Some flu strains can make mice forgetful
Memory trouble and brain changes lingered months after infection
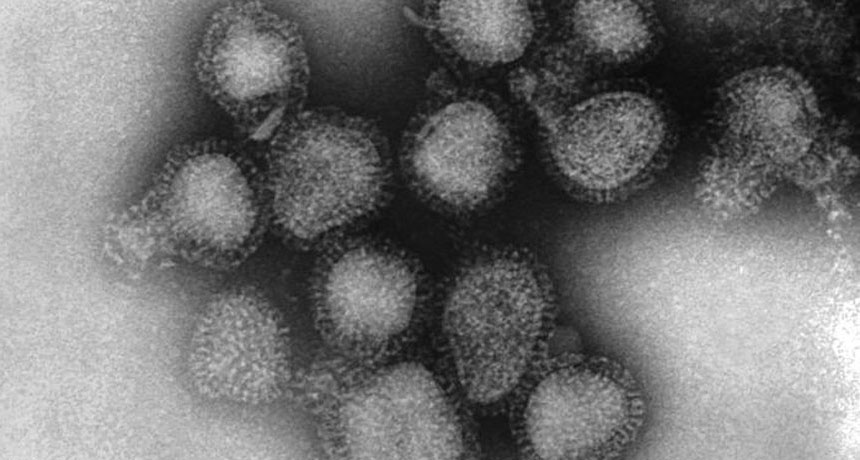
BRAIN DRAIN Certain influenza viruses, like the H3N2 strain shown in this transmission electron micrograph, can cause memory trouble and brain damage in mice months after infection, a new study shows.
Dr. Fred Murphy/CDC