. But now, doctors in places that don’t normally have access to plasma can apply to get plasma for individual patients.
Emergency use authorization can be withdrawn, as was the case for hydroxychloroquine. The FDA rescinded emergency use authorization for the antimalarial drug in June after multiple studies found no benefit to using it (SN: 6/15/20).
Is convalescent plasma safe?
It’s generally considered safe for its standard uses. So far the evidence suggests that’s the case for treating COVID-19, says Liise-anne Pirofski, an infectious diseases physician and immunologist at Albert Einstein College of Medicine in New York City.
A study of 5,000 patients published June 11 in the Journal of Clinical Investigation found serious adverse events, such as allergic reactions or transfusion-related lung injury, occurred less than 1 percent of the time. Larger studies that haven’t yet been peer-reviewed showed similar results.
“The safety is the same as that of standard plasma, which is used every day in hospitals,” Pirofski says.
Does it work?
So far, there aren’t enough data to tell.
The idea is that patients who are ill with COVID-19 could benefit from the antibodies made by others who successfully fought off the virus.
The research that seems to have tipped the scales toward authorization of emergency use came from a preliminary study of 35,000 patients posted August 12 at medRxiv.org. At a news conference announcing the EUA, Trump said the study “has proven to reduce mortality by 35 percent. That’s a tremendous number.”
FDA commissioner Stephen Hahn added “what that means is, and if the data continue to pan out, 100 people who are sick with COVID-19, 35 would have been saved because of the administration of plasma.”
That number appears to come from a subset of the results, and misrepresents what the data actually say.
In a group of about 3,000 patients, researchers compared the mortality of patients who received plasma with high and low levels, or titres, of antibodies at different stages of illness. Of people who got plasma with high levels of antibodies, 8.9 percent died, on average, after seven days of treatment. That’s compared with the 13.7 percent of people who got plasma with low levels of antibodies who died in that time frame.
That study also suggested that earlier treatment was better. On average, 8.7 percent of people who got convalescent plasma within three days of being diagnosed with COVID-19 died within seven days. But waiting until four days or more after diagnosis to start convalescent plasma therapy was associated with 11.9 percent mortality in the seven-day window. That’s a relative difference of about 35 percent, but the absolute difference in mortality is much smaller, about 3.2 percentage points. In other words, about 3 in 100 people would be helped by convalescent plasma therapy here, not 35. Hahn acknowledged in a tweet August 24 that he conflated absolute and relative risk.
Looking out to 30 days after treatment, 21.6 percent of the early treatment group died compared with 26.7 percent of those who got treated later.

Trustworthy journalism comes at a price.
Scientists and journalists share a core belief in questioning, observing and verifying to reach the truth. Science News reports on crucial research and discovery across science disciplines. We need your financial support to make it happen – every contribution makes a difference.
What do other studies tell us?
There is still a lot to sort out.
Who should get access to the limited supply of plasma is a big issue. A study in the Netherlands found that most patients who have been ill for 10 days are already making their own antibodies against the virus. The study was testing convalescent plasma but stopped early because 53 of 66 patients in the study already had antibodies against SARS-CoV-2, the coronavirus that causes COVID-19. Researchers reported those preliminary results July 3 at medRxiv.org.
Adding additional antibodies probably won’t help those already producing their own, and plasma should be reserved for people who aren’t making antibodies yet, the researchers suggest. But other researchers studying convalescent plasma’s effect have not seen preexisting antibodies in most patients, says James Musser, an infectious diseases pathologist at Houston Methodist Hospital.
Not only do researchers need to determine whether convalescent plasma works for anybody, doctors and scientists also need to figure out who is likely to be helped, who won’t — and why. “We need to be able to direct our attention to which patients are most likely to benefit from, in this case, frankly, a relatively precious resource of high titre convalescent plasma,” Musser says.
In Houston, he and colleagues saw promising early results from a safety trial of convalescent plasma transfusions for hospitalized COVID-19 patients. But that early observation lacked a control group, so the researchers set up another study to compare groups of patients who got convalescent plasma with those who didn’t. Of patients in the study for whom 28 days worth of data are available, 145 patients got convalescent plasma while a control group of 435 did not. There was a trend toward less death in the group who got plasma, but that effect was not statistically meaningful, the researchers reported August 10 in the American Journal of Pathology.
When researchers broke the data down to look at people who got treatment within 72 hours of being admitted to the hospital and got plasma with high levels of antibodies, they saw a statistically meaningful difference. About 7 percent of those who didn’t get plasma died within 28 days of hospitalization, compared with 1.2 percent of patients who got plasma with high levels of antibody within a couple of days of hospitalization.
Those results also point to early treatment with high levels of antibodies being better. Exactly how much earlier is best is still not known. The group is conducting more analyses on all 316 patients who have gotten plasma treatment so far. Results should be available soon. But, Musser says, he and other scientists are waiting to see the results from randomized, controlled trials before coming to a decision about how well the treatment works, and for whom.
Will the emergency use authorization interfere with clinical trials?
It depends.
Hospitalized patients who don’t want to deal with enrolling in a clinical trial, or who don’t want to take a chance that they will be assigned to the placebo group, now have easier access to the treatment, which could mean researchers will have more trouble enrolling participants.
A coalition of researchers in the National COVID-19 Convalescent Plasma Project have set up at least 23 clinical trials testing survivors’ plasma for the ability to treat infections at various stages, or to preempt illness in those exposed to the virus as a preventive treatment. Those studies are either planned or ongoing, though recruiting adequate numbers of people has been challenging. Two studies out of Johns Hopkins University have enrolled only about 10 percent of the 500 to 600 volunteers needed.
“For inpatient studies, the EAU makes studying this treatment more difficult,” says Daniel Hanley, a physician who directs multisite clinical trials at Johns Hopkins.
But the emergency use authorization applies only to hospitalized patients. People with milder COVID-19 cannot get convalescent plasma therapy unless enrolled in a clinical trial. “The EUA may increase awareness of convalescent plasma as a treatment that seems pretty safe,” says Shmuel Shoham, an infectious diseases specialist at Johns Hopkins who is involved in clinical trials there. That could help recruitment for trials testing whether plasma therapy could be used as a prophylactic.
What don’t we know?
There’s still a lot researchers don’t know about how and when convalescent plasma therapy could be effective in treating, or preventing, COVID-19. Some evidence suggests that plasma with higher titres of antibodies are more effective, but more detailed information on how much plasma is needed for different patients would help clinicians, Pirofski says.
And the product itself can vary a lot — yet another factor that makes clinical trials challenging. Because people produce widely varying levels and types of antibodies after a COVID-19 infection, plasma taken from those people will also be different, says Suresh Vedantham, a clinical researcher who oversees COVID-19 trials at Washington University School of Medicine in St. Louis. “That’s a big X factor,” making it difficult to compare outcomes between patients treated with plasma from different donors.
Musser wants to know what went wrong for that 1.2 percent of patients in his study who got high levels of antibodies within 72 hours of hospitalization but still died. It’s also important to understand whether plasma can benefit people with health conditions that put them at greater risk of dying from COVID-19.
And researchers may need to compare plasma containing antibodies against SARS-CoV-2 with plasma that doesn’t contain those antibodies, Musser says. That would help determine whether there are other materials in plasma that help fight the infection, or if antibodies are really the active ingredient. If antibodies alone are important, it’s possible that giving purified monoclonal antibodies, which can be made in large quantities in labs, might be better than harvesting plasma from donors. Some studies of such monoclonal antibodies are also under way (SN: 2/21/20).
Researchers also still need to fully answer who benefits most from convalescent plasma treatment. Early evidence hints that plasma therapy works best in younger patients, but more data are needed. And while currently available data on efficacy were enough to authorize emergency use, scientists still only have a limited and fuzzy picture of just how much plasma therapy can help. Pirofski says it’s easier to feel confident about the answers to these questions when there are robust clinical trials with placebo controls.







