Gum disease opens up the body to a host of infections
Mouth microbes have been implicated in a variety of ills, from arthritis to Alzheimer’s
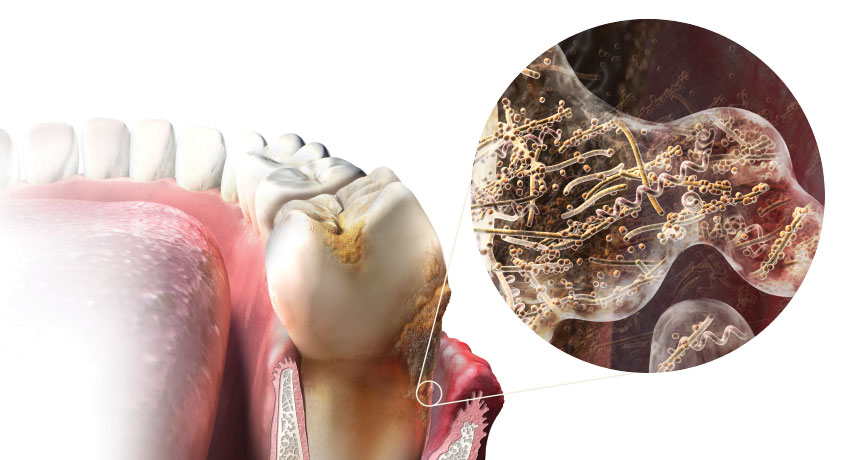
COMMUNITY BUILDING With inadequate brushing and flossing, bacteria caught between the tooth and gum coalesce into a biofilm. Eventually, oral tissue can deteriorate, allowing bacteria to infect other parts of the body.
Nicolle Rager Fuller
For centuries, the mouth and the body have been disconnected — at least when it comes to health care.